Featured Articles
What separates high- and low-performing hospitals in 2025

Hospital finances showed signs of improvement at the end of the second quarter, though notable performance gaps remain between higher- and lower-performing facilities, according to Kaufman Hall’s latest “National Hospital Flash Report,” published Aug. 11.
The median monthly operating margin index rose to 3.7% in June, up from 1.9% in May, though the pace of improvement remains uneven and somewhat unexpected amid recent market turbulence.
Hospitals in the Northeast and Mid-Atlantic reported the largest year-over-year increases in operating margins at 38%, followed by the South and Midwest at 29%. The West and Great Plains saw declines of 13% and 27%, respectively. Smaller and mid-size hospitals generally fared better than large facilities: hospitals with 26 to 299 beds saw margin gains between 17% and 30%, while those with more than 500 beds experienced a 29% decline.
“Higher performing hospitals are nimbler on both the revenue and expense sides,” Erik Swanson, managing director and data and analytics group leader at Kaufman Hall, said in a news release. “They may be expanding their outpatient footprint, diversifying services or managing expenses like purchased services by centralizing some functions. They are also more likely to have value-based care or bundled care arrangements in place.”
In 2025, top-performing hospitals are setting themselves apart from lower-performing facilities through a combination of strategic, operational and financial factors. According to Kaufman Hall and Fitch Ratings, the key differentiators include:
1. Strong market presence in growth regions: Hospitals located in expanding markets — especially in the South, Midwest and Northeast — are benefiting from rising demand, better payer mixes and stronger revenue potential. These organizations are leveraging local demographics and economic growth to drive performance.
2. Workforce recruitment and retention. Talent remains a key differentiator. High performers are more successful in hiring and retaining clinical and nonclinical staff amid national shortages, allowing them to maintain service capacity and quality care while controlling labor costs.
3. Aggressive payer strategy: Top-tier hospitals are skilled at negotiating favorable payer contracts, often using a “mind the gap” approach to keep reimbursement rates at the upper end of the scale. These hospitals maximize market leverage to drive revenue growth.
4. Operational agility: High-performing hospitals are nimble and can adjust quickly to changing conditions. They centralize purchased services, optimize supply chains and adapt care models to improve efficiency.
5. Investment in technology and infrastructure: Successful systems are proactively investing in AI, health IT and data analytics. These investments support care delivery and administrative efficiency and prepare hospitals for value-based care and alternative payment models.
6. Outpatient expansion and service diversification: Expanding outpatient footprints and diversifying service lines allow top hospitals to meet evolving patient demand and offset pressures on inpatient care, particularly in high-cost settings.
7. Proactive real estate and capital management. Strong performers are strategically managing real estate assets to bolster balance sheets and fund growth initiatives, such as facility modernization and digital transformation.
In contrast, lower-performing hospitals, often in rural or underserved regions, struggle with:
- Limited access to capital
- Declining patient volumes or poor payer mixes
- Severe staffing shortages
- High dependency on public reimbursement
- Little room for investment in innovation or infrastructure
Fitch warns that this divergence is becoming a “trifurcation” of hospital performance, with institutions separating into top-tier, middle-tier and lower-tier segments. Without strategic shifts, the financial gap may widen in the years ahead.
Top-performing hospitals will “have a predisposition to maximize that market essentially with annual payer negotiations, in a ‘mind the gap’ mentality that keeps them at the upper end of the payment scale,” Fitch said in a recent report.
Meanwhile, most hospitals are expected to remain in a middle band: operating sustainably but with limited margin growth and persistent staffing challenges. Those at the bottom of the scale face declining volume and payer mix issues and will likely need to rely heavily on outside cash to stabilize, according to Fitch.
The latest hospital financial reports indicate that 2025 performance gains are unevenly distributed, with the gap between top and bottom performers potentially widening as financial pressures persist.

How to Get a High Paying Contract Nursing Job
Contract nursing offers the chance to do meaningful work, gain diverse experience, and earn competitive pay. Whether you’re pursuing contract nursing jobs, per diem nursing positions, or rapid response assignments, the key to maximizing your income is preparation and strategy.
If you’re ready to secure a high-paying contract nursing job, use these proven tips to set yourself apart and negotiate pay that reflects your expertise.
Your resume is your first impression. A clear, polished resume highlights your skills, certifications, and professional accomplishments, and it determines whether you’ll be invited to interview.
Include:
- Your nursing specialties (such as ICU, emergency department, or medical imaging)
- Certifications (like ACLS, BLS, or specialty credentials)
- Details about your experience in different care settings, such as inpatient care, skilled nursing facilities, or acute care staffing
It’s normal to have employment gaps but be ready to confidently explain them during interviews. A well-organized resume positions you as a serious professional ready for high-paying nursing contracts.
Keeping your credentials updated makes you a more attractive candidate and can improve your earning potential.
Make sure to:
- Renew essential licenses and certifications promptly.
- Consider adding specialty certifications that are in demand for travel nursing jobs and contract assignments.
- Stay up to date with immunizations required by hospitals and clinics. Being ready with all documentation can speed up onboarding and help you access crisis response nursing jobs or urgent needs contracts that often pay premium rates.
The more prepared you are, the easier it is for a nurse staffing agency or recruiter to match you with higher-paying positions.
Professional references can be the deciding factor in landing a top-paying assignment.
Employers and recruiters rely on references to verify your:
- Clinical skills
- Professionalism
- Reliability
Choose references who can confidently speak to your work ethic and performance. Positive recommendations can open the door to flexible nursing shifts, per diem contracts, and specialized roles that pay more.
Flexibility is often rewarded in the world of contract nursing.
Consider these options to boost your pay:
- Accepting night shifts or weekends, which usually come with higher hourly rates.
- Taking assignments in locations experiencing shortages, such as rural facilities or emergency department nursing jobs.
- Being open to rapid response contracts or crisis response assignments, which often offer premium compensation.
When you demonstrate a willingness to adapt, you make yourself more valuable to medical staffing agencies and healthcare employers.
In contract nursing, your reputation follows you from one facility to the next. A strong track record makes it easier to secure higher-paying contracts and preferred assignments.
Tips for maintaining a great reputation:
- Be punctual and dependable.
- Communicate clearly with staffing agencies and supervisors.
- Go the extra mile to provide excellent patient care.
Facilities are willing to pay more to bring on nurses with proven reputations for excellence.
Being a contract nurse offers countless benefits, from career variety to premium pay. To make the most of your opportunities:
- Invest time in preparing a strong resume.
- Keep certifications and immunizations current.
- Maintain excellent references.
- Stay flexible with shifts and assignments.
- Build and protect your professional reputation.
When you combine preparation with dedication, you can consistently secure high-paying contract nursing jobs that match your skills and goals.
If you’re looking for your next opportunity, Staff Relief, Inc. is here to help. We partner with hospitals, clinics, and healthcare facilities to connect nurses with the best assignments in Georgia and beyond.
Contact us today to explore available contracts and start earning what you deserve.

Hiring More Nurses Generates Revenue for Hospitals
Underfunding is driving an acute shortage of trained nurses in hospitals and care facilities in the United States. It is the worst such shortage in more than four decades. One estimate from the American Hospital Association puts the deficit north of one million. Meanwhile, a recent survey by recruitment specialist AMN Healthcare suggests that 900,000 more nurses will drop out of the workforce by 2027.
American nurses are quitting in droves, thanks to low pay and burnout as understaffing increases individual workload. This is bad news for patient outcomes. Nurses are estimated to have eight times more routine contact with patients than physicians. They shoulder the bulk of all responsibility in terms of diagnostic data collection, treatment plans, and clinical reporting. As a result, understaffing is linked to a slew of serious problems, among them increased wait times for patients in care, post-operative infections, readmission rates, and patient mortality—all of which are on the rise across the U.S.
Tackling this crisis is challenging because of how nursing services are reimbursed. Most hospitals operate a payment system where services are paid for separately. Physician services are billed as separate line items, making them a revenue generator for the hospitals that employ them. But under Medicare, nursing services are charged as part of a fixed room and board fee, meaning that hospitals charge the same fee regardless of how many nurses are employed in the patient’s care. In this model, nurses end up on the other side of hospitals’ balance sheets: a labor expense rather than a source of income.
For beleaguered administrators looking to sustain quality of care while minimizing costs (and maximizing profits), hiring and retaining nursing staff has arguably become something of a zero-sum game in the U.S.
But might the balance sheet in fact be skewed in some way? Could there be potential financial losses attached to nurse understaffing that administrators should factor into their hiring and remuneration decisions?
Research by Goizueta Professors Diwas KC and Donald Lee, as well as recent Goizueta PhD graduates Hao Ding 24PhD (Auburn University) and Sokol Tushe 23PhD (Muma College of Business), would suggest there are. Their new peer-reviewed publication* finds that increasing a single nurse’s workload by just one patient creates a 17% service slowdown for all other patients under that nurse’s care. Looking at the data another way, having one additional nurse on duty during the busiest shift (typically between 7am and 7pm) speeds up emergency department work and frees up capacity to treat more patients such that hospitals could be looking at a major increase in revenue. The researchers calculate that this productivity gain could equate to a net increase of $470,000 per 10,000 patient visits—and savings to the tune of $160,000 in lost earnings for the same number of patients as wait times are reduced.
“A lot of the debate around nursing in the U.S. has focused on the loss of quality in care, which is hugely important,” says Diwas KC.
But looking at the crisis through a productivity lens means we’re also able to understand the very real economic value that nurses bring too: the revenue increases that come with capacity gains.Diwas KC, Goizueta Foundation Term Professor of Information Systems & Operations Management
“Our findings challenge the predominant thinking around nursing as a cost,” adds Lee. “What we see is that investing in nursing staff more than pays for itself in downstream financial benefits for hospitals. It is effectively a win-win-win for patients, nurses, and healthcare providers.”
To get to these findings, the researchers analyzed a high-resolution dataset on patient flow through a large U.S. teaching hospital. They looked at the real-time workloads of physicians and nurses working in the emergency department between April 2018 and March 2019, factoring in variables such as patient demographics and severity of complaint or illness. Tracking patients from admission to triage and on to treatment, the researchers were able to tease out the impact that the number of nurses and physicians on duty had on patient throughput. Using a novel machine learning technique developed at Goizueta by Lee, they were able to identify the effect of increasing or reducing the workforce. The contrast between physicians and nursing staff is stark, says Tushe.
“When you have fewer nurses on duty, capacity and patient throughput drops by an order of magnitude—far, far more than when reducing the number of doctors. Our results show that for every additional patient the nurse is responsible for, service speed falls by 17%. That compares to just 1.4% if you add one patient to the workload of an attending physician. In other words, nurses’ impact on productivity in the emergency department is more than eight times greater.”
Adding an additional nurse to the workforce, on the other hand, increases capacity appreciably. And as more patients are treated faster, hospitals can expect a concomitant uptick in revenue, says KC.
“It’s well documented that cutting down wait time equates to more patients treated and more income. Previous research shows that reducing service time by 15 minutes per 30,000 patient visits translates to $1.4 million in extra revenue for a hospital.”
In our study, we calculate that staffing one additional nurse in the 7am to 7pm emergency department shift reduces wait time by 23 minutes, so hospitals could be looking at an increase of $2.33 million per year.Diwas KC
This far eclipses the costs associated with hiring one additional nurse, says Lee.
“According to 2022 U.S. Bureau of Labor Statistics, the average nursing salary in the U.S. is $83,000. Fringe benefits account for an additional 50% of the base salary. The total cost of adding one nurse during the 7am to 7pm shift is $310,000 (for 2.5 full-time employees). When you do the math, it is clear. The net hospital gain is $2 million for the hospital in our study. Or $470,000 per 10,000 patient visits.”
These findings should provide compelling food for thought both to healthcare administrators and U.S. policymakers. For too long, the latter have fixated on the upstream costs, without exploring the downstream benefits of nursing services, say the researchers. Their study, the first to quantify the economic value of nurses in the U.S., asks “better questions,” argues Tushe; exploiting newly available data and analytics to reveal incontrovertible financial benefits that attach to hiring—and compensating—more nurses in American hospitals.
We know that a lot of nurses are leaving the profession not just because of cuts and burnout, but also because of lower pay. We would say to administrators struggling to hire talented nurses to review current wage offers, because our analysis suggests that the economic surplus from hiring more nurses could be readily applied to retention pay rises also.Sokol Tushe 23PhD, Muma College of Business
For state-level decision makers, Lee has additional words of advice.
“In 2004, California mandated minimum nurse-to-patient ratios in hospitals. Since then, six more states have added some form of minimum ratio requirement. The evidence is that this has been beneficial to patient outcomes and nurse job satisfaction. Our research now adds an economic dimension to the list of benefits as well. Ipso facto, policymakers ought to consider wider adoption of minimum nurse-to-patient ratios.”
However, decision makers go about tackling the shortage of nurses in the U.S., they should go about it fast and soon, says KC.
“This is a healthcare crisis that is only set to become more acute in the near future. As our demographics shift and our population starts again out, demand for quality will increase. So too must the supply of care capacity. But what we are seeing is the nursing staffing situation in the U.S. moving in the opposite direction. All of this is manifesting in the emergency department. That’s where wait times are getting longer, mistakes are being made, and overworked nurses are quitting. It is creating a vicious cycle that needs to be broken.”
Goizueta faculty apply their expertise and knowledge to solving problems that society—and the world—face. Learn more about faculty research at Goizueta.
*Ding, Tushe, Kc, Lee: “Frontiers in Operations: Valuing nursing productivity in emergency departments.” Manufacturing & Service Operations Management 26:4:1323-1337 (2024)
Georgia could see the largest shortage of RNs by 2036
Staffing is one of the biggest issues facing ASCs. A 2023 survey from ORManager found that in the last 12 months, 56% of ASCs reported an increase in volume. Despite this success, 68% of facilities also reported having a more difficult time recruiting experienced operating room nurses.
“I think the biggest threat towards ASCs in 2023 is staffing, especially qualified, experienced staffing in all areas of an ASC, including business office, pre-op, OR (both nursing and surgical technicians), post-anesthesia care unit and recovery nurses. In addition, sterile processing technicians,” Michael Powers, administrator of Knoxville, Tenn.-based Children’s West Surgery Center, told Becker’s. “Each of these areas require a certain set of skills that are acquired and honed over time. There is increased competition, and in fact it is hard to compete with large health systems/hospitals. I am also finding that ASCs are competing in the same region against one another for the available staffing pool.”
The HRSA report highlights nurse workforce projections from 2021 to 2036 generated using the agency’s health workforce simulation.
Here are the five states with the largest projected shortages of registered nurses by 2036, per the report:
1. Georgia: 29% projected shortage
Projected vacancies: 34,800
2. California: 26% projected shortage
Projected vacancies: 106,310
3. Washington: 26% projected shortage
Projected vacancies: 22,700
4. New Jersey: 25% projected shortage
Projected vacancies: 24,450
5. North Carolina: 23% projected shortage
Projected vacancies: 31,350
https://www.beckersasc.com/leadership/5-states-facing-the-biggest-nurse-shortages-by-2036
Breaking News
Where are Leapfrog’s 5 ‘F’ hospitals?
Five U.S. hospitals have received an “F” safety grade from The Leapfrog Group for spring 2026.
Leapfrog calculates hospital safety grades using up to 22 CMS patient safety measures, data from the Leapfrog Hospital Survey and supplemental imputation. Read more about Leapfrog’s methodology here.
For spring 2026, safety grades were not assigned to the 450 hospitals that did not participate in the Leapfrog Hospital Survey in 2024 or 2025.
The move comes after five Palm Beach (Fla.) Health Network hospitals — part of Dallas-based Tenet Healthcare — filed a lawsuit against Leapfrog after receiving “F” and “D” safety grades. In March, a federal judge ruled the hospitals were deliberately punished with artificially low scores for not participating in the voluntary Leapfrog Hospital Survey. Under the ruling, Leapfrog was required to withdraw the five hospitals’ safety grades for fall 2024, spring 2025 and fall 2025 from its websites and send corrective disclosures to all entities that paid to license those grades.
“Although the court ruling only applied to five hospitals, Leapfrog does not apply programmatic changes to individual hospitals because the hospital safety grade is a national program. We expect to resume full grading in fall 2026,” Leapfrog said in a May 6 news release.
Hospitals have pushed back on Leapfrog’s safety grades for years, arguing the methodology is flawed and unfairly penalizes hospitals that do not participate. Two hospitals filed similar lawsuits in 2017 and 2019, though the cases were eventually dismissed.
In previous years, the “F” list has included more than a dozen hospitals.
Here is the most recent list:
Illinois
Roseland Community Hospital (Chicago)
Mississippi
South Central Regional Medical Center (Laurel)
West Virginia
CAMC Teays Valley Hospital (Hurricane)
Weirton Medical Center
WVU Fairmont Medical Center
See the list of Leapfrog’s 11 “A” hospitals here.
The post Where are Leapfrog’s 5 ‘F’ hospitals? appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Nurses fret AI overreliance could erode care, call for more guardrails
As U.S. nurses increasingly employ AI in their day-to-day tasks, the American Nurses Association is advocating for more nurse-led guardrails amid concerns of bias, unclear accountability and a decline in professional judgement.
On April 22, the ANA hosted an invitation-only “AI in Nursing Practice Think Tank” for nursing leaders to discuss how AI is affecting the profession and what safety protocols should be implemented.
According to a consensus summary, nursing leaders identified five areas of concern:
- Erosion of professional judgement and critical thinking: “Poorly designed or rapidly deployed tools may diminish nurses’ ability to see the whole patient, question outputs and exercise professional reasoning.” They also voiced worries about overreliance and automation bias.
- Unclear accountability and liability: Nursing leaders are concerned about responsibility when AI tools influence care decisions. A common concern was fear of licensure exposure.
- Bias that worsens equity and trust: Patient safety could be at risk if AI tools have algorithmic bias or incorrect data, leaders said.
- Cognitive burden and workflow harm: Even if an AI is designed to alleviate workload, a poor rollout can negatively affect cognitive burden.
- Lack of nursing-specific governance and standards: Most AI frameworks do not specify nursing and are not applicable to practices at the bedside, in education or decision-making.
In its May 5 report, the ANA — which represents more than 5 million U.S. nurses — recommended five action items to address these concerns:
- Issuing clear, nurse-led guardrails
- Curating a nursing AI playbook
- Advancing AI literacy and competence
- Strengthening policy and regulatory advocacy
- Sustaining robust cross-sector collaboration
Access the report here.
The post Nurses fret AI overreliance could erode care, call for more guardrails appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Fatality risk grows 8% per added med-surg nurse patient: Study
For every additional patient assigned to a medical-surgical nurse in Pennsylvania, there is an associated 8% increase in fatality risk within 30 days, according to a study published April 30 in Medical Care.
The study analyzed outcomes of nearly 550,000 medical and surgical patients who received care at a Pennsylvania hospital in 2022 or 2023. More than 2,700 direct care nurses were included in the study, which compared patient outcomes to med-surg nurse staffing ratios.
Researchers at the Philadelphia-based University of Pennsylvania’s nursing department conducted the study, as well as several others focused on nurse-to-patient ratios. In Pennsylvania hospitals, unit-specific plans govern staffing rather than mandated ratios.
Across 132 Pennsylvania hospitals, each additional patient assigned to a nurse was associated with 8% higher odds of patient death within 30 days, 4% higher odds of hospital readmission and 2% increase in length of stay, the study found.
Hospital nurse staffing varies from three to nine patients per nurse in Pennsylvania, according to a May 5 news release from Penn Nursing. The study found an average of 5.9 patients per med-surg nurse, which researchers said is a high workload that can worsen outcomes and employee well-being.
Each additional patient per nurse was associated with 33% higher odds of increased nurse burnout, 43% higher odds of job dissatisfaction and 27% higher odds of intent to leave, according to the study.
If hospitals imposed a 4-to-1 nurse-to-patient ratio in med-surg units, the researchers estimate Pennsylvania hospitals could annually save $66 million due to lower turnover. They also predicted 70,000 fewer hospital days — aka, lower length of stay — resulting in more than $239 million in savings per year.
“[H]ospital variation in nurse staffing is quite consequential for whether patients survive their hospital stay,” the researchers concluded. “Our study and others suggest that nurse understaffing is associated with turnover and setting minimum safe nurse staffing is a direct intervention to reduce understaffing.”
The post Fatality risk grows 8% per added med-surg nurse patient: Study appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 hiring ‘hot spots’ for new graduates
Birmingham-Hoover, Ala., is the top U.S. metropolitan area for college degree holders in their 20s, according to a study from payroll provider ADP.
ADP analyzed anonymized payroll data from more than 209,000 Americans ages 20-29 at more than 20,000 U.S. employers from January 2025 to January 2026, according to the analysis, which was published May 3. The study ranked 53 U.S. metropolitan areas with at least 1 million residents, grading them on wages, hiring and cost of living.
The metropolitan areas were ranked based on their combined percentile across annual wage estimates, nation-to-metro cost of living ratio, affordability-adjusted annual wage and hiring rates.
Below are the 10 top-ranked metropolitan areas, along with their combined percentile rank:
1. Birmingham-Hoover, Ala. — 100
2. Tampa-St. Petersburg-Clearwater, Fla. — 98
3. San Jose-Sunnyvale-Santa Clara, Calif. — 96
4. Columbus, Ohio — 94
5. Raleigh, N.C. — 92
6. Tulsa, Okla. — 90
7. San Francisco-Oakland-Hayward, Calif. — 88
8. Nashville-Davidson-Murfreesboro-Franklin, Tenn. — 87
9. Charlotte-Concord-Gastonia, N.C. — 85
10. New York City-Newark-Jersey City, N.J. — 83
The post 10 hiring ‘hot spots’ for new graduates appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Georgia hospital names Atrium Health Navicent Baldwin COO as CEO
Thomas “Tog” Goss, MSN, RN, was appointed CEO of Putnam General Hospital in Eatonton, Ga., effective June 1.
Mr. Goss will join Putnam General from Atrium Health Navicent Baldwin, a 140-bed acute care hospital in Milledgeville, Ga., where he serves as COO, according to a hospital news release. Atrium Health Navicent, based in Macon, Ga., is part of Charlotte, N.C.-based Advocate Health, which operates a network of hospitals and affiliates across central Georgia, including Navicent Baldwin. Putnam General is affiliated with the Navicent network.
He will succeed Alan Horton, who is retiring after 12 years as CEO and nearly 50 years in hospital leadership.
Mr. Goss has a clinical and operational background, with experience as an emergency medical technician, registered nurse and nursing director.
The post Georgia hospital names Atrium Health Navicent Baldwin COO as CEO appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
The current state of the physician workforce: 9 notes
Physician burnout is declining, systems are finding new ways to recruit physicians without raising pay, but international physicians are in limbo amid visa renewal delays. There are just a few things to know about the physician workforce in 2026.
Here is where the workforce stands in the first half of the year:
1. Across all physician specialties in the U.S., there is a projected shortage of 141,160 full-time equivalent physicians in 2038, according to a December report from the Health Resources and Services Administration.
2. About 59% of healthcare executives said physician specialists are the most difficult clinical job to fill.
3. Pay and financial incentives used to have the greatest impact on physician recruitment, but in recent years, pay has become a smaller factor in why a physician chooses their employer. Physician executives told Becker’s some of the best tools to recruit physicians include a strong culture, opportunities to practice to the top of their license, providing a personal touch during the recruitment process and providing a clinical environment where they can practice what they’ve trained to do.
4. Visa processing delays are sidelining foreign physicians at hospitals and clinics across the nation, adding to staffing shortages and recruitment headaches for hospitals. In October, U.S. Citizenship and Immigration Services froze automatic extensions of employment authorizations for visas. In December, the Trump administration released Proclamation 10998, which implemented a full suspension of entry to the U.S. for nationals from 19 countries, and a partial suspension of entry from 20 countries. Although the travel ban does not apply to visa holders in the U.S., the agency paused visa renewals and updates for people from those countries.
This subjected more than 10,000 physician H-1B visa holders and 17,000 with J-1s, along with thousands of nurses, lab techs and other healthcare workers to the visa pause. Some foreign physicians have waited months for an update on their application, even after their hospital paid a $2,965 fee to fast-track their applications so they would receive it in two weeks. Because most medical residencies begin or end in the summer, a wave of physician visas are expected to expire within weeks, forcing foreign physicians to miss fellowship deadlines, forgo jobs or be sidelined from their current position while waiting for renewal. Physicians on H-1Bs, a visa for highly skilled workers, can keep treating patients for 240 days after their visa expires, but that date is passing for many.
5. Among U.S. resident physicians, about 8 in 10 are in specialty programs and the remainder are in subspecialty programs. Primary care specialties made up the top specialties; internal medicine alone accounted for about one-fifth of all residents. Only 56.4% of non-U.S. international medical graduates matched to a post-graduate year 1, or PGY-1, position, representing a 1.6% decrease from 2025 and a five-year low for these applicants, according to the National Resident Matching Program.
6. An April 23 report from Trilliant Health found that despite a yearslong growth in medical school enrollments and primary care residency slots, these residencies are increasingly going unfilled. Since 2012, U.S. medical residency positions increased 65.6%. For the 2026 Match, more than 40,000 medical school graduates secured a residency spot for 2026. While primary care specialties accounted for about half of these placements (approximately 20,700), “primary care residencies were disproportionately unfilled in 2026,” Trilliant found. “Family medicine went 16.4% unfilled, followed by pediatrics and internal medicine, 5.6% and 4.6%, respectively.”
7. Only 47% of physicians said they would still choose medicine again under the new federal loan cap policy, 27% said they would not choose medicine again and 26% were unsure, according to new data from Panacea Financial shared with Becker’s. Among those paying down debt, 88% identified student loans as the primary burden.
8. Burnout among physicians is continuing to decline, but three specialties — emergency medicine, urological surgery and hematology/oncology — still have a burnout rate of more than 49%, an American Medical Association survey found. In 2025, 41.9% of physicians reported at least one symptom of burnout, down from 43.2% in 2024.
9. Radiology and orthopedics tied for the specialties that lead to the highest net worth, with 39% of providers in those specialties having a net worth over $5 million, an April 24 Medscape report found.
The post The current state of the physician workforce: 9 notes appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
The 10 highest-paying physician specialties in the last 5 years
Orthopedics and plastic surgery have traded the top two spots in Medscape’s annual Physician Compensation Report every year since 2021, and both specialties have seen compensation climb by more than $80,000 over that span.
Orthopedic surgeons now command an average of $611,000 annually, up 20% from five years ago, while plastic surgeons earn $554,000.
- Orthopedics and orthopedic surgery: $611,000
- Cardiology: $575,000
- Radiology: $571,000
- Plastic surgery: $554,000
- Anesthesiology: $543,000
- Urology: $535,000
- Gastroenterology: $530,000
- Otolaryngology: $508,000
- Oncology and hematology: $464,000
- Dermatology: $448,000
- Orthopedic and orthopedic surgery: $543,000
- Radiology: $520,000
- Plastic surgery: $516,000
- Cardiology: $506,000
- Anesthesiology: $499,000
- Gastroenterology: $495,000
- Urology: $485,000
- Otolaryngology: $473,000
- Oncology and hematology: $452,000
- Dermatology: $424,000
- Orthopedics (includes orthopedics and orthopedic surgery): $558,000
- Plastic surgery: $536,000
- Cardiology: $525,000
- Urology: $515,000
- Gastroenterology: $512,000
- Radiology: $498,000
- Dermatology: $479,000
- Anesthesiology: $472,000
- Oncology (includes hematology and oncology): $464,000
- Plastic surgery: $576,000
- Orthopedics: $557,000
- Cardiology: $490,000
- Otolaryngology: $469,000
- Urology: $461,000
- Gastroenterology: $453,000
- Dermatology: $438,000
- Radiology: $437,000
- Ophthalmology: $417,000
- Plastic surgery: $526,000
- Orthopedics and orthopedic surgery: $511,000
- Cardiology: $459,000
- Urology: $427,000
- Otolaryngology: $417,000
- Radiology: $413,000
- Gastroenterology: $406,000
- Oncology: $403,000
- Dermatology: $394,000
- Ophthalmology: $379,000
The post The 10 highest-paying physician specialties in the last 5 years appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
How Emory is using da Vinci digital surgery tools to train the next generation: 3 takeaways
As da Vinci surgery platforms evolve into data-rich, digital ecosystems, health systems are discovering that the real value isn’t just in the operating room — it’s in what the technology can teach.
During a featured session at Becker’s 16th Annual Meeting, Ankit Patel, MD, professor of surgery at Emory University School of Medicine and chief of surgery at Emory Saint Joseph’s Hospital (Atlanta), where he also leads robotic surgical education, shared how the organization has moved from simply performing da Vinci surgery cases to building a comprehensive digital surgical program.
Note: Quotes have been lightly edited for length and clarity.
1. Upgrading the fleet exposed hidden costs and unexpected savings
Emory was among the last academic centers in the country to upgrade its da Vinci surgery fleet, acquiring its first da Vinci Xi in 2019 — five years after launch. Dr. Patel said the delay cost the health system competitive standing and hurt recruitment at every level.
When da Vinci 5 arrived, piloting a single unit revealed something the system hadn’t anticipated: da Vinci surgery cases required fewer instruments, less redundant equipment and simpler sterile processing than laparoscopic alternatives. Costs that had never been carefully tracked suddenly became visible.
“When something breaks, a purchase order gets cut and that equipment gets replaced without really looking into it,” Dr. Patel said. The shift also reduced the need for surgical first assistants in certain cases, freeing staff to be deployed elsewhere — a downstream efficiency the team hadn’t planned for but is now actively tracking for broader standardization.
2. Digital tools are transforming how surgeons are trained and evaluated
Dr. Patel noted that for decades, surgical credentialing relied on case volume with no objective measure of skill. Da Vinci 5’s integrated simulator changes that, offering a structured pathway from basic safety tasks to procedure-specific proficiency. Emory’s fleet has logged more than 200,000 simulator hours, and future versions will analyze prior case performance to recommend targeted exercises automatically.
Equally significant is instant video replay. Where laparoscopic footage once took days to process, da Vinci surgery case video is now accessible within minutes of closing. Residents receive same-day feedback and can apply corrections to their next case immediately, a shift that Emory’s preliminary data suggests is compressing learning curves and accelerating skill transfer across procedure types.
Desktop analytics allow faculty to compare a trainee’s instrument positioning and efficiency across multiple cases in real time, replacing the guesswork that characterized training for generations. “We couldn’t do this before,” Dr. Patel said. “This has been on our wish list for 20 to 30 years.”
3. Telepresence is beginning to reshape how expertise moves across a health system
Emory operates 11 hospitals, and da Vinci 5’s telepresence capability is designed to extend senior surgical expertise to satellite facilities without moving the surgeon or the patient. Dr. Patel currently uses it to observe cases remotely from his clinic, logging in via a text prompt in under 20 seconds. The longer-term vision is enabling satellite-site surgeons to handle higher-complexity cases with remote senior support: reducing interfacility transfers, freeing capacity at the main hub and expanding access to da Vinci surgery across the system.
Physician compensation for remote consultation remains an open regulatory question, but Dr. Patel said Emory is actively working through how to structure the capability across its system. For same-specialty consultations, billing requirements are less of a barrier, making that a natural starting point. “There’s a lot of interfacility transfers we can decrease — that ultimately ends up in savings,” he said.
The post How Emory is using da Vinci digital surgery tools to train the next generation: 3 takeaways appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
12 hospital executives’ thank-you notes to nurses
In honor of National Nurses Month in May and National Nurses Week (May 6-12), hospitals and health systems are recognizing nurses across the country.
This year, the American Nurses Association is again highlighting “The Power of Nurses” as its National Nurses Week theme.
Here are some stats to know about nurses in 2026:
1. For the 24th consecutive year, nurses have ranked as healthcare’s most trusted profession.
2. A March 26 American Nurses Enterprise-commissioned survey found that adjusting minimum wages for competitive compensation, as well as investments in safety, well-being, recruitment and retention, had a strong positive association with a hospital’s operating margin.
3. A Feb. 9 Philadelphia-based University of Pennsylvania survey found the majority of nurses who left bedside roles in recent years are willing to return, and adequate staffing levels are the factor that would reattract them.
4. Across the country, universities and health systems are opening and expanding nursing programs to meet student demand. However, the American Association of Colleges of Nursing found more than 65,000 qualified applicants were turned away in the most recent academic year — largely due to a shortage of nursing faculty.
Becker’s collected messages of appreciation from hospital and health system leaders across the U.S.
Note: Responses have been lightly edited for length and clarity.
Ashley Carlucci, DNP, RN. Chief Nursing Executive for Allegheny Health Network (Pittsburgh): As we celebrate Nurses Week, I want to pause and thank nurses for the leadership, compassion and expertise they bring to patients, families and communities every single day. Nursing sits at the center of care delivery, anchored in human caring, clinical excellence and a deep responsibility to those we serve.
Across every setting, nurses lead with courage and heart, often in moments that matter most. Your voice, judgment and presence continue to shape outcomes, elevate the care experience and advance the profession. Thank you for what you do, for who you are, and for the difference you make, today and always.
Melinda Cooling, DNP. Chief Nurse and Advanced Practice Provider Executive for OSF HealthCare (Peoria, Ill.): I am honored to share my appreciation for our OSF nurses during National Nurses Week. Each day, our nurses make a profound difference in the lives of patients, families and the communities we serve. Nursing is so much more than a profession, it is truly a calling. Our OSF Sisters remind us that everyone is here for a reason and with intention, and that purpose is deeply rooted in compassion, clinical expertise, advocacy and a commitment to providing safe care.
Whether at the bedside, in a clinic, at home or in the boardroom, the presence of our nurses shapes experiences and safety in ways that no metric can fully capture. Patients may not always remember the details of their care, but they always remember how they were treated, with kindness, empathy and respect. This lasting impact often comes from a reassuring word, attentive listening, strong advocacy, or the humility of the care team, and it is the very heart of nursing that extends far beyond clinical moments.
During Nurses Week, I want to express my deep gratitude for your expertise, courage and dedication. You are leaders every day, advancing our mission to deliver safe, compassionate care to every patient, every time. Thank you for being an OSF nurse and for everything you do!
Meredith Foxx, MSN, APRN. Senior Vice President and Chief Nursing Officer of Cleveland Clinic: In honor of National Nurses Week, I want to extend my heartfelt gratitude to nurses across the country, and especially to our nurses at Cleveland Clinic, for the care, compassion and dedication you bring to your work every day. At Cleveland Clinic, nurses are the steady presence at the heart of care, bringing skill, empathy and humanity to every patient and every family in every moment that matters.
I have the privilege of seeing your impact firsthand. You listen closely, anticipate needs and advocate to ensure every patient feels safe, informed and respected. Over the past year, Cleveland Clinic nurses have led meaningful improvements in patient safety, strengthened communication across teams and translated evidence into practice in even the most complex situations. Just as important is the way you show up for one another.
You mentor colleagues, share knowledge and build strong, supportive teams grounded in professionalism and trust. Nursing is more than a profession. It is a calling rooted in service and compassion. Thank you for the countless ways you make a difference each day, including the moments that often go unseen. It is truly an honor to work alongside Cleveland Clinic nurses and to witness the difference you make for our patients, families and communities.
Peggy Norton-Rosko, DNP, RN. Senior Vice President and Chief Nursing Officer at Trinity Health (Livonia, Mich.): Across every role and care setting, our nurses make an immense impact every day through their knowledge, compassion and steady presence. They blend clinical expertise and human connection, caring for patients and families while also supporting and learning from one another. Our nurses are critical to driving meaningful progress and ensuring we continue to meet the changing needs of our communities.
To our Trinity Health nurses, thank you for the dedication and pride you bring to your work every day. The care you provide reflects not only clinical excellence, but the heart of who we are as an organization. Your impact extends far beyond the walls of our facilities, and it is an honor to serve alongside you. During this Nurses Month, and all year long, I share my heartfelt gratitude for all the ways our nurses bring healing and hope to those we serve.
Heather Resseger, DNP, RN. Senior Vice President and Chief Nursing Officer at NorthBay Health (Fairfield Calif.): To our NorthBay Health nursing team: Thank you for the extraordinary care you provide each and every day. The Power of Nurses is evident in every patient interaction, every moment of compassion and every life you touch. Your unwavering commitment not only shapes the patient experience but drives the clinical excellence that defines who we are as an organization. I am incredibly proud that we represent the very best of nursing through measurable patient outcomes and our achievement of Magnet with Distinction recognition — a testament to the strength, skill and dedication you bring to your practice.
I am deeply grateful for your resilience and commitment as we continue to grow and evolve to meet the needs of those we serve. As we expand access to care across Northern California, you remain at the center of improving outcomes and advancing the health of our communities. It is truly an honor to celebrate you and to witness the profound impact you make every day through the power of nursing excellence.
Betty Jo Rocchio, DNP, RN. Executive Vice President and Chief Nurse Executive at Advocate Health (Charlotte, N.C.): I still remember early in my nursing career caring for a patient facing a difficult cancer diagnosis. They were overwhelmed — trying to absorb new information, new fears and a future that suddenly felt uncertain. I couldn’t cure them, but I could care for them. I could sit at eye level, explain what was happening in plain language, hold a hand a little longer, and make sure their voice didn’t get lost in the rush of the day. When they thanked me for what I thought were “small” things, it reminded me that nursing is, at its heart, a promise: to show up with skill, courage and humanity when someone needs it most.
That promise is alive in you. To nurses everywhere — in hospitals and clinics, operating rooms, schools and homes — you step into life’s most vulnerable moments and bring expertise, calm and connection. You combine skill and calm to help patients feel safe in unfamiliar moments. You assess, prioritize and intervene with expertise that changes the course of care. You notice the small signs that make a big difference. You advocate, you teach, you lead and you keep going — always with purpose. During Nurses Week, I want to say what our patients feel every day: thank you. Thank you for choosing this profession, for the compassion you give so freely and for the strength you lend to every person and community you serve.
Brenda Rocha, DNP, RN. Chief Nursing Officer at Baystate Medical Center, Baystate Health (Springfield, Mass.): To my highly esteemed nurses, I salute and honor you with deep appreciation for your commitment to such an extraordinary profession. Nursing remains one of the most respected and trusted calling in the world, and each of you exemplifies why. Thank you for your smiles that bring comfort, your empowered voices that advocate fiercely, your courageous spirit in the face of challenge and your endless passion. The impact you make is felt in every moment of care, whether through a simple touch or an unspoken word.
Your resilience is nothing short of inspiring, and your spirit of inquiry continues to push the boundaries of what is possible, improving outcomes and transforming lives. I am deeply honored to lead you, to learn from you, and to walk beside you in this meaningful work. You are the heart of healing, the voice of hope and the embodiment of excellence in action. Thank you, for all that you are and all that you give. Happy Nurses Week.
Robert Rose, DNP, RN. Senior Vice President of Nursing and Chief Nursing Officer at Ascension (St. Louis): Our Ascension Mission is not just a statement; it is a tangible reality made possible by your commitment to be present for others and to ensure the most vulnerable receive the care they need. During National Nurses Week, we celebrate the incredible strength and dedication of our Ascension nurses. The American Nurses Association’s theme, “The Power of Nursing,” deeply represents us, as it is lived out every day through the extraordinary care you deliver to our families, patients, and the communities we serve. Your dedication and commitment make our Ascension Mission a living reality, ensuring the most vulnerable receive the care they need.
We recognize that nursing is a meaningful vocation — centered on serving humanity and ministering to people during some of the most difficult times of their lives. Whether you are impacting a patient’s care, promoting healing or working tirelessly to remove barriers so families can be reunited, your impact is immeasurable. Thank you for everything you do to care for our patients and families, and for being the hands and heart of Ascension. I am proud to practice alongside you!
Kathleen Sanford, RN. Senior Executive Vice President and Chief Nursing Officer of CommonSpirit Health (Chicago): As we celebrate National Nurses Week, I reflect on the work we did five years ago to develop the first strategic plan for nursing at CommonSpirit Health. At that time, we created five different pins to celebrate nursing, each engraved with words describing what it means to be a nurse at CommonSpirit. The words we chose to honor the skills and vision that nurses bring to care for patients and communities are applicable across our profession:
- Head, heart and hands: You use your head, your heart and your hands to provide care for patients.
- Intellect with love: This is a reminder that we are bright, science-focused professionals who always practice with love.
- Compassion and skill: No matter how skilled you are, in healthcare you must also have compassion, and that describes nurses perfectly.
- Art and science: As we know, nursing is both an art and a science.
- Collegiality and leadership: Collegiality defines the teamwork and spirit of our profession, while leadership reflects the vital role that nurses play in shaping patient care and driving healthcare innovation forward.
To all nurses: Thank you for choosing this profession and for using your talents to make a difference. Most of all, thank you for being united in the purpose and passion of caring for patients.
Janet Tomcavage, MSN, RN. Executive Vice President and Chief Nursing Executive for Geisinger (Danville, Pa.): Nurses are the steady heart of healthcare — showing up every day with skill, compassion and resilience. You care for patients at their most vulnerable moments, listening closely, advocating fiercely, and delivering expert care with humanity and dignity. Your ability to combine clinical excellence with genuine empathy makes a lasting difference not only in outcomes, but in how patients and families experience care.
Thank you for the extraordinary work you do, often under intense situations with higher acuity needs. Your dedication, teamwork and courage lift entire communities and inspire everyone around you. Healthcare is stronger because of you, and your impact reaches far beyond the bedside into our ambulatory and home settings. We are deeply grateful for all that you do — today and every day.
Syl Trepanier, DNP, RN. Chief Nurse Executive at Providence (Renton, Wash.): It is with immense gratitude and pride that I thank each and every nurse across the Providence family of organizations. Thank you for your dedication to our patients, to the nursing profession, to our communities and to each other. I know what you do is not easy. The long hours, the difficult decisions, the sometimes-heartbreaking moments. You are appreciated, you are loved and valued. Happy Nurses Week.
Anne Marie Watkins, DNP, RN. Chief Nursing Executive and Senior Vice President at UCI Health (Irvine, Calif.): During Nurses Week, we celebrate the compassion, expertise, courage and leadership that nurses bring to every patient interaction and every corner of healthcare. Across UCI Health, I am deeply grateful for our nurses who heal, advocate, innovate and lead with both skill and heart. Whether at the bedside, in our clinics, classrooms, research settings or leadership roles, your impact is profound and far-reaching. Thank you for the extraordinary difference you make for our patients, families and communities each day.
The post 12 hospital executives’ thank-you notes to nurses appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
5 ways insurers are betting big on AI
AI was front and center during recent earnings calls for UnitedHealth Group and Elevance Health, as leaders discussed their companies’ respective $1.5 billion and $1 billion tech investments. Both organizations, along with Centene, made Fortune‘s top companies for AI adoption in 2025, as well.
Payers have been experimenting with internal and member-facing capabilities, while grappling with health system AI use, as well. As insurers build upon their substantial investments and weigh how humans can stay “in the loop,” here is where that money is actually going.
Member navigation and digital experience
From chatbots to provider-matching tools, major insurers have been diving into use cases that aim to drive member experience.
Several major insurers — including UnitedHealthcare, Elevance, Aetna and Cigna — have launched virtual assistants for members. By the end of 2026, more than 20 million UnitedHealthcare members should have access to generative AI virtual assistant Avery. Elevance’s virtual assistant reached 22 million commercial members, and the company planned to broaden the assistant’s reach to Medicare. Aetna said it would roll out voice enablement with its generative AI assistant in early 2026.
Along with an AI-powered chatbot, Cigna also launched a “proprietary” provider-matching tool and redesigned its real-time cost-tracking resource, which breaks down deductibles, out-of-pocket costs and integrated bill payments. A claim submission feature allows members to upload bills, autofills details and fields updates. Those with employer-sponsored coverage can also access plan selection support to get a sense of healthcare costs and available providers.
Prior authorization and claims processing
As carriers double down on their commitment to reducing prior authorization, AI has become one means of doing so. The vast majority of surveyed health plan executives, 93%, expect AI to add value by automating prior authorizations, according to recent Deloitte research.
During Elevance’s latest earnings call, President and CEO Gail Boudreaux said the company’s Health OS platform and other AI tools have cut prior authorizations by almost 70%. Under Carelon, Health OS unifies provider data, lab results and pharmacy information, filling gaps that could otherwise prompt a denial. More than 60,000 Elevance associates can access this technology.
Internal automation
Across insurers of all sizes, internal automation has been a priority with AI deployment. Last year, former UnitedHealth Group CEO Andrew Witty said the company directed 26 million customer calls with AI agents and anticipated that AI would direct more than half of these calls by 2026.
Earlier this year, Humana deepened its relationship with Google Cloud to launch its AI-enabled Agent Assist, which aims to accelerate care-support personnel activities.
Beyond direct member interactions, Elevance employees use AI toolkit Spark to streamline workflows. The features help with manual task automation, including document analysis and contract processing.
Clinical decisionmaking and solutions
Recently, Optum’s Value Connect brought together clinical, operational and financial data into a single system for payers and providers in value-based arrangements. The platform can flag which members may need intervention. This year, Optum reported customers had 29% fewer emergency room visits, 28% fewer preventable hospital readmissions and more than a 20% improvement in care gap closure. Elevance’s Health OS also strives to bridge interoperability gaps.
Industry group AHIP recently shared how payers are putting AI to use in predictive risk modeling and research support to assist with care management.
The post 5 ways insurers are betting big on AI appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
64% of Americans worry about healthcare costs: 6 notes
With 2026 midterm elections around the corner, nearly two-thirds of U.S. adults are concerned about affording healthcare, according to an April 29 KFF poll.
The survey canvassed 1,343 U.S. adults, of whom 1,107 were registered to vote.
Here are six notes from the poll:
1. The share of adults concerned about healthcare affordability parallels the amount of U.S. adults worried about gas and transportation costs, which is also 64%.
2. When asked about steps health insurers could take, nearly one-half of adults said lowering out-of-pocket costs would be their top priority. Twenty-two percent said eliminating prior authorization, and 12% said more flexibility with choosing providers.
3. Roughly 9 out of 10 voters said healthcare costs will influence their approach to 2026 midterms. The majority of Democrats and independents said these costs will inform which party’s candidate they support.
4. Thirty-seven percent of voters trust the Democratic party on healthcare costs, whereas only 26% believe in the Republican party’s ability to address the issue. Less than half of voters support the Trump administration’s approaches to healthcare and prescription drug costs.
5. However, Republicans are more trusted than Democrats when it comes to addressing fraud and waste in government health programs.
6. Many voters do not trust either party on most healthcare-related issues, though.
The post 64% of Americans worry about healthcare costs: 6 notes appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Rural Health Transformation Should Mean Removing Barriers—Not Reinforcing Them
Rural healthcare is at an inflection point. Hospitals are closing or scaling back essential services. Labor and delivery units are disappearing. Rural operating rooms sit idle not due to a lack of patients, but to a shortage of clinicians. At the same time, policymakers are advancing initiatives like the President’s Rural Health Transformation Program (RHTP), aimed at rethinking how care is delivered in rural communities.
This is a moment for bold thinking. But transformation cannot succeed if outdated regulatory barriers remain. While the RHTP has made progress by easing restrictions on nurse practitioners and physician assistants, significant barriers persist for specialized providers like nurse anesthetists.
If we are serious about strengthening rural healthcare, policy should be assessed through a simple framework: Effectiveness, Efficiency, and Enhanced Access.
Effectiveness: Proven Care, Proven Outcomes
Certified Registered Nurse Anesthetists (CRNAs) have safely delivered anesthesia care for more than a century. In many rural hospitals, they are the primary and many times, the only anesthesia professionals.
The evidence is clear: anesthesia care delivered by CRNAs is safe, high-quality, and comparable to other delivery models. This is not a new workforce. CRNAs are a mature, well-established profession with a long track record of safety across all practice settings, including the most resource-constrained environments.
When access to anesthesia determines whether a hospital can sustain surgical, obstetric, or emergency services, effective policy must ensure that care can actually be delivered.
Efficiency: Lower Costs, Sustainable Systems
Rural hospitals face extraordinary financial pressure. Thin margins, workforce shortages, and declining reimbursement make every operational decision high-stakes.
CRNAs are the most cost-efficient solution to sustain anesthesia services. Allowing them to practice to the full extent of their licensure enables high-quality care while better managing labor costs – often the single largest expense hospitals face.
By contrast, unnecessary supervision adds cost and administrative complexity without improving outcomes. These requirements can delay care, limit staffing flexibility, and even force service line closures. Medicare’s physician supervision requirement, which persists despite opt-out policies in half of states and no supervision requirement in the laws of 45 states, often results in non-anesthesia-trained physicians “supervising” highly-trained anesthesia professionals. Hospitals are then left with two poor options: reduced access to anesthesia services or adoption of significantly more expensive care models that further strain fragile finances.
If rural health transformation is meant to create reliable systems of care, removing artificial barriers should be a shared priority.
Enhanced Access: Providing Care Where It’s Needed Most
Access to healthcare is often discussed in abstract. In rural communities, it is more straightforward: access is everything.
When an expecting mother must travel hours for a C-section, a farmer delays surgery, or a child’s emergency care is limited by anesthesia availability, the system is not delivering.
CRNAs are uniquely positioned to address this: they are more likely to practice in rural and underserved areas and already serve as the backbone of anesthesia delivery in many of these communities.
Policies that restrict their ability to practice fully directly reduce access; policies that empower them expand access immediately.
Looking Ahead: A Workforce Reality We Can’t Ignore
The nation faces a growing shortage of physician anesthesiologists. Training pipelines have not kept pace, and geographic maldistribution continues to widen gaps, especially in rural areas with aging populations.
In contrast, the number of CRNAs is growing steadily, with strong representation in rural America and a demonstrated willingness to serve where need is greatest.
This is not a future concern, it is a present reality. Policymakers can either align regulations with workforce trends, now or confront worsening consequences later. Delays carry real risk, as rural hospital closures are often permanent.
Addressing the Safety Argument
Opposition to full scope of practice for CRNAs is often framed around patient safety. That argument does not withstand scrutiny. More than a century of clinical practice, supported by decades of research, shows no credible evidence of compromised safety. These arguments persist not because of data, but because of longstanding professional and economic interests.
Healthcare policy should be guided by evidence and patient needs, not protectionism.
A Clear Opportunity
The RHTP represents an opportunity to modernize care delivery in underserved communities. Meaningful transformation should:
- Remove unnecessary barriers limiting CRNA practice
- Align scope-of-practice policy with licensure and outcomes
- Prioritize workforce models that improve access and reduce costs
- Support rural hospitals with flexible, evidence-based staffing solutions
This is not about choosing one provider over another. It is about ensuring access to safe, timely, and affordable care, regardless of geography.
Conclusion
Rural healthcare does not need more complexity. It needs practical solutions grounded in reality.
Applying the framework of effectiveness, efficiency, and enhanced access leads to a clear conclusion: allowing CRNAs to practice to the full extent of their licensure is one of the most immediate, impactful steps available to stabilize rural healthcare.
The tools already exist. The question is whether we are willing to use them.
Tracy Young, MS, MBA, CRNA, is a healthcare executive and Certified Registered Nurse Anesthetist who leads large‑scale anesthesia operations as Chief Operating Officer of Essential Anesthesia Services. He currently serves as President‑Elect of the American Association of Nurse Anesthesiology.
The post Rural Health Transformation Should Mean Removing Barriers—Not Reinforcing Them appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Medical liability premiums rise for 7th year: 6 things to know
Medical liability insurance premiums increased nationwide for the seventh consecutive year in 2025, marking the longest sustained upward trend since the early 2000s, according to new research from the American Medical Association.
AMA published two policy research reports on medical liability April 27. The first analyzes annual changes in medical liability insurance premiums between 2016 and 2025. The second examines medical liability claim frequency among patient care physicians in the U.S. between 2016 and 2024.
“Although there was a continued rise in MPL premiums over the past seven years, the severity and the magnitude of this rise pale in comparison to the hard market in the early 2000s,” Allen Hardiman, PhD, AMA’s lead economist, wrote in the first report. “Nevertheless, if this upward trajectory continues to worsen in the future, it could lead to a negative impact on patients’ access to care.”
A hard market refers to a period marked by significant premium increases, stricter underwriting and reduced coverage availability.
Six things to know:
1. The share of medical liability premiums that increased year-over-year jumped from 13.7% in 2018 to 39.9% in 2025.
2. Last year, physicians in 36 states reported at least one premium increase. Physicians in 11 states had at least one premium increase by 10% or more.
3. Pennsylvania, Kentucky, Florida, Illinois and New York saw the largest increases between 2024 and 2025. California remained an outlier with significantly lower premiums, as the state has a cap on non-economic damages.
4. Premiums were highest for OB/GYN and general surgery, reflecting greater liability exposure in those specialties.
5. Overall, 28.7% of physicians reported being sued during their careers in 2024, down from 34% in 2016.
6. Physicians 55 and older were more likely to be sued (45.2%) compared to those under 45 (11%). Among OB/GYNs and general surgeons 55 and older, nearly three in four had faced at least one claim in their careers.
The post Medical liability premiums rise for 7th year: 6 things to know appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 states with most, least drug use
New Mexico is the most at-risk state for drug use, according to an April 29 ranking from personal finance website WalletHub.
The list was created to determine where drug use is most pronounced and which areas are most at risk by comparing the 50 states and Washington, D.C. across 20 metrics in three categories: drug use and addiction, law enforcement and drug health issues and rehabilitation.
Metrics included overdose deaths per capita and substance abuse treatment facilities per 100,000 people using illicit drugs. WalletHub calculated each state’s weighted average across all metrics to determine its overall score, with the state ranked No. 1 having the most significant drug problem based on the data analyzed.
The U.S. saw the largest decrease in drug overdose death rates ever recorded in 2024, exceeding the record set in 2018. The rate declined 26.2% between 2023 and 2023, from 31.3 to 23.1 per 100,000, according to CDC data. A separate CDC report found Vermont, Rhode Island and New York had the largest decreases in predicted drug overdose deaths between August 2024 and August 2025.
Here are the 10 states most and least at risk for drug use, per WalletHub:
10 most
1. New Mexico
2. Arkansas
3. Alaska
4. Nevada
5. Missouri
6. West Virginia
7. Colorado
8. Washington, D.C.
9. Oklahoma
10. Mississippi
10 least
42. Nebraska
43. Connecticut
44. Hawaii
45. Ohio
46. Virginia
47. Iowa
48. Maryland
49. Minnesota
50. Florida
51. Utah
The post 10 states with most, least drug use appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Can ambient AI work for nurses? Jefferson Health is finding out
As part of a goal to return 10 million clinical hours to clinicians by 2028, Philadelphia-based Jefferson Health is piloting an ambient AI documentation tool for nursing units — a largely unprecedented goal for health system AI projects.
The system operates 32 hospital campuses and approximately 700 care sites throughout Pennsylvania and New Jersey. In September, the organization announced the time-saving plan, which also broadly aims to improve patient care and outcomes, cut administrative burden and enhance operational efficiency.
Jefferson Health President Baligh Yehia, MD, told Becker’s the system wants to save each clinician an average of one hour of administrative work per day, which adds up to 10 million hours that can be used for patient-facing care. The saved time is measured through signal data, which are the AI tool logs, as well as in-person observation to verify the data.
An early aspect of this project featured ambient listening technology available to Jefferson’s physicians, advanced practice providers and physical therapists working in specific settings, including ambulatory sites.
So far, the system has logged about 350,000 hours, or 3.5%, thanks to the ambient technology, according to Colleen Mallozzi, RN, senior vice president and chief nursing informatics officer at Jefferson Health.
Ms. Mallozzi and Dr. Yehia told Becker’s they expect other AI-focused technologies, including a documentation tool that could be made available to its 14,000 nurses and other staff, will expedite the system’s progress toward 10 million hours.
The ambient AI pilot for nurses
Based on the success of physicians using ambient listening technology for documentation, Jefferson is taking a similar — but not identical — approach for nurses.
Physicians document their work through treatment decisions and care plans in EHRs; while nurses document in standardized flow sheets with drop-down menus and checklists. That fundamental difference influenced how Jefferson is testing ambient AI for nursing.
At three nursing units at Abington (Pa.) Hospital, a 667-bed regional referral and teaching hospital, care teams are piloting ambient AI technology. The tool translates spoken language into structured flow sheet documentation.
After gaining a patient’s consent, the nurses, patient care technicians, patient care coordinators and nurse managers on those three units verbalize their assessments. The ambient technology ingests the care conversations and delivers a structured output for nursing flow sheets.
The first hurdle for Jefferson? Nurses do not always verbally communicate what they are doing.
“Imagine if you had to go throughout your day just verbalizing everything you were doing. How awkward would that be?” Ms. Mallozzi said. “Nurses are used to quietly going about their assessments, doing three different tasks at once, and now they have to verbalize it. So this was a big change. There’s an awkwardness to get over, to figure out how to have that conversational care with your patients and verbalize some of the things you were doing.”
‘We have camps’: The adoption challenge
About 30% of nurses are hesitant to use the technology, Ms. Mallozzi said.
Jefferson hosted a panel discussion about the technology April 22 for about 400 nurse leaders to query staff members who are taking part in the pilot. Common concerns raised by staff included legal ramifications, environmental effects, potential over-reliance and feeling like they are “performing” for the AI rather than focusing on the patient.
She said newer-to-practice nurses are more hesitant to verbalize their assessments, likely because they are “still getting their feet grounded in their practice.”
“It’s been a little polarizing. We have camps,” Ms. Mallozzi said, adding that Jefferson plans to make the model opt-in after the pilot, similar to the rollout for the physicians’ ambient documentation tool.
Results so far
The pilot is in its early stages, so nursing-specific outcomes are still emerging. However, Ms. Mallozzi said the ambient tool is changing the way nurses work.
“The technology is amazing, but this is about transforming the way that nurses practice, the way that they engage with their patients: to verbalize their care,” Ms. Mallozzi said. “It’s incredible, because it’s helpful for the patients to understand what you’re going through, what you’re thinking through, that critical thinking aspect.”
She raised an unexpected benefit: the added educational value for nursing students at the teaching hospital. Nursing students do not have to guess at the clinical reasoning behind their supervisors’ decisions — the verbalization requirement makes that thinking explicit and audible in real time.
For documentation, Jefferson Health leaders are predicting similar results from its ambient tool for physicians and APPs. That tool has decreased time spent on EHRs by about 17%, as well as 16% less time spent on charts outside of work — sometimes called “pajama time” — and 40% less time to close a chart, Dr. Yehia said.
On a larger scale, he said Jefferson is saving clinicians an average of 15 to 20 minutes per day.
Jefferson’s broader AI strategy and governance structure
The system has identified and implemented more than 100 AI-powered solutions, including ones focused on care delivery, revenue cycle operations and back-office tasks.
Each idea and technology is funneled through Jefferson Health’s AI Center for Excellence, which launched in 2022. A key component of the system’s AI governance structure is usability.
“The biggest underline for me is this [AI technology] is being implemented by our clinical staff, for them and by them,” Ms. Mallozzi said. “We aren’t just making broad stroke decisions for what they’re going to use. … We run [technology] by them, we let them poke holes in it and then we pilot it with them.”
If an AI tool does not click with clinicians, it does not make it to a systemwide launch, she said.
Jefferson’s near-future AI plans include agentic technologies, such as voice agents for follow-up phone calls and appointment scheduling.
We are not “implementing technology for the sake of implementing technology,” Ms. Mallozzi said. “It truly is grounded in returning time to care: care for yourself, care for your patients. I think it’s really important that we look at, are you getting time to take a breath after a complex patient experience or a death of a patient? Are you getting time to take your lunch? The time may be given back for that bedside care and time with patients, but if our clinicians are caring for themselves, they’re going to be better caregivers for other individuals as well.”
The post Can ambient AI work for nurses? Jefferson Health is finding out appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
What’s retaining nurses in long-term care
The majority of nurses working in long-term care said they are happy in their position, but 73.8% have reported their job has become more difficult in the last 18 months, a recent American Association of Post-Acute Care Nursing survey found.
The survey of nearly 500 nurses and certified nurse aides, conducted in November, asked about their perspective on drivers of job satisfaction and challenges in their jobs, according to an April 27 association news release.
Here are three survey findings:
1. The most important factors keeping nurses in their jobs are meaningful relationships with residents (31%), a strong sense of purpose (28%) and team and work culture (15%).
2. The top contributors to dissatisfaction and burnout are increasing regulatory burden (16%), staffing shortages (12.5%) and leadership gaps (7%).
3. Nurses are more likely to stay in a position that is supported by a strong work culture with a reinforced sense of purpose and flexibility. A nurse’s decision to stay or leave is also closely tied to their relationship with their supervisor.
The post What’s retaining nurses in long-term care appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
6 best healthcare employers for career growth: LinkedIn
Six healthcare organizations — including one health system — have been recognized on LinkedIn’s list of the 50 best U.S. employers to grow careers.
The LinkedIn Top Companies 2026 list features organizations that provide employees with skill-building and advancement opportunities, according to an April 28 LinkedIn News post. It is based on LinkedIn data and evaluates companies on key markers of career progression, such as how employees develop new skills and how quickly they advance within an organization.
Eligible companies had 5,000 or more global employees, with at least 500 in the U.S., as of Dec. 31. Attrition could be no higher than 10%, and companies could not have layoffs of 10% or more over the methodology period of Jan. 1, 2025, through Dec. 31.
Here are the healthcare organizations featured, along with their rank out of 50 and headquarters city:
11. CVS Health (Woonsocket, R.I.)
13. UnitedHealth Group (Eden Prairie, Minn.)
24. Eli Lilly and Co. (Indianapolis)
28. Kaiser Permanente (Oakland, Calif.)
30. Roche (San Francisco)
41. Abbott (Abbott Park, Ill.)
The post 6 best healthcare employers for career growth: LinkedIn appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
The federal policy pushing physicians out of medicine
Physicians are increasingly uncertain if their career choice was worth the debt they took on for training — and some of them would not choose medicine again under new federal caps on student loans, according to new data from Panacea Financial shared with Becker’s.
The survey included responses from 270 physicians and was conducted in early 2026.
Here are six takeaways from the survey:
1. Only 47% of physicians said they would still choose medicine again under the new federal loan cap policy. Another 27% said they would not choose medicine again, while 26% were unsure.
2. Paying of debt was the single most common financial priority named by respondents, cited by 79% as their top goal.
3. Debt repayment ranked above retirement savings, homebuying and investing as priorities. Among those paying down debt, 88% identified student loans as the primary burden.
4. Of physicians who said they struggle to balance loan repayment with other financial goals, 37% were already in practice, a sign that higher attending salaries do not automatically resolve debt-driven financial stress.
5. Financial confidence among physicians also remains low. On a five-point scale, 71$ of respondents rated their financial confidence as a 3 or below. physicians actively in practice averaged just 3.27 out of 5, and medical students averaged 2.33, with residents and fellows averaging 2.63.
6. Forty-six percent of respondents said they do not fully understand their loan repayment, forgiveness or refinancing options.
The post The federal policy pushing physicians out of medicine appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 predictions for hospital margins: Moody’s
Hospitals are bracing for a cascade of financial pressures as rising insurance costs, Medicaid restrictions and a growing number of uninsured patients threaten to reshape patient behavior and erode margins in the years ahead, according to a new Moody’s Healthcare Quarterly report.
From declining elective procedure volumes to worsening payer mix and ballooning bad debt, health system leaders face a challenging landscape that could last through 2027 and beyond.
Here are 10 predictions for health system executives.
1. The increasing costs of health insurance and out-of-pocket expenses will likely change patient behavior in the coming years. Hospital leaders can expect lower patient volumes, especially for “profitable elective procedures,” according to Moody’s, which will negatively affect financial performance.
2. Many hospital executives will see a worse payer mix as fewer patients use commercial insurance and Medicaid eligibility is restricted. They’ll likely experience lower reimbursement for services and higher uncompensated care with more uninsured patients.
“These effects will likely be gradual and varied, having a greater effect on hospitals located in certain states or with higher exposure to certain demographic groups,” the report notes. “The impact on margins will likely be muted in 2026, with the potential for more margin erosion ahead.”
3. The number of uninsured patients will likely increase due to higher premiums – which are rising 6% to 7% in 2026 for employer-sponsored plans – and subsidy cuts for ACA plans. Unemployment is also on the rise and with it, a drop in employer-sponsored plans.
4. Medicaid restrictions may “significantly decrease the number of people covered,” especially in states with Medicaid expansion. Work requirements expected to take effect next year will further limit access. Hospitals can expect fewer Medicaid-covered patients and more resources spent on administrative work and redetermination, according to the report.
“There is also the potential for revenue losses due to provider payment caps and reductions in the Federal Medical Assistance Percentage (FMAP), the formula used to determine how much of a state’s Medicaid costs are paid by the federal government,” the report notes.
5. Bad debt will likely increase as hospitals see lower patient volumes, more uninsured patients and pass more costs on to patients.
6. Hospitals may report a decline in elective surgery as patients lose health insurance or take on high deductible plans, opting to forgo care until it’s life threatening. Fewer high-dollar elective procedures would negatively affect cash flow, according to the report.
7. Uninsured patients and patients with limited access to healthcare may also decide to forgo preventative care and routine visits, which would lead to higher emergency room traffic. “This will further cut into hospitals’ profit margins,” according to the report.
8. Hospitals may see less reimbursement for services performed after payer mix shifts. “We estimate that a one percentage-point shift in payor mix from commercial to Medicaid is associated with an estimated 0.5%-1.0% decline in net patient service revenue and approximately 50-150 basis points in operating margin compression, before consideration of offsetting cost actions or Medicaid supplemental payments,” the report says.
9. The hospitals with large emergency medicine operations will likely experience more negative impacts from uncompensated care.
10. For-profit hospital operators could see reduced EBITDA due to the ACA’s enhanced premium tax credit expiration. Moody’s estimated for-profit operators could see up to 6.4% reduction in EBITDA year over year, with larger companies most able to make adjustments that would dampen impact.
The post 10 predictions for hospital margins: Moody’s appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Why AI in revenue cycle has become a necessity — 3 takeaways
Revenue cycle leaders are facing a national coder shortage, intensifying payer complexity and tighter margins. In this environment, AI has become an operational necessity, not a strategic option. But the differentiator isn’t tool selection; it’s whether leaders have reframed workforce and governance for a technology that now arrives continuously, not in discrete projects.
During an April 14 featured session hosted by Soventum at Becker’s Hospital Review 16th Annual Meeting, three leaders working across academic medical centers, health systems and vendor partnerships discussed how they are pairing AI with upskilling and governance to protect both ROI and teams. The panelists were:
- Michelle McCormack, director of clinical documentation integrity at a large health system in California
- Tami McMasters Gomez, executive director of revenue cycle at UC Davis Health in Sacramento, Calif.
- Thea Campbell, business director of revenue cycle at Solventum and acting president of the American Health Information Management Association
Below are three takeaways from their conversation.
Note: Quotes have been edited for length and clarity.
1. The business case is coder shortage meets payer complexity
Ms. McMasters Gomez traced AI’s shift from innovation to necessity in mid-rev cycle to a national coder shortage producing backlogs in charge lag, AR days and related KPIs — especially at growing systems.
Ms. Campbell said payer complexity is the equal partner: realizing revenue has grown too fragmented and payer-specific for a single standardized workflow, and with organizations fighting for every dollar they collect, AI has become the tool finally equipped to address that complexity at scale.
2. Upskilling, not replacement, is the workforce play
At UC Davis Health, Ms. McMasters Gomez said the team is moving coders from repetitive areas like radiology, where AI is mature, onto more complex work such as dermatology procedure coding — while standing up a formal policy for auditing AI output and routing coders into different roles.
“There’s got to be a human in the loop,” she said.
Ms. McCormack said CDI teams will need a different talent mix once simple audits are automated: strategic thinkers, project managers and staff who can read tool performance and feed learnings back to vendors.
“These tools are only as good as the documentation it sits on,” she said.
Ms. Campbell framed the cultural shift plainly: “AI is not going to take your job. AI is going to change your job.”
3. Governance and pace separate winners from losers
Ms. McMasters Gomez described UC Davis’s IT AI governance and IT security structures, which vet every vendor through what she called a deliberately agonizing process before sign-off.
Ms. Campbell said IT partners at large systems are sometimes managing 150-plus products, meaning revenue cycle has to negotiate for a handful of priority projects rather than assume capacity.
Both Ms. McCormack and Ms. Campbell said AI can no longer be treated as a discrete project — new capabilities arrive continuously, and leaders who chase every vendor will face significant rework as regulation catches up.
Beyond the project mindset
The panel’s common thread: pace, governance and workforce strategy matter more than tool selection. Ms. McCormack urged caution and stacked deployments around a small set of trusted vendors, with clinical, IT and revenue cycle leaders in the room together before adding more. For executives whose AI programs are still being managed pilot by pilot, the implication is a structural rethink of how AI capabilities are absorbed into daily operations.
The post Why AI in revenue cycle has become a necessity — 3 takeaways appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 best, worst states for nurses in 2026
Maine is the best state for nurses to practice in 2026, according to WalletHub’s annual ranking, which evaluates opportunity, competition and working conditions.
To determine the best and worst states for nurses, the personal finance company evaluated all 50 states across two two dimensions: opportunity and competition, and work environment. Those dimensions were evaluated using 20 metrics, ranging from monthly average starting salary for nurses to average commute time.
Analysts graded each metric on a 100-point scale, with a score of 100 representing the most favorable conditions for nurses.
Each state’s weighted average across all metrics was used to calculate its overall score and rank the sample. More information about the methodology is available here.
Here are the 10 best and worst states for nurses in 2026, per the ranking:
Best
1. Maine
2. New Hampshire
3. Washington
4. Oregon
5. Arizona
6. West Virginia
7. Minnesota
8. Montana
9. Connecticut
10. Florida
Worst
50. Oklahoma
49. North Dakota
48. Alabama
47. Mississippi
46. South Dakota
45. Louisiana
44. Tennessee
43. Arkansas
42. Hawaii
41. Virginia
Three notes:
- Though ranked No. 1 overall, Maine placed 10th for the opportunity and competition rank, and third for work environment.
- New Hampshire (ranked second overall), earned the top spot for the work environment rank and placed 12th for opportunity and competition.
- Arizona (ranked fifth overall) was ranked No. 1 for opportunity and competition, and 25th for work environment.
The post 10 best, worst states for nurses in 2026 appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 best, worst entry-level jobs in 2026
WalletHub released its 2026 ranking of the best and worst entry-level jobs April 27, and certified nursing assistants in nursing homes claimed the No. 3 spot — driven by a 2.9% unemployment rate, high job availability, and one of the lowest chances of being replaced by automation.
To identify the best and worst first-timer jobs, the personal finance company compared 108 entry-level occupations across three dimensions: immediate opportunity, growth potential and job hazards.
Analysts evaluated the dimensions using 12 metrics ranging from average starting salary to typicality of working more than 40 hours per week.
Each metric was graded on a 100-point scale, with 100 representing the most favorable conditions for entry-level workers. WalletHub used each entry-level position’s weighted average across all metrics to calculate its overall score. More information about the methodology is available here.
The best and worst entry-level jobs, alongside their scores, according to the analysis:
Best
1. Hardware engineer I
2. Engineer I
3. Certified nursing assistant – nursing home
4. Software engineer I
5. Safety representative I
6. Safety technician I
7. Electrical engineer I
8. Operations research analyst I
9. Environmental, health and safety engineer I
10. Electronics engineer I
Worst
108. Welder I
107. Emergency dispatcher
106. Automotive mechanic I
105. Boilermaker I
104. Computer numeric control machine programmer I
103. Mechanical drafter I
102. Telecommunications technician I
101. Benefits administrator I
100. Tool and die maker I
99. Architectural drafter I
The post 10 best, worst entry-level jobs in 2026 appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
The best states for senior living: US News
Florida has the highest number of “best” senior living communities, while three states — Alaska, Montana and North Dakota — have no top-ranked communities, according to an April 14 U.S News & World Report ranking.
In its 5th annual Best Senior Living ratings, U.S. News honored a total of 1,614 communities for providing the best care.
The report analyzed 3,098 senior living communities in independent living, assisted living and/or memory care. The company also took into account community life aspects, such as dining and activities, management and staff responsiveness, overall value and social engagement, and safety and caregiving. Participant communities had to be part of the consumer-satisfaction survey in 2025 and meet other eligibility criteria. Read more about the methodology here.
Here is the total number of top-ranked senior living communities in each state and the District of Columbia.
Alabama: 8
Alaska: 0
Arizona: 32
Arkansas: 6
California: 117
Colorado: 34
Connecticut: 23
Delaware: 2
Florida: 137
Georgia: 35
Hawaii: 1
Idaho: 5
Illinois: 98
Indiana: 37
Iowa: 17
Kansas: 34
Kentucky: 10
Louisiana: 12
Maine: 2
Maryland: 51
Massachusetts: 68
Michigan: 46
Minnesota: 37
Mississippi: 8
Missouri: 73
Montana: 0
Nebraska: 19
Nevada: 7
New Hampshire: 8
New Jersey: 51
New Mexico: 2
New York: 56
North Carolina: 67
North Dakota: 0
Ohio: 47
Oklahoma: 20
Oregon: 14
Pennsylvania: 74
Rhode Island: 11
South Carolina: 24
South Dakota: 1
Tennessee: 58
Texas: 139
Utah: 8
Vermont: 3
Virginia: 60
Washington: 36
Washington, D.C.: 1
West Virginia: 5
Wisconsin: 9
Wyoming: 1
The post The best states for senior living: US News appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
11 things to know about the uninsured population: KFF
In 2024, the uninsured rate grew for the first time since 2019, according to an April 9 KFF issue brief.
KFF reviewed data on uninsured trends and demographics in recent years, focusing on individuals under 65 years old. Following a pandemic-era rollback of redeterminations, people eventually began facing eligibility checks after Medicaid’s continuous enrollment provision ended in 2023. The following year, many states finished this unwinding, resulting in coverage losses. Medicaid and ACA changes, along with enhanced subsidy expiration, could keep up this trend in future years.
Here are 11 notes about the uninsured in 2024:
1. The number of people lacking health insurance and the uninsured rate increased in 2024 for the first time since 2019, reaching 26.7 million people and a rate of 9.8%.
2. The Congressional Budget Office estimates over 14 million more people will be uninsured by 2034.
3. In terms of the uninsured’s economic status, 85.1% reside with working families, 73.8% have at least one full-time worker in their household and 80.1% are low income.
4. The uninsured disproportionately live in the 10 non-expansion states. Forty-two percent of uninsured individuals live in these states, resulting in an uninsured rate of 14.5% in non-expansion states versus 8% in expansion states.
5. The majority (63.7%) of uninsured individuals are people of color, and 41.9% of the uninsured population is Hispanic.
6. Texas had the highest uninsured rate at 19.2%, and Massachusetts had the lowest at 3.3%.
7. One in 4 uninsured people were not U.S. citizens.
8. Over 40% of uninsured adults did not have a consistent venue to seek medical advice or receive care while sick.
9. Nearly 60% of the uninsured said either they or someone they live with struggled to pay for healthcare.
10. Over half of those who are uninsured could be eligible for Medicaid or subsidized marketplace coverage but did not have it.
11. Nearly 40% of adults without health insurance in the three years leading up to 2024 said it was due to a job loss or new employer. About one-quarter said they were no longer able to access Medicaid, the Children’s Health Insurance Program or another form of public coverage. Cost increases, missed deadlines and age were other explanations.
The post 11 things to know about the uninsured population: KFF appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
We don’t just need more nurses. We need more leaders to train them.
With the United States facing an estimated deficit of more than 250,000 registered nurses by 2028, the nursing shortage is seemingly hard to escape right now: It is dominating headlines, part of policy debates and seen in the lived experiences of anyone who has waited for hours in an understaffed emergency room. But for all the attention this crisis receives, we’re not talking enough about what’s driving it. Beyond the bedside nursing shortage, there is a growing deficit of advanced practice providers, clinical educators, and nurse leaders who oversee care delivery and manage healthcare teams. These are the professionals who train the next generation of nurses — and without them, we risk slowing down the talent pipeline significantly.
The numbers are stark. According to the American Association of Colleges of Nursing, more than 65,000 qualified applicants were turned away from nursing programs in the most recent academic year, largely because schools lack the faculty to teach them. The national nursing faculty vacancy rate currently hovers near 7%, with nearly 1,700 positions unfilled. More than a third of current nursing faculty are over age 60, and a wave of retirements is accelerating the shortage. Meanwhile, faculty salaries trail clinical roles by 20% to 30%, making it difficult to attract doctoral-prepared nurses to academia when they can earn significantly more in practice.
This creates a vicious cycle: Too few educators mean too few seats in nursing programs, which result in too few graduates entering the workforce. At this rate, the bedside shortage will only keep growing. Breaking that cycle requires making graduate nursing education more accessible — not only for the students who need advanced degrees, but also for the faculty we need to keep teaching. Online graduate programs offer one of the most effective paths to doing both.
Yet these programs can face resistance. Critics question whether virtual formats can adequately prepare clinicians for the realities of patient care. Too often, online programs are treated as a pandemic-era stopgap, rather than a legitimate long-term model. That skepticism comes at a real cost. For licensed nurses looking to advance their careers — by pursuing a Master’s, a Doctor of Nursing Practice, or a specialized certification — traditional in-person graduate programs remain a significant barrier. Many are working full time, raising families, or living in rural areas far from academic medical centers. The same constraints also apply to many faculty members. By reducing the burden of regular travel and rigid scheduling, we can attract and retain experienced educators and make the profession more attractive and accessible to the next generation.
Online graduate programs remove those barriers without compromising rigor. The most impactful models do so not by abandoning hands-on learning, but rather by incorporating it strategically. A hybrid approach is most effective because it combines high-quality online coursework with intentional on-campus immersion experiences, like direct faculty mentorship and simulation training. This allows students to gain the flexibility they need without sacrificing the experiential learning required to be prepared for a clinical environment.
Like many areas of higher education, online nursing instruction became more prevalent in reaction to the COVID-19 pandemic. But for some institutions, virtual education is far from new. At The University of Texas Medical Branch, our School of Nursing has spent more than a decade developing and refining virtual instruction for graduate nursing students. Over a decade ago, we implemented a quality improvement program using videoconferencing via FaceTime to conduct virtual clinical site visits.
Across 492 visits over three semesters, faculty, students and preceptors all found the virtual format to be an effective way to evaluate student progress, with more than 85% of stakeholders reporting satisfaction and an estimated savings of nearly $142,000 (compared to in-person clinical site visits). We also consistently see high certification exam pass rates. The approach has worked so well that additional graduate tracks adopted it independently. When the pandemic hit and institutions scrambled to move online, UTMB had years of established protocols to draw from — and as a result, other programs in Texas, as well as nationally and internationally, even reached out to us for guidance.
Online graduate nursing programs are not a workaround. They are a proven workforce development engine — one that expands access for students, eases the burden on faculty and introduces future practitioners to telehealth workflows before they ever enter practice. Solving the nursing crisis requires more than recruiting new graduates; it requires investing in the nurses we already have and giving them accessible paths to advanced degrees, leadership roles and teaching careers. Institutions need to commit to building and funding online graduate programs, and accrediting bodies need to evaluate them on outcomes rather than format. Online graduate programs have been building toward this moment for years. Now it’s time to fund them, scale them and treat them as what they are: one of the most effective tools we have to solve the nursing crisis.
The post We don’t just need more nurses. We need more leaders to train them. appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Closing the gaps: How connected technology is reshaping specialty medication access
Health systems and specialty practices are under increasing pressure to accelerate patient access to therapies. Fragmented workflows, disconnected systems and administrative work continue to slow that process.
During a recent webinar hosted by Becker’s Healthcare and CoverMyMeds, leaders from CoverMyMeds and Ontada explored how integrated technology and AI-powered automation can streamline specialty medication access and improve outcomes for both patients and care teams.
Here are four key takeaways from the conversation.
1. Fragmentation is the core barrier
Both Miranda Delatore DNP, RN, NEA-BC, vice president of product at CoverMyMeds, and Molly Brady, RN, BSN, director of customer success at Ontada, identified fragmentation as the root cause of delays in specialty therapy starts. Care teams are navigating a patchwork of EHRs, payer portals, faxes, emails and spreadsheets to complete a single medication access workflow.
“None of these tools were really designed to work together,” Miranda said. “By default, clinicians have ended up acting as this integration layer and we all know that’s definitely not why they went to school.”
She noted that roughly 60% of clinicians still cite phone calls, emails and manual EHR data entry as among their most time-consuming daily tasks. These administrative delays often translate directly into clinical delays.
Molly echoed this from the oncology practice level, describing a recent clinic visit. “The care team was literally going to the order in the EHR, looking at the practice management system, into the payer portal just to complete the approval step tied to a single treatment plan.”
In oncology, where timing directly affects outcomes, those gaps have real consequences. “Delays in treatment create more stress for those patients, and they force clinics to adjust infusion schedules, chair time and staffing,” Molly said. “When those workflows aren’t connected, those delays are absolutely unavoidable.”
2. The cost of administrative work
The complexity behind a single therapy start spans benefits investigation, prior authorization and patient support enrollment. Each step often requires accessing multiple disconnected systems.
Inconsistent data formats, repeated information requests and manual re-entry create inefficiencies and increase the risk of error.
“Everyone is dependent on having the full story around the patient, and we’ve not enabled them in a way to have access to that consistently,” Miranda said.
The responsibility falls heavily on care teams working directly with patients facing serious diagnoses. “These are the people that are often face-to-face with a patient who’s carrying the weight of a really heavy diagnosis,” she said. “I believe that’s where health systems are really feeling this friction.”
Beyond the human impact, the inefficiency is costly. Health systems are allocating staff time to administrative tasks that pull them away from direct patient care, a dynamic many organizations are working to reverse.
3. Integration enables scalable improvement
CoverMyMeds is addressing fragmentation by bringing benefits investigation, prior authorization and patient support enrollment into a single connected experience embedded within the EHR.
“When an EHR can automatically surface the right information and pre-populate what’s needed, it dramatically reduces the amount of manual input that’s required,” Miranda said. “That alignment reduces the delays caused by missing or mismatched fields and leads to more complete submissions on the first try.”
She emphasized that the goal is to support existing clinical workflows rather than change them. By integrating tools directly into the EHR, care teams can stay focused on patients instead of navigating multiple systems.
4. AI and automation
Both speakers distinguished between automation and AI, noting that each plays a specific role in improving workflows. Automation addresses repetitive, structured tasks, while AI helps interpret unstructured clinical data and align it with payer requirements.
“Think about taking clinical notes or nuanced documentation and mapping that information to complex payer requirements,” Miranda said. “Those are areas where today clinicians spend a lot of time hunting and pecking in the chart.”
The platform’s design reflects a balance between efficiency and oversight: technology operates in the background while clinicians retain visibility and control over decisions.
For health system leaders, the starting point is clear. Organizations should assess current workflows, benchmark performance and identify gaps in interoperability across providers, pharmacies and payers.
“Understand the impact to patients first,” Mirand said. “Technology really connects and works in the background but ultimately the clinical teams always have the oversight to make the decision to move forward. The value is to reduce friction — but not to introduce uncertainty.”
The post Closing the gaps: How connected technology is reshaping specialty medication access appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 metros with highest, lowest healthcare spending per person
Per-person healthcare spending among people with employer-sponsored insurance averaged $6,711 nationally in 2022, though this figure varies significantly by geography, according to an April 9 report from the Health Care Cost Institute.
To compile the report, the nonprofit research institute analyzed spending data across 269 individual metro areas in 45 states, examining the price, use and mix of services for people with employer-sponsored insurance.
Prices accounted for the most spending variation across markets, and high outpatient hospital spending was the strongest predictor of overall spending. Of the 269 markets included in the analysis, 88% had highly or very highly concentrated hospital markets, where less competition tends to drive prices higher, according to the report. Only 3% of markets were unconcentrated and all in major cities such as Chicago, Los Angeles and New York City.
All 10 of the highest-spending metro areas had prices above the national average. In addition, of the 102 metros with above-average overall spending, 93 also had above-average outpatient spending.
10 highest-spending metro areas:
- Charleston, W.Va.
- Anchorage, Alaska
- Janesville, Wis.
- New York City
- Huntington, W.Va.
- Springfield, Ill.
- Racine, Wis.
- Green Bay, Wis.
- Champaign, Ill.
- Gettysburg, Pa.
10 lowest-spending metro areas:
- Bakersfield, Calif.
- Tucson, Ariz.
- Riverside, Calif.
- Fayetteville, Ark.
- Flagstaff, Ariz.
- Morristown, Tenn.
- Knoxville, Tenn.
- San Luis Obispo, Calif.
- Fort Smith, Ark.
- Johnson City, Tenn.
View the full report here.
The post 10 metros with highest, lowest healthcare spending per person appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
6 discharge lounge best practices
More hospitals and health systems are leaning on discharge lounges to decongest EDs and improve patient experience, but there are no industrywide procedures for setting up a lounge.
The first lounges were piloted around 2020 and have gained popularity over the last few years. Palos Heights, Ill.-based Northwestern Medicine Palos Hospital opened its discharge lounge in December 2022. Within a year, the lounge cut average ED wait times down to one hour, cut the number of patients left without being seen by 49% and improved both inpatient and ED patient experience scores.
Becker’s spoke with Rebecca Baute, BSN, RN, chief nurse executive, and Brittany Barasa, DNP, RN, manager of patient care of nursing throughput and patient care tech float pool, in an upcoming Becker’s Healthcare “Clinical Leadership Podcast” to discuss the best practices for setting up a successful discharge lounge.
Here are the six best practices they recommend:
1. Having the right staff run the lounge is critical, Ms. Baute said. Their lounge is run by a dedicated, tenured registered nurse who can work independently and has strong critical thinking skills, along with a patient care technician. These staff are prepared to recognize when a patient decompensates and needs to be readmitted, and can review charts, identify potential discharges proactively and understand where bottlenecks are likely to occur.
2. Setting clear expectations and having an in-depth orientation ensures the discharge staff can work independently from day 1. Discharge staff participate in the same annual skills days as the hospital’s med-surg and step-down nurses to ensure they have the same training and exposure to products and tools, Ms. Barasa said. Leaders also connected discharge staff with the physical therapy team to train them in body mechanics, so that staff could better help patients go from stretchers or wheelchairs into cars. This prevents injury for the discharge staff and provides a safer environment for patients.
3. Discharge lounges should be close to an exit where ambulance partners and families can pull right up and have a direct path to patients. That ease of access makes a real difference, Ms. Baute said. At the same time, having proximity to clinical support means the discharge staff is surrounded by other nurses who can respond quickly if a patient’s condition worsens.
4. Patient comfort is also vital, since some patients spend hours in the lounge. The hospital provides quiet packs that include earplugs, eye masks, crossword puzzles and other items to keep patients comfortable and entertained. The lounge also has access to a restroom, and space for medical supplies and equipment.
5. The lounge is open Monday through Friday from 9 a.m. to 5:30 p.m. At the beginning of each day, the team reviews all patients with current discharge orders and uses a team chat that includes discharge lounge staff, charge nurses and relief charge nurses, to identify patients that are ready to be sent to the lounge. Patients are transferred to the lounge, where they then receive education, the after-visit summary, medication and are discharged. During slow periods, the lounge staff rounds on units proactively to assist with discharge and bringing patients to the lounge.
6. Communication across the organization is key. “Interdisciplinary teams need to understand the why behind the discharge lounge,” Ms. Baute said. “Much of the time, the purpose is to decompress the emergency department, and a surprising number of people across the organization don’t realize that we may have 40 patients holding in hallways. Without that shared understanding, teams won’t consistently use the lounge as the resource it’s meant to be.”
Communication also includes constantly reviewing and expanding the patient criteria over time to meet the current needs or the organization.
The post 6 discharge lounge best practices appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
36% of Americans turn to social media for health information: Pew
About one-third of Americans say they get health information from social media, while a smaller but growing share turn to artificial intelligence chatbots, according to an April 7 analysis from Pew Research Center.
The findings, based on a survey of 5,111 adults conducted in October 2025, highlight how digital platforms are reshaping where people seek health advice, even as concerns about accuracy persist.
Here are seven key findings from the analysis:
- Roughly 36% of U.S. adults report using social media for health information at least sometimes, compared with 22% who say the same about AI chatbots. Both sources trail more traditional avenues such as healthcare providers (85%) and major health websites (60%).
- Users of both social media and AI chatbots are more likely to describe these tools as convenient rather than reliable. For example, 40% of social media users say health information on those platforms is highly convenient, but only 7% consider it highly accurate.
- Similarly, about half of chatbot users say the information is convenient, and 41% say it is easy to understand. However, opinions on accuracy are mixed, with slightly more users saying chatbot information is not accurate than those who say it is.
- Younger adults are more likely than older Americans to use both sources. About 52% of adults under 30 say they get health information from social media at least sometimes, compared with 21% of those 65 and older. For AI chatbots, about 32% of adults ages 18 to 29 report using them for health information, versus 10% of those 65 and older.
- The report also found disparities tied to income and insurance status. Americans without health insurance are somewhat more likely to rely on social media and chatbots for health information than those with coverage.
- Despite their accessibility, both platforms fall short on personalization. A majority of social media users — 59% — say the health information they encounter is not personalized, while 47% of chatbot users say the same.
- There is also significant overlap between the two groups: 61% of people who use AI chatbots for health information also report using social media for the same purpose.
The post 36% of Americans turn to social media for health information: Pew appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Nurse job satisfaction drops after 3-year recovery: Survey
In a reversal of a three-year trend, job satisfaction among nurses is declining and more are considering leaving the profession, according to a recent survey of 2,090 nurses.
Nurse.org, a news and educational website focused on the nursing profession, surveyed its audience of active nurses and nursing students in February and March. Because the respondents are Nurse.org’s audience, the organization said April 6 the survey results are not a nationally representative sample.
Nurse.org has conducted this survey annually since 2022 to track national trends in job satisfaction, burnout and other workforce trends. Here are five key findings from this year’s survey:
1. Plans to leave: Twenty-three percent of nurses said they are at least somewhat likely to leave the profession within the next year.
2. Job satisfaction: In the 2026 survey, 47% of nurses said they were satisfied with work, representing a decrease from the 55% who said the same in 2025.
While the percentage is an improvement from the 2022 survey — when 28% expressed satisfaction — the 2026 results show a stress signal for the future nursing workforce. The least satisfied group was nursing students currently in the workforce, as 18% rated their job a 4 or 5 out of 5.
3. What’s retaining bedside nurses: Approximately 2 in 5 respondents selected financial necessity as a reason they are staying at the bedside despite wanting to leave. Other common reasons include schedule convenience (32%), commitment to patient care (28%) and workplace relationships (24%). Nurses could select up to three choices.
Eight percent cited good management or leadership support as a reason to stay on the job, the survey found.
“Nearly a quarter of nurses staying at the bedside say they’re waiting for a planned career transition or retirement (23%),” Nurse.org said. “The picture this creates is of a workforce that, for many, is staying not because they want to but because they have to. That’s a fragile foundation for retention.”
4. Financial stability: Although 55% of respondents said their compensation increased between 2025 and 2026, 37% said they would go into debt if an unexpected $1,000 expense appeared.
More than one-third (37%) said financial strain has prompted them to work extra shifts or overtime, 15% said they have taken a second job and 8% said financial stress has prompted considerations to leave bedside nursing.
5. Workplace violence: Since the organization’s 2022 survey, reported rates of workplace violence have not improved.
In this year’s survey, 52% of nurses said they have experienced verbal threats or aggressive language in the past year, 27% reported physical assault and 10% reported sexual harassment.
Overall, Nurse.org said nurses remain passionate about their profession but poor workplace conditions “are pushing the needle in the wrong direction again.”
“None of these shifts is catastrophic on its own. But taken together, they suggest that the structural problems facing nursing were not resolved by the brief period of recovery that followed the pandemic. They were, at best, partially and temporarily eased,” the organization said.
The post Nurse job satisfaction drops after 3-year recovery: Survey appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
4 Joint Commission moves
So far in 2026, The Joint Commission — the oldest and world’s largest standard-setting and accrediting body in healthcare — has launched two outcomes-driven certifications and condensed serious safety event lists.
Here are four updates the accrediting body has announced since January, starting with the most recent:
1. The organization launched its first outcomes-driven certifications March 30: one for perinatal care and the other for cardiac procedures. The perinatal care certification will evaluate hospitals’ maternal and newborn outcomes and patient care experiences, and the cardiac certification will assess operation-specific outcome measures, readmissions and patient experience data.
2. Two of The Joint Commission’s affiliate organizations named new board members March 9. Adolfo Llinás, MD, chief medical officer of Fundación Santa Fe de Bogotá in Bogotá, Colombia, joined the Board of Joint Commission Resources. Sarita Mohanty, MD, president and CEO of the SCAN Foundation in Long Beach, Calif., joined the National Quality Forum Board.
3. The Joint Commission and the National Quality Forum plan to align their serious safety reporting frameworks. The accrediting body will adopt the NQF’s Serious Reportable Events List across all accredited domestic and international organizations, effective Jan. 1.
4. The National Association for Healthcare Quality and The Joint Commission rolled out a new regulatory and accreditation micro-credential for practical survey readiness. The self-paced program trains healthcare professionals to interpret standards, manage surveys and sustain corrective actions.
The post 4 Joint Commission moves appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Best, worst states for children’s healthcare
Massachusetts is the best state for children’s healthcare, WalletHub found.
The personal finance website compared the 50 states and District of Columbia across three dimensions: kids’ health and access to healthcare; kids’ nutrition, physical activity and obesity; and kids’ oral health. Each state was evaluated using 33 metrics, which was graded on a 100-point scale, with 100 representing the best care. The data included measures for children and younger.
Here are the best and worst states for children’s healthcare, along with their total score:
Best states
- Massachusetts: 67.34
- Rhode Island: 61.77
- Connecticut: 60.91
- Vermont: 60.90
- Hawaii: 60.74
- New Jersey: 60.32
- Pennsylvania: 58.17
- New York: 57.41
- Iowa: 57.01
- California: 56.25
Worst states
- Mississippi: 37.69
- Arizona: 41.36
- Alaska: 42.20
- Montana: 42.91
- Kentucky: 43.98
- Wyoming: 44.09
- Georgia: 44.59
- Texas: 44.63
- Oklahoma: 44.72
- Arkansas: 45.02
The post Best, worst states for children’s healthcare appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Top medical schools for 2026, per US News
U.S. News & World Report published its 2026 best medical schools list April 7 as part of its Best Graduate Schools rankings.
Medical schools were ranked on a four-tier system, with overall scores calculated based on percentile performance compared to all rated schools. U.S. News created two separate lists — best medical schools for research and best medical schools for primary care — both of which evaluate schools on faculty resources and entering students’ academic credentials.
Tier 1 schools have the highest rankings, falling in the 85th to 99th percentile. U.S. News surveyed 203 medical schools, including 102 that qualified for research rankings and 99 for primary care.
The research list included metrics such as research activity and total NIH research grants, while the primary care list included metrics such as medical school graduates practicing in primary care specialties.
Schools that declined to participate or lack sufficient data were labeled unranked. Peer and residency assessment surveys were not used in the medical school rankings. Learn more about the methodology here.
Here are the highest-performing medical schools for 2026, in alphabetical order, per U.S. News:
Tier 1 medical schools for research
- Baylor College of Medicine (Houston)
- Case Western Reserve University (Cleveland)
- Emory University (Atlanta)
- Mayo Clinic Alix School of Medicine (Rochester, Minn.)
- Ohio State University (Columbus)
- University of California Los Angeles David Geffen School of Medicine
- University of California San Diego
- University of California San Francisco
- University of Colorado School of Medicine (Aurora)
- University of Florida (Gainesville)
- University of Pittsburgh
- University of Rochester (N.Y.)
- University of South Florida Morsani College of Medicine (Tampa)
- University of Texas Southwestern Medical Center (Dallas)
- Vanderbilt University (Nashville, Tenn.)
- Yale University (New Haven, Conn.)
Tier 1 medical schools for primary care
- East Carolina University Brody School of Medicine (Greenville, N.C.)
- Geisel School of Medicine at Dartmouth (Hanover, N.H.)
- Saint Louis University
- University of Arkansas for Medical Sciences (Little Rock)
- University of California Davis
- University of California San Diego
- University of California San Francisco
- University of Hawaii-Manoa John A. Burns School of Medicine (Honolulu)
- University of Kansas Medical Center (Kansas City)
- University of Minnesota (Minneapolis)
- University of Nebraska Medical Center (Omaha)
- University of New Mexico (Albuquerque)
- University of North Carolina at Chapel Hill
- University of Wisconsin-Madison
- Western University of Health Sciences (Pomona, Calif.)
- William Carey University College of Osteopathic Medicine (Hattiesburg, Miss.)
The post Top medical schools for 2026, per US News appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Top graduate nursing programs for 2026: US News
U.S. News & World Report released its 2026 rankings of the nation’s best graduate nursing programs April 7, with Johns Hopkins University in Baltimore and Emory University in Atlanta topping the lists for Master of Science in Nursing and Doctor of Nursing Practice programs, respectively.
The rankings are part of U.S. News‘ broader Best Graduate Schools rankings, which evaluate programs across disciplines including business, education, law, engineering, medicine and nursing using a combination of statistical indicators and peer assessments.
For nursing, the rankings evaluated in-person, hybrid and flexible MSN and DNP programs using data submitted in late 2025 and early 2026 from 682 accredited institutions. Of those, 147 MSN and 154 DNP programs met eligibility criteria, including accreditation and minimum enrollment thresholds.
The methodology incorporates 15 indicators across areas such as faculty resources, research activity, program size, student selectivity and peer and professional assessments. Weighting for these indicators remains unchanged from recent editions.
Across all graduate disciplines, U.S. News bases rankings on a mix of expert opinion and quantitative measures of academic quality and outcomes, including inputs such as student qualifications and outputs such as graduate success.
The full methodology can be found here.
Note: The lists include ties.
The 10 top nursing schools for master’s degrees:
1. Emory University Woodruff (Atlanta)
2. Johns Hopkins University (Baltimore)
3. Duke University (Durham, N.C.)
3. Ohio State University (Columbus)
5. Vanderbilt University (Nashville, Tenn.)
6. University of Michigan (Ann Arbor)
7. New York University—Meyers (New York City)
8. University of Alabama at Birmingham
8. University of California, Los Angeles
8. University of Pennsylvania (Philadelphia)
The 10 best nursing schools for DNPs:
1. Johns Hopkins University (Baltimore)
2. Emory University Woodruff (Atlanta)
3. Rush University (Chicago)
4. Duke University (Durham, N.C.)
4. University of California, San Francisco
4. University of Michigan (Ann Arbor)
4. University of Washington (Seattle)
8. University of Minnesota Twin Cities (Minneapolis)
9. University of Alabama at Birmingham
9. University of Pittsburgh
The post Top graduate nursing programs for 2026: US News appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Georgia hospital matches donor in $2M campaign
Madison, Ga.-based Morgan Medical Center has kicked off a $2 million capital campaign after it received a $1 million matching challenge grant from an anonymous donor.
The “Growing for You” campaign will fund expansions and upgrades at the 25-bed critical access facility to keep residents from having to travel outside the county for specialized care, according to an April 6 news release shared with Becker’s.
Campaign improvements include a third operating room suite, expanded emergency department treatment rooms, a new laboratory area, a new pharmacy and cardiopulmonary areas and diagnostic imaging enhancements.
“Charitable gifts, including new gifts received through Georgia’s popular rural hospital tax credit program, Georgia Heart, will be matched dollar for dollar up to a total match of $1 million,” the release said.
The post Georgia hospital matches donor in $2M campaign appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Nursing emerges as top pathway to middle-class income
Plentiful job openings and potential six-figure incomes are drawing young Americans to nursing, while prospects in other fields are declining, The Wall Street Journal reported April 1.
While factory work and office jobs were once the most reliable path to the middle class in the U.S., automation, globalized manufacturing and, most recently, artificial intelligence have threatened some of these pathways. Amid this, healthcare has remained largely insulated from the effects of AI on job prospects.
Throughout an uncertain U.S. labor market, nursing offers stability and, for some, prosperity, the Journal reported.
The median annual income for registered nurses is nearly double that of all occupations, at $93,600 compared to $49,500, according to data from the Bureau of Labor Statistics. It rises to $132,050 for nurse practitioners, nurse midwives and nurse anesthetists.
Healthcare was the largest driver of job growth in the U.S. in 2025, while many other industries cut jobs. The trend does not seem likely to change anytime soon: Healthcare could become the largest private-sector employment category within the next decade, according to a March report. Employment of advanced-degree nurses and registered nurses is projected to increase by 35% and 5%, respectively, from 2024 to 2034, according to the Labor Department.
Further, healthcare workers’ earnings have increased nearly twice as fast as non-healthcare workers between 1980 and 2022, especially for nurses, according to an October 2025 research paper published by the National Bureau of Economic Research. Healthcare employee earnings increased 60.1% between 1980 and 2022, compared to 34.1% for non-healthcare workers. For nurses, earnings rose 81.7%.
The post Nursing emerges as top pathway to middle-class income appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 trends in healthcare tech investments and ROI
The return on investment conversation for health technology and AI-powered applications has evolved over the years. Initially a sticky subject without a true answer, IT leaders in many organizations have been able to prove the value of soft ROI and lean into the discomfort of making big investments that indirectly influence the bottom line.
Becker’s Healthcare asked 60+ healthcare technology, financial, clinical and operational leaders about how their organizations measure and track technology ROI and 10 themes emerged, setting the tone for how they’ll evaluate future investments.
The leaders surveyed are speakers at the Becker’s 11th Annual Health IT + Digital Health + Revenue Cycle Conference, Sept. 14-17, 2026 in Chicago. Click here to learn more and register or sponsor.
1. ROI is multidimensional. Financial return is necessary, but not sufficient. The near-universal consensus among IT leaders was that healthcare technology ROI cannot be reduced to a payback period or an internal rate of return calculation. Leaders across the field structure their thinking across clinical, operational, financial, and experiential dimensions simultaneously. The organizations that have advanced furthest have built formal frameworks — scorecards, tiered value models, balanced metric sets — to make this multidimensionality legible to finance committees rather than leaving it as a philosophical disclaimer.
2. Reducing clinician burnout and administrative burden is a primary return. The reclamation of clinician time — from documentation, administrative tasks and the cognitive overhead of poorly designed workflows — is both a moral and financial imperative. Leaders said any technology that adds net burden to providers is not an innovation but technical debt, and the long-term cost of that debt — in turnover, in errors, in disengagement — routinely exceeds the paper savings that justified the investment. If physicians and nurses don’t get meaningful time back, the financial ROI tends to disappoint.
3. Adoption is the gating factor and deployment is not the same as value. A technology deployed but not used delivers a return of precisely zero. The most rigorous frameworks treat adoption and sustained workflow change as the true leading indicators that value will be realized, not go-live dates or license counts. Organizations that treat implementation as an afterthought will consistently underperform on their technology investments regardless of how sound the underlying solution is.
4. Define success criteria before you buy anything. The leaders most confident in their ROI frameworks share a common practice: they establish the business case, KPIs, and definition of success before procurement, not after. Technology investments fail most predictably when the problem being solved is unclear at the outset, leaving organizations automating broken processes rather than fixing them. The discipline of writing the business case with explicit objectives, scope, and measurable outcomes is the prerequisite for any honest ROI conversation.
5. AI requires a portfolio approach to tracking and measurement. Different categories of AI investment require fundamentally different ROI metrics. Table-stakes AI might be measured by staff satisfaction and retention, AI-enhanced workflows by efficiency and quality improvements, AI-imagined new care models by clinical outcomes like mortality and length of stay, and exploratory AI by its contribution to the innovation pipeline. Applying a single financial threshold across all AI investments will cause organizations to kill the most transformative bets while over-investing in incremental ones.
6. Risk reduction and cost avoidance must be quantified. Cybersecurity investments, patient safety tools, and regulatory compliance technology generate returns through costs and harms avoided rather than revenue generated, and these returns are chronically undervalued in ROI conversations. Preventing a serious adverse event, a ransomware disruption, or a regulatory penalty can dwarf the savings from efficiency-focused technology. The challenge is not recognizing this intellectually but building the analytical discipline to put numbers on avoided outcomes before the board, not after the incident.
7. The best technology disappears into the workflow. Truly valuable technology becomes invisible; it quietly removes friction rather than adding a new interface layer that clinicians must navigate around. If a solution is generating frequent complaints in the months after go-live, the end users are feeling frustrated by it instead of relieved. Organizations that consistently realize technology ROI treat workflow integration as a primary design constraint with the potential to unlock real value over time.
8. Trusted data and real-time analytics are the connective tissue. A consistent view is that technology without trusted data creates no value regardless of how capable the underlying tool is. The system-level return from technology accrues when clinical, operational, and financial leaders can act on high-quality, timely information, shifting institutions from reactive to proactive postures. Building that data foundation is often less visible than deploying a new application, but it is what determines whether the application’s ROI is theoretical or real.
9. Patient outcomes and access are the ultimate standard. Across clinical leaders in particular, there is a consistent anchoring of ROI definitions to measurable improvements in outcomes, access, and quality of life for patients with financial returns treated as instrumental, a means of sustaining the mission rather than the mission itself. Technologies that cannot demonstrate impact on those dimensions will eventually struggle to justify themselves regardless of their operational efficiencies. The ultimate measure of healthcare technology ROI is lives improved or saved.
10. Speed to value and total lifecycle cost both matter. The speed of value delivery is a component of ROI. An investment that doesn’t yield returns for two years costs the organization real capital in the intervening period and weakens the case for the next transformation initiative. IT leaders are now advocating for full lifecycle cost analysis of new technology that accounts for implementation, training, ongoing support, and optimization. Organizations that consistently win on technology ROI model both dimensions and build the organizational change capacity to accelerate realization, not just the analytical capacity to measure it.
The post 10 trends in healthcare tech investments and ROI appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Fortune’s 17 best healthcare companies to work for
Seventeen healthcare organizations landed on Fortune’s 2026 list of the “100 Best Companies to Work For.”
Fortune partnered with Great Place to Work, a people analytics firm, to create the list. The firm surveyed employees at various organizations, gathering qualitative and quantitative feedback about workplace culture by asking them to rate 60 statements on a five-point scale and answer two open-ended questions. The list is based on employee feedback, and companies with the broadest sets of employees reporting positive experiences earn the highest rankings.
Employers must have 1,000 or more U.S. employees and be nongovernment organizations to be considered. Great Place to Work received more than 1.3 million survey responses in the last year, including more than 640,000 from employees at eligible companies.
The healthcare organizations featured include health systems, pharmaceutical companies and healthcare services companies.
Here are the 17 healthcare organizations that made Fortune’s list, along with their rank out of 100 and headquarters city:
22. Brightview Senior Living (Baltimore)
26. Scripps Health (San Diego)
27. AbbVie (North Chicago, Ill.)
34. Texas Health Resources (Arlington)
39. Hackensack Meridian Health (Edison, N.J.)
40. CHG Healthcare Services (Midvale, Utah)
45. Baptist Health South Florida (Coral Gables)
55. Stryker (Portage, Mich.)
58. Merck (Rahway, N.J.)
61. Elevance Health (Indianapolis)
65. Vertex Pharmaceuticals (Boston)
68. United Therapeutics (Silver Spring, Md.)
70. SCAN Health Plan (Long Beach, Calif.)
75. Atlantic Health System (Morristown, N.J.)
77. Shields Health Solutions (Stoughton, Mass.)
97. Jackson Healthcare (Alpharetta, Ga.)
98. Wellstar Health System (Marietta, Ga.)
The post Fortune’s 17 best healthcare companies to work for appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
What health questions are people asking Microsoft Copilot?
Nearly 1 in 5 people who turn to Microsoft Copilot for health information discuss personal symptoms or conditions, the tech giant found.
Microsoft analyzed more than 500,000 deidentified health-related conversations to reveal what people are aiming to find out.
Nationwide, consumers are increasingly seeking medical advice from AI chatbots, while some researchers are calling for a “humble” AI framework that isn’t so authoritative (the technology still often gets things wrong):
Here are seven key findings from the March 10 Microsoft Copilot report:
1. Nearly 20% of conversations involve personal symptom or condition discussions, indicating strong demand for individualized health guidance
2. The largest category — general health information (40%) — is heavily focused on specific treatments and conditions, suggesting true personal health intent may be higher.
3. About 1 in 7 personal health queries are about someone else (e.g., child, parent, partner), highlighting AI’s emerging role as a caregiving support tool.
4. Personal symptom and emotional health queries spike during evening and nighttime hours, when access to traditional care is limited.
5. Device usage differs significantly: Mobile is dominated by personal health concerns, while desktop skews toward professional and academic use.
6. A notable share of queries centers on healthcare navigation, including finding providers and understanding insurance, underscoring persistent system friction.
7. The findings point to implications for platform design, safety and responsible development of health AI tools.
The post What health questions are people asking Microsoft Copilot? appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
What it takes to sustain engagement among Gen Z nurses: 6 things to know
Generation Z nurses require more frequent one-on-one interaction with managers and leaders than prior generations to maintain similar levels of engagement and retention, according to a March 25 report from Laudio and the American Organization for Nursing Leadership.
“Engaging and Retaining Gen Z Nurses: Trends and Strategies” draws on data from Laudio’s workforce analytics platform, spanning nearly 100,000 registered nurses and their managers across more than 150 hospitals and health systems, along with interviews with nurse leaders. It examines how the fastest-growing segment of the nursing workforce is reshaping expectations around leadership, scheduling and career development.
Six key findings:
1. Gen Z now represents the second-largest cohort of nurses in health systems and is the only generation increasing its share, signaling a continued shift in workforce dynamics as older cohorts retire or exit.
2. Compared with other generations, Gen Z nurses require about 2.5 times more meaningful interactions with frontline leaders each month to achieve similar engagement and retention outcomes. These interactions typically included one-on-one check-ins, recognition and feedback.
3. Retention is strongest in the first two years of employment, a period typically supported by residency programs and structured onboarding. After roughly 30 months, turnover among Gen Z nurses rises above that of other generations, suggesting the necessity of reinforced engagement once formal support programs taper off.
4. Gen Z nurses are more likely to cluster shifts to create longer stretches of time off and are more consistent about taking meal breaks. While these patterns may support work-life balance, the report also notes they could contribute to fatigue and burnout over time.
5. Early-career movement into certain specialties, such as critical care, is occurring alongside slower entry into others, including rehab and therapy roles. At the same time, Gen Z nurses are stepping into charge nurse and assistant manager roles at rates comparable to prior generations, indicating a stable early leadership pipeline.
6. Interviews with nurse leaders at high-performing organizations identified five priorities for engaging and retaining Gen Z nurses: personalizing professional development, reducing administrative friction, modernizing communication channels, offering greater scheduling flexibility and strengthening mental health support. Together, these efforts reflect a broader shift toward more individualized and continuous engagement strategies.
The post What it takes to sustain engagement among Gen Z nurses: 6 things to know appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
AI Won’t Improve Care Quality Until Your Workforce Is Ready
In conversations with healthcare executives nationwide, I’m hearing a consistent theme: their organizations are investing heavily in AI to address capacity constraints and improve care quality, but getting clinical teams to use these tools effectively remains one of their biggest hurdles. Not the technology itself—the workforce’s readiness to leverage it.
We wanted to understand if this was systemic. So, we developed the Covista Care Capacity Monitor—a national study fielded by Gallup across all 50 states, surveying more than 1,300 clinicians and 160 healthcare executives.
What the Data Reveals
The adoption is real: 71% of healthcare organizations now use AI for clinical documentation, 54% for EHR interactions and 46% for diagnostics. Three-quarters of executives say AI has a positive impact on care quality. And 65% say AI can help address staffing shortages at least somewhat. The technology is working.
The hiring bar is shifting: 64% of healthcare executives say AI fluency now factors into recruiting decisions for physicians—57% for NPs and PAs, 49% for RNs. Nearly 60% also report that most of their existing clinical workforce needs upskilling or reskilling in these same technologies.
The priority gap tells its own story: 74% of clinicians say staffing is the problem, and only 34% prioritize technology improvements. Yet 63% say they want AI training. Those things aren’t in conflict—but right now, most clinicians aren’t seeing them as connected.
The Real Priority: Care Quality
When we asked healthcare executives about their top priorities for 2026, achieving adequate staffing ranked first, cited by 87% as a major priority.
The reason? Staffing shortages are negatively affecting care quality. 73% of healthcare executives and 76% of clinicians say staffing shortages negatively affect their ability to deliver high-quality care. Half of executives say shortages have reduced their capacity to serve patients.
From my vantage point preparing healthcare’s future workforce, these challenges are more connected than they may appear. Health systems have already made the AI investment—and are planning more. The workforce readiness investment is what unlocks it—getting that technology to do what it was built to do: relieve pressure on stretched teams and improve the quality of care they can deliver.
Most executives already sense this—the overwhelming majority see AI as part of the solution, increasing productivity and offloading the time-consuming administrative work that nurses, doctors and other clinicians deal with today. But the single biggest blocker right now is human capital: professionals who are fluent in these tools, can use them responsibly and help lead change within their health systems.
Our healthcare partners tell us that when clinicians are trained to use AI effectively, they can focus more attention on the aspects of care that require human judgment and connection. AI handles documentation, manages knowledge overload and surfaces what needs attention. Clinicians do what only clinicians can: exercise judgment, build trust and care for patients. The implementations that work are ones where staff understand what the technology is doing—and what it isn’t. Opacity breeds resistance. Transparency and training remove it.
Without readiness, the opposite happens. Experienced clinicians adopt new AI tools while managing full patient loads with minimal training time, creating stress and resistance. Newly hired staff need extensive AI onboarding, pulling experienced clinicians away from patient care.
The result? Underutilized technology. Frustrated staff. And care quality challenges remain unsolved.
What’s Actually Required
Getting there requires curriculum change that moves with urgency—for the next generation of healthcare professionals and the workforce already in place.
Our collaborations with Hippocratic AI, Google Cloud and Hello AI by GE Healthcare serve students pursuing healthcare careers and the health systems and healthcare providers whose staff need upskilling now. We’re developing AI credentials that run alongside traditional curriculum—building fundamental understanding of how AI works, when to trust it, when to question it and how to integrate it safely into clinical judgment.
The most effective approaches require sustained partnerships between healthcare and education providers. Health systems that clearly articulate what “AI workforce-ready” means for their environment give education institutions specific targets. Working together on competency development ensures graduates arrive with skills that match real-world workflows—and creates pathways for current staff to develop capabilities without leaving practice.
The Path Forward
Executives see AI’s value for care quality, but they’re underinvesting in workforce readiness. That gap explains why implementations stall.
The question isn’t whether to focus on staffing or AI adoption or care quality. It’s recognizing these are connected. You can’t hire fast enough to fill the gap. But you can prepare your current and future workforce to leverage AI in ways that help them deliver higher-quality care even while teams are stretched.
The organizations that realize the greatest returns on their AI investments will be the ones that build clinical trust in the technology in advance—through deliberate, sustained workforce preparation.
##
Michael Betz is Chief Digital Officer of Covista, America’s largest healthcare educator serving more than 97,000 students, and President of Walden University, one of Covista’s five institutions.
The Covista Care Capacity Monitor combines survey data from 1,347 clinicians and 167 healthcare executives with labor market analysis from U.S. Census, Bureau of Labor Statistics, Lightcast and IPEDS. Explore the platform at covista.com/research.
The post AI Won’t Improve Care Quality Until Your Workforce Is Ready appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Most health systems lack tools for vendor-agnostic interoperability: Survey
Health IT leaders increasingly see vendor consolidation as central to achieving interoperability, but most organizations lack the tools to fully realize it, a March 24 survey from CliniComp found.
The findings are based on a survey of CIOs conducted by the CHIME Foundation and released by CliniComp. The survey examined how health system leaders view interoperability, including current capabilities, barriers to adoption and expected outcomes.
Here are five key findings from the survey:
- Nearly 90% of respondents said vendor consolidation is critical to their interoperability strategy, while 16% reported their core electronic health record systems currently support vendor-agnostic interoperability.
- Cost and vendor-related challenges emerged as the most significant barriers. About 47% of respondents cited the expense of initial and ongoing integration, while 42% pointed to vendor unwillingness and delays. Many organizations still rely on customized or add-on solutions to bridge integration gaps, the survey found.
- The survey also highlighted how fragmented data environments continue to hinder progress. Nearly half of respondents, 47%, said their organizations have the necessary data, but it remains siloed across disconnected systems. Many view interoperability not as foundational infrastructure, but as a project layered on top of existing systems.
- Despite these challenges, respondents expressed a clear understanding of interoperability’s potential benefits. About 58% cited improved care coordination as a key outcome, while 37% pointed to improved patient safety, reduced medical errors or lower costs and duplication.
- CIOs from hospitals with more than 500 beds reported they are still unable to fully participate in all four core domains of interoperability: sending, receiving, finding and integrating data.
The post Most health systems lack tools for vendor-agnostic interoperability: Survey appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
AI is coming for admin jobs, CFOs say
Artificial intelligence is expected to disproportionately affect routine, clerical and administrative roles, while having a limited near-term impact on overall employment, The Wall Street Journal reported March 24.
The Journal cited findings from a working paper recently published on the National Bureau of Economic Research website. The study, produced with economists from the Federal Reserve Banks of Atlanta and Richmond, surveyed about 750 CFOs across multiple industries between late 2025 and early 2026.
Five things to know:
1. Workers in more highly skilled roles, such as engineers and architects, are more likely to keep their jobs, especially if they can utilize AI, according to the report.
2. John Graham, an economist at Duke University and one of the paper’s authors, told the Journal that employees with jobs that require higher levels of training and education could eventually be affected, “but probably not in 2026.”
3. Regardless of role, AI is unlikely to eliminate a substantial number of roles in the near-term, according to the report. The study found that AI had essentially no employment effect in 2025. In 2026, CFOs expect that AI will reduce their headcount by about 0.4% compared to what it otherwise would have been.
4. Companies with 500 or more employees are more likely to cut routine worker roles, while smaller companies plan to hire more skilled technical workers, according to the report.
5. Another of the study’s authors, Atlanta Fed economist Salomé Baslandze, told the Journal she is optimistic AI will eventually create new types of work. She also expressed concern, however, that many of the roles vulnerable to elimination are stepping stones for moving into the middle class.
The post AI is coming for admin jobs, CFOs say appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
‘We don’t think of it as just a service line’: How 5 health systems integrate behavioral health into core finances
Across five health systems, behavioral health leaders are seeing a fundamental shift in how integration is financed: moving from siloed service lines and short-term funding toward enterprisewide cost strategies.
Rather than treating behavioral health as a standalone service, leaders said systems are embedding it across care settings and budgets, reflecting its impact on overall patient outcomes and utilization.
Arpan Waghray, MD, CEO of Renton, Wash.-based Providence’s Well Being Trust, told Becker’s the shift requires a broader view of where behavioral health fits across the system.
“We don’t think of behavioral health funding as just a service line,” he said. “Our intent is to think about this in a much broader context. So thinking about all the care that’s delivered outside of the behavioral health specialty for patients … and intentionally building these into the operating budgets of every unit.”
Other leaders echoed the importance of embedding behavioral health into core operations rather than treating it as optional.
Elicia Bunch, vice president of behavioral health at Aurora, Colo.-based UCHealth, said integration must extend into financial and operational structures.
“When it’s embedded in our operational budgets, reimbursement strategies and comprehensive patient outcomes, it really does become sustainable,” she said.
Tracey Izzard, vice president of behavioral health services at Norfolk, Va.-based Sentara Health, said the system has structured behavioral health as a horizontal service line that spans care settings.
“It’s where we’re combining our health plan, our ambulatory and our acute care, and we are embedding behavioral health along the way,” she said.
The system’s vertical behavioral health service line includes the behavioral health unit, emergency department, outpatient programs, partial hospitalization, intensive outpatient services and outpatient medication management.
Utilization and costs
Leaders said this shift is driven in part by the significant role behavioral health plays in hospital utilization and costs. Often, patients who could have entered outpatient programs depend on crisis care for social, mental health and substance use needs.
The financial implications are also substantial.
Mental illness costs the U.S. economy $282 billion annually, researchers at New York City-based Columbia University found. Behavioral health conditions are also linked with up to threefold spending increases for individuals with otherwise similar physical disease burden, according to a study published in 2025 in JAMA Network Open.
“Since we are a payer and we’ve been scaling services, our goal is to start to measure that, to see if that reduction other organizations are seeing, if we’re realizing that value,” Dawn Zieger, vice president of psychiatry and behavioral health at Danville, Pa.-based Geisinger, told Becker’s.
Ultimately, leaders frame integration as a mechanism to reduce total cost of care and improve system efficiency. Embedding behavioral health into primary care and other settings is seen as key to reducing avoidable costs.
“Continuing to treat it as a one-off or an ancillary service — that’s where we continue to absorb all of that cost,” Ms. Izzard said. “There’s all that extra cost where we can embed it and where we can work hand in glove with primary care. That’s where we start to see the total cost of care reduced.”
At the system level, leaders also emphasize aligning financial incentives across entities to support integration.
“All those expenses and all those revenues are ultimately the system’s,” Mr. Jones said. “We’re trying to avoid the sometimes perverse incentive of thinking, ‘Well, what’s good for the department versus what’s good for the hospital?’ We are thinking about what’s good for the patient, and then let’s figure out how the finances work behind the scenes.”
Reimbursement challenges
Despite the potential for return on investment, leaders highlighted persistent reimbursement gaps that require alternative financial strategies. In some systems, behavioral health services continue to rely on internal subsidies.
Maurizio Fava, MD, chair of psychiatry at Somerville, Mass.-based Mass General Brigham, said long-standing reimbursement challenges have required systems to step up.
“Our level of reimbursements for services in the state of Massachusetts has always made it hard to actually support the salaries of our clinicians, and so there has always been substantial subsidy of psychiatric services,” he said.
At Geisinger, reimbursement does not cover outpatient services, Ms. Zieger said. She added that fortunately, the system has other specialties including orthopedics and cardiology with a margin to help pay for the services the community needs.
These financial pressures are compounded in systems with a high proportion of Medicaid patients, in which reimbursement rates are typically lower.
“Fifty percent of our payer mix is Medicaid, which is often populations that have social determinants of health challenges,” Ms. Zieger said. “We’re looking really hard at how to optimize our payment, the fee-for-service commercial space and our Medicaid care so that we can make sure we’re able to have sustainable operations. It’s a hard hill to climb.”
To address these gaps, systems are expanding beyond traditional reimbursement models, including community benefit investments and partnerships.
“Last year, we invested in our community benefits almost $2.1 billion across our seven states. So it’s not an insignificant amount,” Dr. Waghray said. “We’re trying to align our Community Health investment dollars in a way that provides them better support and structure.”
The bridge between clinical care and community partnerships is also critical, particularly when working with organizations that may have more favorable reimbursement structures, he said.
Others have worked to align reimbursement models with integrated care delivery.
“That really includes using collaborative care codes, which are funded primarily under the medical plan, and then also supporting traditional behavioral health benefits where that model works best,” Ms. Bunch said. “A key has really been matching the care model to the reimbursement pathway in a way that really optimizes both the clinical and the business model approach to care.”
Philanthropy, high-margin service lines and grants
Leaders also highlighted the importance of partnerships and alternative funding sources. For example, over the past several months, Los Angeles-based UCLA Health, Monterey, Calif.-based Montage Health and Boston Children’s Hospital have received large gifts for behavioral health.
“Philanthropy was used as a source of discretionary funding by each hospital and by each investigator,” Dr. Fava said. “Now we have a single team that oversees fundraising and philanthropy. … There will be donors that are going to say, ‘I would like to fund research in this area,’ and that may lift all boats in terms of philanthropic support across the entire department.”
Bernard Jones, vice president for behavioral and mental health and the psychiatry department for Mass General Brigham, said interventional psychiatry and procedural services can help improve financial sustainability.
“We are particularly interested in those sort of cutting edge services delivered through a department of psychiatry that not only help advance patient care significantly, but are often the most favorably reimbursed,” he said. “So thinking about interventional psychiatry and some of our procedural services, and that’s also a good way within an integrating department to make things financially sustainable.”
Long-term sustainability must be built into financial models, particularly when relying on grants.
Dr. Waghray cautioned against short-term funding strategies that cannot be maintained.
“The worst thing we can do is get some funding or grant and then support somebody for a short duration of time, and then have to take a service, pull the service back, just because there’s no sustainable pathway,” he said.
Systems are increasingly evaluating sustainability at the beginning of grant-funded initiatives to avoid these disruptions.
“So how do we make sure on the other end of the grant we understand exactly what we’re going to be able to do,” Ms. Zieger said. “We know that we’ve got to be nimble on the other side of the grant infrastructure.”
Governance
Financial integration is reinforced through governance structures that align decision-making across the system. Ms. Izzard said cross-functional leadership alignment is critical.
“Having those standard committees where you have the CMOs, COOs and CFOs from all three divisions come together to make decisions on how to best proceed in the behavioral health area — a lot of alignment is met when we meet in those areas, but then we can also see where the divergence is.”
Ms. Bunch added that executive-level prioritization is essential to sustaining progress.
“When behavioral health is represented in executive decision making priority, strategy and financial planning, it really ensures the work remains central to the organization’s mission and strategy, and that is certainly how UC Health has demonstrated this mission.”
Editor’s note: This is the first of a three part series exploring what behavioral health integration looks like financially, clinically and operationally. Check out Becker’s behavioral health newsletter to see more coverage on the topic.
The post ‘We don’t think of it as just a service line’: How 5 health systems integrate behavioral health into core finances appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
20 best small cities for careers
Alpharetta, Ga., is the best small U.S. city for careers, according to a Jan. 13 ranking from CoworkingCafe.
The ranking was developed by analyzing 298 U.S. cities with populations below 250,000. CoworkingCafe evaluated several key metrics on a 100-point scale, including salary, income, cost of living, job market strength, access to healthcare and commute times.
Some of the small cities are also fast-growing communities with new hospital projects, such as Dallas-based Baylor Scott & White Health’s hospital that opened in Frisco, Texas, in July and Arlington-based Texas Health Resources’ hospital in McKinney, Texas, slated to open in 2028.
Here are the top 10 career hotspots with fewer than 250,000 residents, according to CoworkingCafe:
1. Alpharetta, Ga.
2. South Jordan, Utah
3. Mountain View, Calif.
4. Santa Clara, Calif.
5. Palo Alto, Calif.
6. Carmel, Ind.
7. Fishers, Ind.
8. Franklin, Tenn.
9. Kirkland, Wash.
10. Portland, Maine
11. Frisco, Texas
12. Bellevue, Wash.
13. San Ramon, Calif.
14. Boca Raton, Fla.
15. Flower Mound, Texas
16. Troy, Mich.
17. Pflugerville, Texas
18. Richmond, Va.
19. Alexandria, Va.
20. McKinney, Texas
The post 20 best small cities for careers appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
‘Game-changers for their communities’: UAB plans 3rd freestanding ED
Birmingham, Ala.-based UAB Health System is planning a third freestanding emergency department, this time in Oxford, Ala.
UAB St. Vincent’s St. Clair has filed a letter of intent with the Alabama State Health Planning and Development Agency to seek a certificate of need for the project.
The proposed freestanding ED would be developed through a joint venture between UAB Health System, the city of Oxford and Oxford Health Systems, the city’s healthcare authority.
Oxford Mayor Alton Craft said the city’s rapid growth has outpaced its healthcare infrastructure, creating a need for additional emergency services.
“We approached UAB to fill this need in our community because we know they represent world-class patient care,” Mr. Craft said in a March 20 news release. “This project is only the beginning of healthcare transformation in our region.”
UAB Health System CEO Dawn Bulgarella said proximity to care is a key driver of community health outcomes.
“This project expands care options for Oxford and surrounding communities,” Ms. Bulgarella said. “It will enhance access and support continued improvement of health outcomes across the region.”
She added that the partnership would connect patients in the region to UAB’s broader care delivery network, improving access to specialty care while leveraging scale to help manage costs.
UAB Medicine currently operates freestanding emergency departments in Gardendale, Hoover and Trussville.
“Our other freestanding emergency departments have been game-changers for their communities,” Ms. Bulgarella said. “We hope to make this one a reality in partnership with the city of Oxford soon.”
Additional details, including the facility’s location and timeline, are expected to be announced at a later date.
The post ‘Game-changers for their communities’: UAB plans 3rd freestanding ED appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 most, least stressed states
South Dakota was found to be the least stressed state, while Louisiana was the most stressed, according to WalletHub’s annual ranking.
WalletHub compared all 50 states across 4 key dimensions — work-related stress, money-related stress, family-related stress, and health- and safety-related stress — which were evaluated using 40 metrics, ranging from residents’ average hours worked per week to the state’s quality of infrastructure. The health- and safety-related component factored in each state’s share of adults in fair or poor health, with diagnoses of depression, mental health, suicide rate and more. Read more about the methodology here.
Here are the 10 most and least stressed states, along with their overall score out of 100:
Most
1. Louisiana: 62.86
2. Kentucky: 58.18
3. New Mexico: 57.65
4. West Virginia: 56.20
5. Arkansas: 55.60
6. Nevada: 53.82
7. Oklahoma: 53.47
8. Oregon: 52.39
9. Mississippi: 52.16
10. Alabama: 50.99
Least
1. South Dakota: 32.35
2. Utah: 32.61
3. Minnesota: 33.50
4. New Hampshire: 33.51
5. Vermont: 33.77
6. Idaho: 35.12
7. North Dakota: 35.84
8. Connecticut: 36.46
9. Massachusetts: 36.54
10. Iowa: 37.28
The post 10 most, least stressed states appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Viewpoint: US nursing workforce faces several risks
Federal budget policies could put the nation’s nursing faculty workforce under great strain, according to a March 20 JAMA Health Forum viewpoint by two leaders at the University of North Carolina at Chapel Hill.
Proposed changes to the U.S. federal budget emphasize short-term recruitment of clinical nursing staff “without thoughtful consideration for the faculty needed to train more nurses, not only for the present moment, but also for decades to come,” according to the viewpoint.
The piece, “Funding Nurse Recruitment While Defunding Nurse Educators,” is by Joshua Barrett, PhD, RN, the associate director for UNC’s Center for the Business of Health, and Zoey Kernodle, DrPH, the center’s director and a research assistant professor.
The faculty nursing shortage is a significant driver of the nation’s short supply of nursing professionals.
Dr. Barrett and Dr. Kernodle outlined two budget policy proposals that could harm the U.S. nursing workforce long-term:
1. The Nurse Faculty Loan Program
Drafts of the fiscal 2026 budget — H.R.1, which passed in July — included proposed cuts to federal nursing research and workforce development programs. One of those programs, called the Nurse Faculty Loan Program, faced termination but “ultimately received funding,” the viewpoint said. However, “recurring proposals for its elimination suggest its future remains tenuous.”
“During the 2023 to 2024 academic year, U.S. nursing schools turned away 65,766 qualified applicants, primarily due to insufficient faculty,” the viewpoint said. “Without capacity expansion, nursing schools will continue to limit the total workforce regardless of recruitment program success.”
2. Federal loan limits
One compounder to the potential elimination of the Nurse Faculty Loan Program and broader nurse educator shortage are proposed limits to federal student loans.
H.R.1 places a $200,000 cap on federal loans for students in professional degree programs. The Education Department proposed removing nursing programs from the “professional” designation and shifting them to “graduate,” which would limit borrowing to $100,000 for students in Master of Science in Nursing and Doctor of Nursing Practice programs.
DNP graduates account for a significant amount of nursing faculty, the viewpoint said.
“With loan limit reductions and proposed [Nurse Faculty Loan Program] elimination occurring simultaneously, prospective nursing faculty face a double constraint: reduced borrowing capacity for their education and eliminated loan forgiveness for faculty service,” according to the viewpoint.
To mitigate the nursing faculty shortage and support the future nursing workforce, Drs. Barrett and Kernodle said policymakers should stabilize and sustain funding the Nurse Faculty Loan Program and address “the academic-clinical salary differential,” as advanced practice registered nurses earn a median salary of $129,480, compared to the median $93,958 salary for nursing faculty.
The post Viewpoint: US nursing workforce faces several risks appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
‘The 1980s called’: CMS to phase out fax, mail
CMS has finalized a rule to phase out faxing and mailing for healthcare claims documentation.
Four things to know:
1. The Administrative Simplification; Adoption of Standards for Health Care Claims Attachments Transactions and Electronic Signatures Final Rule is projected to save the healthcare industry roughly $781 million annually by establishing national standards for the electronic exchange of clinical documentation, according to a March 20 CMS news release. CMS did not share data behind the estimate.
“The 1980s called, and they want their fax machines back,” CMS Administrator Mehmet Oz, MD, said in the release. “… This new rule will modernize American healthcare by standardizing electronic claims attachments and enabling secure electronic signatures. Because every minute providers save on paperwork is another minute they can spend caring for patients.”
2. The rule also adopts standards for electronic signatures to support the secure, authenticated transmission of claims-related information across healthcare entities.
3. The rule takes effect May 19 and applies to HIPAA-covered entities, including health plans, healthcare clearinghouses and healthcare providers that conduct electronic transactions. Covered entities must comply by May 19, 2028.
4. It establishes the first HIPAA-adopted standards for healthcare claims attachments, allowing for the secure electronic exchange of supporting clinical documentation such as medical records, X-rays and imaging, clinical notes, telemedicine visit documentation and laboratory results, according to a CMS fact sheet.
The post ‘The 1980s called’: CMS to phase out fax, mail appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
How rural hospital CEOs are navigating new healthcare laws in 2026
As rural hospital leaders guide their organizations through 2026, they are juggling the financial pressure of federal Medicaid changes while looking to state legislatures for tools to stabilize their organizations.
From Nebraska’s Medicaid work requirements to New Mexico’s updated physician loan forgiveness initiative, the policy landscape is reshaping how rural hospitals recruit, operate and plan for the future.
Becker’s asked six CEOs which healthcare law or legislative change is most top of mind and how their organizations are preparing.
New Mexico
Several New Mexico bills were signed into law March 6; they are focused on reforming hospital funding, medical malpractice rules and patient billing. David Shaw, CEO of Nor-Lea Hospital District in Lovington, expressed appreciation for the initiatives aimed at enhancing physician recruitment and retention.
“Notably, New Mexico’s anticipated participation in the Interstate Medical Licensure Compact and the revision of the state’s loan forgiveness program for physicians, which increases annual awards to $75,000, represent significant progress,” Mr. Shaw said. “These measures demonstrate that New Mexico is committed to welcoming physicians and valuing their contributions to healthcare.”
Once details regarding the updated loan repayment program are finalized, hospital leadership will prioritize understanding the new provisions so it can inform current providers and integrate the information into recruitment materials, he added.
Nebraska
Superior-based Brodstone Healthcare is preparing for the rollout of Rural Health Transformation Program funds and the changes accompanying HR 1, particularly new Medicaid work requirements, CEO Treg Vyzourek said. The organization is taking an active role in educating the Medicaid population in its region as information is released by the state, he said.
“Nebraska is also taking a more aggressive approach by proposing zero-day retroactive eligibility for patients who may qualify for Medicaid,” Mr. Vyzourek said. “We are highly concerned about the financial impacts of the Medicaid cuts and the implementation of work requirements, especially if zero-day retroactive eligibility is approved.”
Operationally, Brodstone Healthcare anticipates increased costs as a result of added administrative burden associated with the rollout of HR 1 and changes to Medicaid, he added.
Medicaid funding changes are also top of mind for Manuela Banner, RN, president and CEO of Memorial Community Hospital and Health System in Blair.
“We are preparing for increased uncompensated care and continued pressure on already thin margins, while doing everything we can to protect access to essential services in our community,” she said. “While the Rural Health Transformation Program grant is helpful, it was never intended to replace Medicaid dollars and will only go so far in offsetting potential cuts, particularly as a significant portion of the funding in our state is directed to entities that are not hospitals.”
Tim Gullingsrud, CEO of Banner Health’s Ogallala Community Hospital, said the state-directed payment model implemented in 2025 has been transformative in helping to improve its financial performance by raising Medicaid reimbursements.
“However, our top concern for this year is the potential decline in these reimbursements and methodology changes that could threaten our financial stability,” Mr. Gullingsrud said. “We’re also actively working on Rural Health Transformation grant applications to ensure sustainable programs within the five-year funding window, while preparing operational strategies to survive on lower reimbursement rates across all payers.”
In addition to managing reimbursement uncertainty, leaders pointed to disciplined operations and workforce support as priorities.
“Our focus right now is on staying disciplined operationally, supporting our workforce and continuing to advocate for sustainable funding solutions that allow rural providers to keep serving their communities,” Ms. Banner said.
North Dakota
Rural Health Transformation Program funding is one of the biggest areas leaders at Linton Regional Medical Center and Wishek-based South Central Health are closely monitoring, CEO Lukas Fischer, BSN, RN, said.
“These changes have the potential to significantly reshape how rural hospitals deliver care by expanding access to telehealth, care coordination and innovative service models,” Mr. Fischer said. “We are actively aligning our operations and partnerships to take advantage of these opportunities while maintaining financial sustainability. The challenge will be balancing innovation with ongoing workforce limitations that continue to impact rural healthcare delivery.”
Arizona
Gary Kartchner, MSN, RN, CEO of TMC Health’s Benson Hospital and Northern Cochise Community Hospital in Willcox, is focused on how policy changes are affecting access to care, such as uncertainty in Medicaid enrollment and declining affordability in the marketplace, which leave patients at risk of becoming uninsured or delaying care.
“At the same time, cuts to SNAP are increasing food insecurity in our communities, which shows up in worse health outcomes when patients do seek care. We are also seeing growing pressure in bad debt, a clear sign that families are struggling to afford care,” Mr. Kartchner said. “Our focus is on strengthening care coordination and working with community partners to intervene earlier, while continuing to elevate these impacts with policymakers.”
The post How rural hospital CEOs are navigating new healthcare laws in 2026 appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
10 most, least innovative states
Of the 50 states and Washington, D.C., the nation’s capital is the most innovative, according to a ranking from personal finance website WalletHub.
The March 18 list evaluated all 50 states and Washington, D.C., using 25 indicators of “innovation friendliness,” including share of STEM professionals and concentration of technology companies. Metrics were graded on a 100-point scale, and each state’s weighted average was used to calculate its innovation index.
Here are the 10 most and least innovative states, according to WalletHub:
Most innovative
1. Washington, D.C.
2. Massachusetts
3. California
4. Colorado
5. Washington
6. Maryland
7. Virginia
8. Delaware
9. Utah
10. New Jersey
Least innovative
42. Alaska
43. Oklahoma
44. Kentucky
45. Kansas
46. Arkansas
47. Iowa
48. North Dakota
49. West Virginia
50. Louisiana
51. Mississippi
The post 10 most, least innovative states appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
Judge’s ruling on HHS’ vaccine overhaul spurs questions about RSV shot availability
A federal judge’s March 16 ruling blocking much of HHS’ recent vaccine policy overhaul is raising new questions about access to respiratory syncytial virus preventive shots for infants.
In the decision, the U.S. District Court for the District of Massachusetts invalidated actions taken by members appointed to the CDC’s Advisory Committee on Immunization Practices after HHS Secretary Robert F. Kennedy Jr. restructured the panel in June. The court found the committee was improperly constituted and vacated its recommendations, effectively reinstating the prior childhood immunization schedule and limiting the authority of the reconfigured advisory group.
In January, the CDC adopted a revised vaccine schedule that cut the number of vaccines routinely recommended for children and adolescents from 18 to 11.
The March 16 ruling has created near-term uncertainty for clinicians, states and public health officials, who are working to understand its implications for vaccine policy and coverage, The New York Times reported. Experts told the news outlet that the back-and-forth on vaccine policy is fueling confusion across care settings, particularly as the Trump administration is expected to appeal the decision, raising the possibility that the policy landscape could change again within days.
One area of concern is access to monoclonal antibody products that protect against RSV. Because at least one product was added to federal recommendations under the now-invalidated advisory committee, its coverage status is unclear. The disruption could affect whether certain RSV preventive therapies remain available at no cost to eligible children, depending on how federal agencies and payers respond in the coming weeks.
“It would be unfortunate if the court ruling were to limit access to a critical prevention tool for infants and young children, especially as R.S.V. activity is rising, with the highest rates of severe illness among those under age 4,” Robert Hopkins Jr., MD, medical director for the National Foundation for Infectious Diseases, told the Times.
The post Judge’s ruling on HHS’ vaccine overhaul spurs questions about RSV shot availability appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
An issue with hospital executive pay
Nashville, Tenn.-based HCA Healthcare’s executive compensation structure underscores a clear industry reality: financial performance — particularly EBITDA — remains the dominant driver of leadership pay.
According to HCA’s 2025 proxy report, published March 13, 80% of executive incentive compensation is tied to EBITDA performance, with the remaining 20% linked to quality and patient care metrics such as infection rates, mortality and patient experience scores. This weighting reflects a strong emphasis on financial outcomes, even as health systems face increasing pressure to prioritize quality, access and workforce stability.
The structure also reinforces how the for-profit hospital operator defines success.
EBITDA targets are set within a relatively narrow range — with threshold performance at 4% below target and maximum at 4% above — and can yield payouts of up to 200% for that portion of incentives. In 2025, HCA executives achieved near-maximum performance, contributing to total bonus payouts of nearly 196% of target.
For example, HCA CEO Sam Hazen saw his overall compensation increase by $2.7 million in 2025 as the health system reported a $6.8 billion in net income on revenue of $75.6 billion, according to the report. Mr. Hazen earned more than $5.4 million in nonequity incentive plan compensation in 2025.
Notably, quality metrics — while present — are partially dependent on financial performance.
If EBITDA falls below 90% of target, no payout is awarded for the quality portion of incentives. This design positions financial performance as a gatekeeper, even for measures tied to patient outcomes and experience.
The emphasis on financial performance aligns with broader critiques of how hospital economics — and executive incentives — are structured.
Speaking on “The Healthcare Bridge” podcast, Mark Cuban — entrepreneur and co-founder of Cost Plus Drugs Co. — argued that hospital performance is often driven less by operational efficiency and more by market leverage.
“One, I have market dominance, and I get to say, ‘f— you,’ to everybody and the insurance companies, right? I don’t need you, because I’m going to get my own patients too,” Mr. Cuban, who said. “Two, I don’t have enough patient flow, so I need you insurance companies to send me patients, and so I’ll do the deal that you want me to do, because otherwise I don’t have a patient funnel.”
He also suggested that executive compensation structures can incentivize growth for scale rather than long-term sustainability.
“I think part of the challenge is [how] most CEOs are rewarded. Hospital CEOs are rewarded by revenues and scale, and so they default to more buildings,” he said. “If this 100-bed hospital is not my final destination, I want to be the 60-hospital, 6 zillion beds, because that’s where I’m making $10 million a year.”
For hospital and health system leaders, this model — and Mr. Cuban’s critique — highlight a key tension: whether compensation structures are truly aligned with long-term value, or primarily with financial growth and market position.
Editor’s note: Becker’s has reached out to HCA for comment on this story and will update this story as more information becomes available.
The post An issue with hospital executive pay appeared first on Becker’s Hospital Review | Healthcare News & Analysis.
How 3 hospitals are bringing nurses back to the bedside
A rising demand for adequate nurse staffing is pushing some hospitals to expand their recruitment strategies to nurses who had left the bedside.
Adequate staffing made national headlines during the COVID-19 pandemic, and has been a core issue for many hospitals ever since. But in the last year, its importance has become central as studies and organizations hone in on staffing levels as a key issue in the industry.
- A Philadelphia-based University of Pennsylvania survey found the majority of nurses who left bedside roles in recent years are willing to return, and adequate staffing levels are the factor that would reattract them.
- Another study of U.S. magnet hospitals found facilities where nurses report “enough nurses to get the work done” have better physician outcomes.
- The Joint Commission has formally recognized nurse staffing as a national performance goal, meaning hospitals seeking accreditation must meet certain standards related to staffing and oversight.
- Adequate staffing is also still at the center of many union negotiations and nurse strikes.
Becker’s reached out to CNOs to find out if they are actively working on recruiting nurses back to the bedside. Every nurse leader said it is, but the ways they attract nurses back to the bedside differs.
Note: Responses have been lightly edited for length and clarity.
Maribeth McLaughlin, BSN, RN. Chief Nurse Executive and Vice President of Patient Care Services at UPMC (Pittsburg): Every nurse is part of the pipeline. It doesn’t matter whether they’ve left for ambulatory care, virtual nursing, work-from-home, we’re looking to bring any and all of them back to the bedside. As part of that effort, we looked at our education model and asked: how do we build something that supports the new graduate, the brand-new nurse straight out of school, as well as the returning nurse?
What we moved to is a system known as the tiered skill acquisition model. It’s an evidence-based model that allows us to standardize our approach so that everyone receives all the necessary components, while also individualizing it based on where each nurse is in their journey. The tiered structure ensures everyone gets the right resources and materials, but it’s flexible enough to meet each nurse where they are. For a nurse who’s returning to the bedside, probably the biggest challenge is technology. Many returning nurses still have their critical thinking skills intact; it’s really about bringing those skills back to the forefront and getting them current on the technology. We tailor their orientation accordingly.
An experienced nurse who’s been away is still looking for work-life harmony. They’re trying to find what they need to make work fit within their life. That’s where our career ladder and our various programs come in.
We also allow people to come in and shadow. I actually just spoke with a nurse who has been working alongside physicians in research, is moving back to the Pittsburgh region, and wants to explore returning to the bedside. She hasn’t done it in a long time, but she’s feeling disconnected from her patients. We talked about how we could bring her in, let her shadow for a while, and I spent a good amount of time speaking with her individually about this life change, because I think that matters. It’s not just about “come back and get a job.” It has to work within the whole of their life. Making sure it’s a good fit from the beginning is another critical piece of what we do.
Deana Sievert, DNP, MSN, RN. Senior Vice President and CNO at Rush University Medical Center (Chicago): We see tremendous value in recruiting nurses who left the bedside and helping them get back to caring for patients again. While we are fortunate to have many tenured staff who remain at the bedside — speaking volumes to our strong nursing culture — we are still focused on trying to bringing more back into these roles.
For example, we have boomerang campaigns where we reach out to eligible staff who have left and simply invite them back. Sometimes we find that staff end up realizing the “grass is not always greener,” and they are very interested in returning to Rush. We will be adding new, regular touchpoints with those who have left to highlight new opportunities that become available and would be a good fit for a former nurse. The focus there is to keep connecting until something resonates with them to consider returning.
But more importantly, we are working hard to not lose them from the bedside in the first place. Rush is fortunate to have a robust shared governance system in place that helps us work with the tenured staff to better meet their needs. One of the messages we recently received was the need to find different ways to recognize our tenured staff with more than 15 years at the bedside.
We are also working closely with those seasoned nurses to design different staffing models that allow for fewer weekend commitments, fewer holiday commitments and other perks that our nurses have identified as things they would appreciate.
Courtney Vose, DNP, RN. Senior Vice President and CNO of Yale New Haven (Conn.) Hospital: There is only one thing that enhances great nursing — the added value of wisdom and experience. We work in close partnership with our nursing leaders, talent acquisition, finance and marketing to build strong, sustainable pipelines across every care area. Safe staffing, defined by us as staffing that fully accounts for volume, acuity and workload, is our number one priority.
We review our staffing performance three times a day and continuously adjust our plans based on real-time feedback from frontline RNs. This disciplined, data-driven approach strengthens the resilience of our current team, accelerates recruitment and creates the conditions that invite experienced nurses back to the bedside.
The post How 3 hospitals are bringing nurses back to the bedside appeared first on Becker’s Hospital Review | Healthcare News & Analysis.

What to Expect When Working for a Nurse Staffing Agency
Starting a new nursing job in metro Atlanta—or anywhere in Georgia, South Carolina, Alabama, Florida or beyond —can feel overwhelming, even when you know it’s the right move. Working for a nurse staffing agency opens the door to exciting opportunities like travel nursing jobs, per diem nursing positions, and flexible contract nursing assignments, but for many nurses, the process can seem mysterious.
Here’s what to expect and how to prepare so you can start your journey with confidence.
Whether you’re interested in contract nursing jobs, per diem, or full-time placements, the process of joining a nursing agency is straightforward.
- Explore Open Positions
Start by browsing our current healthcare staffing opportunities, including travel nurse contracts and per diem RN jobs across Georgia. You can view all available positions [here]. - Apply and Submit Your Resume
Once you find a role that matches your skills and interests—like emergency department nursing jobs, radiology technologist positions, or ICU contract assignments—submit your application. Our recruitment team reviews your resume to ensure a great fit. - Complete Skills Assessments
After initial screening, you’ll complete online assessments to evaluate your clinical expertise. - Interview and Client Screening
Next, you’ll interview with a recruiter from Staff Relief. Some positions require additional interviews with the hiring facility, especially for rapid response nursing or specialized roles.
The good news? This process typically moves fast—most candidates receive an offer within 9 days of applying.
More Earning Potential
One of the biggest reasons nurses choose agencies like Staff Relief is the pay. Per diem and contract nursing jobs can pay up to 50% more than traditional staff positions. You’ll also have access to the same premium assignments available with leading partners such as Aya Healthcare, AMN Healthcare, and Medical Solutions.
More Flexibility and Freedom
When you work with a nurse staffing agency, you decide when and where you want to work. Whether you prefer travel nurse assignments across the Southeast or local shifts around Georgia, you have control over your schedule.
More Responsibility and Professional Growth
As a contract or per diem nurse, you’ll take on additional responsibilities like tracking time and attendance. While this requires organization, it also builds valuable skills in accountability and independence.
More Variety and Travel
You won’t be tied to one facility. With travel nursing jobs, you can explore new cities, gain diverse experience, and enjoy housing assistance coordinated through agency partnerships.
More Security and Benefits
Even though you’re working flexible assignments, you still receive comprehensive benefits. Staff Relief provides health insurance and other perks so you can feel secure in your role.
If you’re a nurse who thrives in a fast-paced, dynamic environment and values more freedom, higher pay, and a variety of assignments, agency work could be your ideal career path.
Staff Relief partners with major healthcare staffing leaders to offer you access to top contracts and exclusive opportunities. Ready to get started?Contact Staff Relief today to learn more about our per diem nursing jobs, travel nurse assignments, and allied health contracts in Georgia. Let the best nurse staffing agency in Geogia find the perfect fit for your skills and goals.

Travel Nurse Pay in Georgia – Updated
Working as a contract nurse or per diem nurse in Georgia opens doors to flexibility, premium pay rates, and the chance to grow your experience across different healthcare settings. Whether you’re comparing travel nursing jobs, exploring remote RN jobs, or looking into per diem nursing positions, it’s essential to understand the factors that impact your earnings so you can make informed decisions and advocate for fair compensation.
Below, you’ll find everything you need to know about travel nurse pay in Georgia, average hourly rates, and how variables like specialty and location shape your paycheck.
When you partner with a nursing staffing agency or medical staffing agency, you’ll likely choose between contract assignments and per diem shifts:
- Contract Nursing Jobs: You’ll sign an agreement to work a set number of hours over a defined period, such as 8–13 weeks. Many contract nursing jobs offer guaranteed hours, premium rates for urgent needs, and stipends for housing and travel.
- Per Diem Nursing Jobs: “Per diem” means “per day.” These shifts are typically scheduled a week at a time, providing maximum flexibility for nurses who prefer short-term or occasional work. Per diem nurses often receive higher hourly rates to compensate for the lack of long-term commitment and benefits.
Whether you’re drawn to the stability of a contract or the freedom of per diem nursing shifts, you’ll be paid hourly, with rates that can fluctuate based on demand and specialty.
No two assignments are exactly the same. Here are the main factors that determine what you’ll earn as a travel nurse or per diem nurse in Georgia:
1. Location
Urban areas like Metro Atlanta and Savannah typically offer higher compensation compared to rural hospitals and clinics. Travel nurse jobs in Atlanta often pay a premium to attract experienced RNs to high-volume facilities.
2. Specialty
Your area of expertise makes a significant difference. Roles in the emergency department, ICU, operating room, and critical care nursing often command the highest hourly rates. Specialized skills like medical imaging, radiology technologist jobs, or dialysis RN contracts can further boost your earning potential.
3. Experience and Credentials
More years in the field—and specialty certifications—qualify you for higher-paying assignments. Rapid response nursing jobs and crisis response contracts also tend to pay more due to urgency and complexity.
4. Facility Type
Pay can vary depending on whether you’re working in an acute care hospital, skilled nursing facility, outpatient clinic, or rehab center. Some settings offer incentives like retention bonuses or completion bonuses.
5. Travel Requirements
Assignments requiring you to commute 50+ miles often include additional stipends or elevated pay rates to offset costs and time away from home.
While rates fluctuate weekly based on demand and season, here’s what you can generally expect in Georgia:
- General RN: $40–$46 per hour
- General RN (Metro Atlanta): $48–$55 per hour
- Specialty RN (ICU, OR, ED): $55–$75+ per hour, depending on urgency and shortage areas
- Licensed Practical Nurse (LPN): $25–$40 per hour
- LPN (Metro Atlanta): $30–$45 per hour
These figures often include travel stipends and housing allowances. For high-paying travel nursing companies or crisis response contracts, rates can exceed $80 per hour in peak demand.
Some agencies bundle housing and travel reimbursements, while others pay a higher hourly rate without stipends.
Before accepting a contract, review details carefully:
- Hourly base pay
- Housing allowance or provided housing
- Meal and incidentals stipends
- Travel reimbursements
- Completion and referral bonuses
If you’re unsure whether a pay package is competitive, compare it with similar contract nursing jobs.
- Get certified in high-demand specialties like emergency room nurse staffing, ICU nursing, or radiology technologist work.
- Consider rapid response nursing or ICU contract nurse positions for premium rates.
- Pick up flexible options like weekend nursing contracts or extra per diem shifts to maximize income.
- Keep your licenses and certifications current to qualify for the broadest range of assignments.
If you’re ready to explore per diem nursing jobs in Georgia or secure a travel nurse contract with competitive pay and benefits, Staff Relief, Inc. is here to help.
Contact us today to learn more about available contracts and start earning what you deserve.

The Ultimate Guide to Per Diem and Travel Nursing Jobs in the Southeast
If you’re an RN exploring your next career move, you’re not alone. Demand for per diem nursing jobs, travel nursing assignments, and contract nursing positions continues to rise across the Southeast—including Georgia, Florida, Alabama, and North Carolina.
At Staff Relief, we specialize in connecting nurses with flexible, rewarding opportunities at top healthcare facilities. Whether you’re searching for remote RN jobs, weekend nursing contracts, or emergency department nursing careers, this guide will help you understand your options and how to get started.
Per diem nursing offers unmatched flexibility. You can pick up shifts on your schedule—ideal for maintaining work-life balance or supplementing your income. Contract nursing jobs, meanwhile, provide stability for a set duration, often with higher pay rates and benefits.
- Flexible nursing shifts that fit your lifestyle
- The ability to work in acute care, skilled nursing facilities, or inpatient care units
- Opportunities to gain experience in critical care, emergency departments, or medical imaging
- Access to rapid response nursing jobs and crisis response travel nurse contracts that offer premium compensation
- The chance to build your resume with respected employers like Aya Healthcare, AMN Healthcare, and Medical Solutions
Many nurses are drawn to the Southeast for its competitive pay and growing healthcare networks. Here are some popular areas to consider:
- Georgia: From Atlanta to Savannah, per diem nursing jobs in Georgia are in high demand. If you’re wondering how to become a travel nurse in Georgia, Staff Relief can guide you through licensing and onboarding.
- Florida: Coastal communities and urban hospitals alike need RNs for contract nursing jobs in Florida, especially in ICU, OR, and emergency room nurse staffing.
- North Carolina: Explore travel nurse assignments in North Carolina, including rapid response nursing and critical care contracts.
- Alabama: More facilities are offering remote RN jobs in Alabama and local contracts to address staffing shortages.
You have more options than ever to search for your next role. While many nurses and allied health professionals look on popular platforms like Indeed and Vivian, applying through multiple agencies can be time-consuming and repetitive.
Staff Relief makes it simpler. Our job board and mobile app put thousands of opportunities in one place. You can browse, compare, and apply to positions without juggling multiple applications or credentialing processes.
Here are a few resources to explore:
- Staff Relief Job Board & Mobile App – Your all-in-one hub for per diem, travel, and contract jobs, with a streamlined application process and dedicated support.
- Indeed – Search a wide range of listings for nursing and allied health jobs.
- Vivian Healthcare Jobs – Compare pay packages and contract details across agencies.
Ready to save time and find your next assignment faster? Start with Staff Relief’s platform for the most efficient experience
Aya Healthcare, AMN Healthcare, and Medical Solutions are some of the most respected companies in the industry offering extensive travel nursing, per diem, and rapid response assignments nationwide. As a partner, Staff Relief has access to some of the same contracts and exclusive opportunities available through Aya, AMN, and Medical Solutions. You can explore top-paying positions without having to apply separately to multiple agencies. Whether you’re interested in Aya Healthcare contracts, AMN Healthcare rapid response nursing jobs, or Medical Solutions travel nurse assignments, our team can help you compare options and secure the role that fits you best.
Choosing the right nursing agency is essential. Whether you’re evaluating Aya Healthcare reviews, AMN Healthcare pay packages, or Medical Solutions job openings, here are factors to consider:
- Transparent pay packages and benefits
- Support with licensing and credentialing
- Access to crisis response contracts and rapid response nursing jobs
- A reputation for placing nurses in top paying travel nursing companies
- Ongoing support and career development resources
Staff Relief partners with major systems and local facilities to deliver healthcare staffing solutions that prioritize both the nurse and the patient.
If you’re searching for flexible RN shifts, contract nursing jobs, or remote nursing positions, we’re here to help. From emergency department nurse jobs to radiology technologist staffing, our team can match you with assignments that fit your goals.
Connect with Staff Relief today to get personalized recommendations, compare contracts, and start your next chapter with confidence.

Pros and Cons for Working for a Nurse Staffing Agency
In today’s fast-changing healthcare landscape, more nurses are exploring flexible career paths, including per diem nursing jobs, travel nursing contracts, and remote RN positions. Whether you’re a seasoned nurse searching for higher pay or a new grad eager to explore diverse settings, working with a nursing staffing agency can be a rewarding option. But like any career move, it’s important to weigh the benefits and challenges before deciding.
Below, we break down the main pros and cons of working with a medical staffing agency in Georgia and across the Southeast, so you can make the best choice for your lifestyle and goals.
One of the top reasons nurses choose per diem nursing positions or local contract nursing is the freedom to control their schedule. Unlike full-time hospital roles, contract assignments and per diem shifts let you decide when and where you work. This flexibility is ideal if you have family commitments, are pursuing further education, or simply want more autonomy in your day-to-day life.
Agencies like Aya Healthcare, AMN Healthcare, and Medical Solutions often post weekend nursing contracts, PRN RN positions, and rapid response nursing jobs you can pick up on your terms.
If maximizing your earnings is a priority, you’ll be glad to know that contract nursing jobs and per diem shifts typically pay higher hourly rates compared to permanent staff roles. These assignments often include stipends for meals, lodging, and travel—especially for travel nurse jobs in Atlanta, Savannah, and the Florida Panhandle. Many nurses find that with smart budgeting; they can work fewer shifts while maintaining or even increasing their income.
Plus, expenses related to travel nursing—like transportation and temporary housing—are often tax-deductible, creating additional financial benefits.
For nurses who thrive on change, working with a healthcare staffing agency provides a steady stream of new experiences. You’ll build your skills across different units, such as emergency departments, inpatient care, and even specialized areas like radiology technologist jobs or diagnostic imaging. This variety not only helps you stay engaged but also makes your resume stand out to future employers.
While flexible shifts are a major perk, it’s important to recognize that per diem nursing jobs don’t always guarantee steady hours. You may have weeks packed with back-to-back assignments, followed by slower periods. In some cases, last-minute schedule changes can impact your plans. If you prefer consistency, consider long-term contract nursing jobs, which often range from 6 to 17 weeks and offer more predictable schedules.
Contract and travel nurses frequently rotate among facilities, from skilled nursing facilities to acute care hospitals. Each location has its own protocols, electronic health records, and workplace culture. While you’ll eventually become comfortable in new settings, the learning curve can feel steep, especially when starting out. Nurses who value long-term relationships with coworkers and patients may find this aspect challenging.
If you’re adaptable, resourceful, and excited by the idea of working in diverse environments, you’re well-positioned to succeed. Many RNs say contract work rekindled their passion for patient care, exposed them to innovative treatments, and expanded their professional networks.
Whether you’re interested in remote nursing jobs in Alabama, ICU travel nurse assignments in Georgia, or emergency room contracts throughout the Southeast, there’s no shortage of options through reputable agencies like Aya Healthcare, AMN Healthcare, and Medical Solutions.
Ready to explore per diem nursing positions or contract opportunities? Here are a few steps to begin:
- Research Top Agencies: Read reviews and compare pay packages, benefits, and housing support.
- Set Your Priorities: Decide what matters most—schedule flexibility, pay rate, location, or specialty.
- Prepare Documentation: Update your licenses, certifications, and resume.
- Search Nursing Jobs Online: Use platforms like Indeed, Vivian Health, and agency job boards to find assignments that match your goals.
- Ask Questions: Speak with recruiters to understand expectations, cancellation policies, and support resources.
Working with a nursing staffing agency can be an empowering way to build a flexible, well-paid, and fulfilling career. If you’re considering making a change, take time to explore your options and connect with agencies committed to supporting nurses at every step.
Explore current per diem and contract openings with Staff Relief today and discover how flexible nursing can work for you.

How to Get a High Paying Contract Nursing Job
Contract nursing offers the chance to do meaningful work, gain diverse experience, and earn competitive pay. Whether you’re pursuing contract nursing jobs, per diem nursing positions, or rapid response assignments, the key to maximizing your income is preparation and strategy.
If you’re ready to secure a high-paying contract nursing job, use these proven tips to set yourself apart and negotiate pay that reflects your expertise.
Your resume is your first impression. A clear, polished resume highlights your skills, certifications, and professional accomplishments, and it determines whether you’ll be invited to interview.
Include:
- Your nursing specialties (such as ICU, emergency department, or medical imaging)
- Certifications (like ACLS, BLS, or specialty credentials)
- Details about your experience in different care settings, such as inpatient care, skilled nursing facilities, or acute care staffing
It’s normal to have employment gaps but be ready to confidently explain them during interviews. A well-organized resume positions you as a serious professional ready for high-paying nursing contracts.
Keeping your credentials updated makes you a more attractive candidate and can improve your earning potential.
Make sure to:
- Renew essential licenses and certifications promptly.
- Consider adding specialty certifications that are in demand for travel nursing jobs and contract assignments.
- Stay up to date with immunizations required by hospitals and clinics. Being ready with all documentation can speed up onboarding and help you access crisis response nursing jobs or urgent needs contracts that often pay premium rates.
The more prepared you are, the easier it is for a nurse staffing agency or recruiter to match you with higher-paying positions.
Professional references can be the deciding factor in landing a top-paying assignment.
Employers and recruiters rely on references to verify your:
- Clinical skills
- Professionalism
- Reliability
Choose references who can confidently speak to your work ethic and performance. Positive recommendations can open the door to flexible nursing shifts, per diem contracts, and specialized roles that pay more.
Flexibility is often rewarded in the world of contract nursing.
Consider these options to boost your pay:
- Accepting night shifts or weekends, which usually come with higher hourly rates.
- Taking assignments in locations experiencing shortages, such as rural facilities or emergency department nursing jobs.
- Being open to rapid response contracts or crisis response assignments, which often offer premium compensation.
When you demonstrate a willingness to adapt, you make yourself more valuable to medical staffing agencies and healthcare employers.
In contract nursing, your reputation follows you from one facility to the next. A strong track record makes it easier to secure higher-paying contracts and preferred assignments.
Tips for maintaining a great reputation:
- Be punctual and dependable.
- Communicate clearly with staffing agencies and supervisors.
- Go the extra mile to provide excellent patient care.
Facilities are willing to pay more to bring on nurses with proven reputations for excellence.
Being a contract nurse offers countless benefits, from career variety to premium pay. To make the most of your opportunities:
- Invest time in preparing a strong resume.
- Keep certifications and immunizations current.
- Maintain excellent references.
- Stay flexible with shifts and assignments.
- Build and protect your professional reputation.
When you combine preparation with dedication, you can consistently secure high-paying contract nursing jobs that match your skills and goals.
If you’re looking for your next opportunity, Staff Relief, Inc. is here to help. We partner with hospitals, clinics, and healthcare facilities to connect nurses with the best assignments in Georgia and beyond.
Contact us today to explore available contracts and start earning what you deserve.

How to Find the Best Nursing and Allied Health Jobs in 2025
If you’re thinking about a career change this year, you’re not alone. Thousands of nurses and allied health professionals are exploring contract nursing, per diem shifts, and even remote RN jobs to gain more flexibility, better pay, and fresh experiences.
But with so many options and so many staffing agencies—how do you know where to start?
This guide will walk you through:
✅ Why more professionals are choosing contract and per diem work
✅ How to evaluate agencies and read nursing agency reviews
✅ Where to find the best nursing jobs in 2025
✅ Tips for comparing assignments and getting hired faster
The days of sticking to one hospital job for your entire career are long gone. Today’s nurses are building more dynamic, customized careers—often combining contract assignments with per diem shifts.
The benefits of contract nursing are clear:
- Higher pay compared to permanent staff roles
- Housing and travel stipends
- Bonuses for completing assignments
- The chance to build experience in specialized areas like ICU, ER, and diagnostic imaging
- Flexibility to take time off between contracts
Meanwhile, per diem nursing jobs offer even more control over your schedule. You can pick up shifts when you want—whether that means extra weekends or just a few days a month.
If you’re drawn to this flexibility, you’re in good company. Contract and per diem work have become the fastest-growing segments of healthcare employment.
Once you decide to make a change, your next step is choosing a partner to help you find assignments. But not all agencies are the same.
Before you commit, take time to read nursing agency reviews. Here’s what to look for:
- Transparency in pay packages and benefits
- Support with licensing, credentialing, and onboarding
- Access to rapid response nursing jobs and high-demand contracts
- A track record of placing candidates in the highest paying travel nursing companies
- Clear communication and responsive recruiters
At Staff Relief, we know that trust matters. As a partner of Aya Healthcare, AMN Healthcare, and Medical Solutions, we can give you access to exclusive contracts without the hassle of applying to multiple platforms.
There are dozens of websites that list healthcare jobs, but it’s easy to get overwhelmed. To save time, start with the best nursing job sites for 2025:
- Staff Relief Job Board & Mobile App – Your one-stop platform to see per diem, contract, and travel nursing jobs nationwide, including remote RN jobs and medical imaging positions.
While many agencies focus on nursing alone, allied health roles are booming, too. If you’re a technologist or imaging specialist, consider exploring:
- Radiology technologist jobs in hospitals and outpatient centers
- Diagnostic imaging careers in high-demand specialties
- Medical imaging staffing agencies that can connect you to flexible contracts
- Radiographer employment for mobile imaging services or large health systems
Staff Relief supports professionals across disciplines and can help you find medical imaging jobs near you with excellent pay and benefits.
Ready to pick up extra shifts or transition into per diem work full-time? Here are tips to get per diem nursing jobs faster:
- Keep your credentials and health records updated.
- Sign up with an agency that has real-time job listings.
- Use the Staff Relief app to get instant alerts when new shifts are posted.
- Be proactive—per diem openings often fill quickly.
Whether you want the best remote nursing jobs for RNs, the stability of contract work, or the variety of per diem assignments, 2025 is the perfect year to take control of your career.
At Staff Relief, we make it easy to:
- Access the highest paying travel nursing companies
- Compare contracts side by side
- Read verified nursing agency reviews
- Secure opportunities in radiology, imaging, and allied health
- Apply once and explore thousands of jobs nationwide
Connect with Staff Relief today, and let’s build your path forward together.

Everything You Need to Know About Travel Nurse Credentialing
Every hospital, clinic, and long-term care facility has its own standards for verifying a clinician’s qualifications and readiness to practice. Even if you’ve worked at a similar facility before, you can’t automatically carry over your credentials. Each assignment requires you to complete a credentialing and onboarding process to ensure patient safety and compliance with regulations.
Credentialing typically includes:
- Drug screening
- Health assessments
- Proof of licensure and certifications
- Background checks and reference verifications
- Competency exams
- Facility-specific training and onboarding
Many nurse managers or department leaders will schedule a phone or video call to review workflows, discuss expectations, and confirm you’ve completed all requirements before your start date.
Preparation is key. Keeping all your essential documents organized will save you time and stress whenever you accept a new assignment. Here’s what you’ll need to have ready:
- Copies of your professional license(s) and any specialty certifications (such as BLS, ACLS, PALS)
- Two valid forms of identification (e.g., driver’s license and passport)
- A record of your annual physical exam (valid for one year)
- TB test results (valid for one year)
- Drug screen results
- Immunization and titer records (MMR, Varicella, Hepatitis B, and others)
- Proof of flu vaccination (especially if starting in the fall or winter)
- COVID vaccination records if required by the facility
- Payroll forms and direct deposit information
- References and verified work history
- Competency test results (if applicable)
If you want to avoid delays, consider getting your TB test, physical, and immunizations updated while you’re applying for contracts. Staying current helps you move quickly when the right opportunity arises.
Most healthcare facilities require online assessments to verify your competency in your specialty. These assessments might include:
- Skills checklists
- Clinical scenario testing
- Electronic medical record (EMR) training modules
Once you pass these evaluations, you’ll typically complete one to two days of orientation to get familiar with the facility’s policies, documentation standards, and workflows. This process helps ensure you can provide safe, effective care from day one.
If you work in in-demand roles such as ER RN, PCU RN, CT Technologist, RRT, Surgical Tech, Mammo Tech, Home Health RN, or M/S RN, expect additional verifications and specialty-specific assessments. Facilities often have strict guidelines for these positions due to the complexity of care and the need for current certifications.
Staff Relief’s credentialing team can walk you through these specialty requirements step by step so you feel confident and prepared.
Large national agencies often have more rigid, self-directed credentialing processes. Working with a regional partner like Staff Relief provides you with hands-on support. Our team will:
- Help you track deadlines for documents and assessments
- Coordinate background checks and health screenings
- Connect you with local resources for TB testing and physicals
- Answer your questions about compliance and onboarding
This personal guidance ensures nothing falls through the cracks—and you’re always ready to step into your next assignment.
Credentialing isn’t a one-time process. Here are a few habits that can help you stay organized:
- Keep a digital folder with scanned copies of your documents
- Mark your calendar with expiration dates for your TB test, physical, and certifications
- Get your annual flu shot early if you expect to start an assignment in the fall
- Check whether your next facility requires a COVID vaccine or booster
- Keep your immunizations up to date to avoid delays
Being proactive makes you more competitive for premium travel contracts and quick-start assignments.
Navigating credentialing can feel like a lot to manage, especially if you’re juggling multiple offers. That’s why choosing the right staffing partner is so important.
Staff Relief has years of experience supporting clinicians across Georgia, Alabama, Florida, and the Carolinas. Whether you’re a first-time traveler or a seasoned professional, you’ll have a dedicated team behind you to make credentialing smooth, transparent, and stress-free.
If you’re exploring travel nursing jobs or allied health contracts in the Southeast, our team is here to help you navigate credentialing and start your next adventure with confidence. Contact Staff Relief today to learn about current opportunities and get expert support every step of the way.
Addressing Georgia’s Critical Nursing Shortage
The nursing shortage in Georgia has reached critical levels in 2025, with nearly every county—urban and rural—struggling to recruit and retain qualified healthcare professionals. This crisis isn’t just about open positions; it’s about ensuring patients receive safe, timely, and compassionate care when they need it most.
From major hospitals to long-term care facilities, healthcare organizations are urgently seeking skilled nurses, surgical techs, and allied health professionals who can step into high-demand roles and make an impact.
Several factors continue to drive Georgia’s nursing shortage:
- Rising demand for healthcare services: The state’s aging population and expanded access to care have increased the need for RNs, LPNs, and allied health professionals.
- Burnout and workforce attrition: The lingering effects of the pandemic, combined with long hours and emotional stress, are pushing many clinicians to reduce hours, retire early, or leave the field altogether.
- Education and training bottlenecks: Limited capacity in nursing schools and faculty shortages continue to constrain the pipeline of new graduates.
- Rural disparities: Non-metro counties face even steeper challenges recruiting clinicians, leaving communities with limited access to primary and specialty care.
As a result, many hospitals and clinics are leaning heavily on travel contracts, per diem staff, and flexible assignments to keep up with patient needs.
The staffing shortage has ripple effects throughout Georgia’s healthcare infrastructure:
- Hospitals are relying on travel clinicians—especially in specialties like ER RNs, PCU RNs, and Surgical Techs—to fill critical gaps.
- Skilled professionals such as CT Technologists, RRTs, Mammo Techs, and Home Health RNs remain in high demand, driving up competition and pay rates.
- Burnout among the remaining workforce leads to higher turnover, further deepening shortages.
- Patients experience longer wait times, delayed procedures, and uneven access to care, particularly in rural and underserved areas.
The result is a cycle of strain that requires strategic intervention.
While the challenges are significant, Georgia’s healthcare leaders are adopting innovative strategies to rebuild the workforce and improve retention:
1. Expanding Educational Pathways
- New state investments in nursing schools and allied health programs are increasing enrollment capacity.
- Fast-track bridge programs are helping LPNs and paramedics advance to RN licensure more efficiently.
2. Financial Incentives and Career Support
- Loan repayment and tuition reimbursement programs are helping attract graduates to high-need areas.
- Retention bonuses and flexible scheduling are becoming standard in many contracts.
3. Investing in Burnout Prevention
- More facilities are offering mental health resources and dedicated time off to protect clinician well-being.
- AI-supported scheduling tools are helping balance workloads and reduce last-minute staffing gaps.
4. Expanding Telehealth and Remote Care
- Telehealth adoption continues to grow in 2025, allowing clinicians to manage certain care remotely.
- Hybrid care models are easing staffing pressures in rural counties.
5. Embracing Flexible Staffing Models
- Short-term contracts, rapid response assignments, and per diem shifts give clinicians more options to work on their terms.
- Many clinicians are finding that a mix of travel and local assignments offers better work-life balance.
Healthcare facilities across Georgia and the Southeast increasingly rely on experienced staffing agencies to fill urgent and specialized positions. When you partner with a staffing agency that understands the local landscape, you gain access to:
- Skilled clinicians ready to step into critical roles—whether it’s an ER RN, PCU RN, CT Tech, RRT, or Mammo Tech.
- Flexible workforce solutions to manage seasonal demand and unexpected absences.
- Streamlined credentialing and onboarding to get staff in place faster.
- Insights into regional pay trends and incentives.
Staff Relief, for example, has built long-standing partnerships with hospitals, outpatient centers, and home health agencies across Georgia, Florida, Alabama, and the Carolinas, making it easier to adapt to changing needs.
If you’re considering your next step in nursing or allied health, there has never been a better time to explore opportunities in Georgia. Clinicians with experience in specialties like emergency nursing, progressive care, surgical services, medical-surgical units, and diagnostic imaging are in especially high demand.
With flexible contracts, competitive compensation, and support from experienced recruiters, you can build a career that aligns with your goals and helps meet a pressing need.
Georgia’s nursing shortage is a complex, urgent issue—but progress is happening. By investing in education, supporting the workforce, embracing innovation, and building strong partnerships, the state is working to rebuild its healthcare capacity.
If you’re a healthcare professional ready to make an impact—or a facility seeking experienced clinicians—this is the moment to take action.
Ready to explore the latest opportunities or learn how strategic staffing can help? Contact Staff Relief today and join the effort to strengthen Georgia’s healthcare system for everyone.

10 Tips for Travel Nurses
Travel healthcare is more than just an assignment, it’s an opportunity to expand your skills, explore new places, and make an impact where it matters most. Whether you’re a seasoned travel nurse, a respiratory therapist, or a surgical technologist, knowing how to navigate contracts and maximize your experience is key to success.
Here are ten essential tips every travel healthcare professional should keep in mind.
1. The Demand for Your Skills is Higher Than Ever
In 2025, healthcare facilities across the Southeast in Georgia, Alabama, Florida, and the Carolinas are experiencing critical staffing shortages. High-demand specialties like CT Tech, ER RN, Surgical Tech, RRT, PCU RN, Mammo Tech, Home Health RN, and M/S RN are seeing unprecedented opportunities.
Travel nursing jobs and allied health contracts are plentiful, but competition can be fierce for the best assignments. Staying flexible and proactive will help you secure roles that match your expertise and goals.
2. Understand Tax Implications of Travel Assignments
Many clinicians overlook how travel pay affects their taxes. Housing stipends, travel reimbursements, and per diem allowances can all impact your taxable income. It’s wise to consult a tax professional who understands healthcare contracts to ensure you’re planning ahead and taking advantage of eligible deductions.
3. Credentialing and Compliance Take Preparation
Every state has different licensure and credentialing requirements. Georgia, Florida, and the Carolinas all have their own rules around background checks and health records.
Be prepared to provide:
- A TB test (valid for 1 year)
- A current physical exam (valid for 1 year)
- Titers and immunization records
- A background check
- A drug screen
It’s smart to get your TB test, physical, and immunizations done while you’re applying so you’re ready as soon as you receive an offer. Keep your immunizations updated, including your flu shot in the fall and COVID vaccinations where required. This will prevent delays when it’s time to start your contract.
Working with a healthcare staffing agency like Staff Relief ensures you’ll have help coordinating these documents and understanding what’s required for each facility.
4. Housing Options Vary by Assignment
Some contracts include housing stipends, while others offer pre-arranged accommodations. It’s critical to understand:
- What your stipend covers
- Whether you’ll be responsible for utilities, deposits, or furniture
- How your housing affects your taxable income
If you prefer to find your own place, Staff Relief can help source local housing options and connect you to reputable providers in your assignment area.
5. Your Reputation Will Follow You
Healthcare facilities often work with the same staffing partners across regions. Showing up on time, being adaptable, and maintaining professionalism will build your reputation and make it easier to secure future assignments.
Positive references can help you access competitive roles in specialties like ER, PCU, and surgical services.
6. Flexibility is Your Superpower
The most successful travel clinicians are those who can pivot quickly. Being open to night shifts, rural contracts, or high-demand specialties often results in higher pay and priority placement.
If you’re willing to work in critical areas, you’ll find more opportunities and stronger negotiating power.
7. Pay Packages Can Be Complex
Your compensation may include:
- Base hourly pay
- Travel stipends
- Housing allowances
- Completion bonuses
Make sure you understand the full picture, not just the hourly rate. This is essential so that you can budget effectively. A reputable healthcare staffing agency will always be transparent about how your pay is structured.
8. Burnout is Real so Take Care of Yourself
Long shifts and adapting to new teams can be stressful. Protect your mental health by:
- Scheduling regular downtime between contracts
- Accessing telehealth services offered through Staff Relief for confidential support
- Staying connected to your support network
Prioritizing self-care helps you bring your best to every assignment.
9. Smaller Agencies Can Get You Into Hidden-Gem Facilities
Smaller agencies can often place clinicians into smaller community hospitals and rural facilities where patient loads are more manageable, but pay rates remain competitive. These positions are available through Staff Relief in Georgia, Alabama, and South Carolina. Only Staff Relief and one or two other boutique firms serve these facilities, so you won’t find these assignments through large national agencies like Aya, Medical Solutions, or AMN Healthcare.
10. Choosing the Right Staffing Partner Matters
Your agency isn’t just your employer, it’s your advocate. The best healthcare staffing partners:
- Have deep relationships with respected hospitals and clinics
- Offer personal support before, during, and after your assignment
Staff Relief has decades of experience supporting clinicians across the Southeast, combining local expertise with a commitment to transparency and respect.
If you’re exploring travel nursing jobs or allied health contracts in Georgia and beyond, now is the time to take the next step. With the right support and preparation, your travel career can be rewarding, sustainable, and full of growth. Contact Staff Relief today to learn about current opportunities and find the right fit for your skills and goals.

How to Choosing the Right Medical Staffing Agency
Choosing the right medical staffing agency isn’t just about finding a job—it’s about building a career with the support, transparency, and opportunities you deserve. Whether you’re looking for contract nursing jobs, travel assignments, or allied health positions, partnering with the right agency helps you feel confident every step of the way.
As a regional leader in the Southeast serving Georgia, the Carolinas, Alabama, and Florida, Staff Relief specializes in high-demand roles and offers deep local expertise to help you succeed.
Here are six essential tips to guide your search for a medical staffing agency you can trust.
1. Work with a Partner Who Knows the Region
When you’re working in states across the Southeast, you want an agency that understands the unique dynamics of each market. Regional experience matters because:
- Different states have varying credentialing and compliance requirements
- Compensation rates shift between urban and rural facilities
- Each area has its own demand for specialties, including CT Tech, ER RN, Surgical Tech, RRT, PCU RN, Mammo Tech, Home Health RN, and M/S RN assignments
Staff Relief’s recruiters have years of experience placing clinicians throughout Georgia, Alabama, Florida, and the Carolinas. This local knowledge ensures you’re matched with facilities that fit your skills, preferences, and professional goals.
2. Evaluate the Agency’s Reputation and Track Record
A medical staffing agency’s history is a strong indicator of what you can expect. Take time to:
- Explore the agency’s website to see testimonials from nurses, surgical techs, respiratory therapists, and imaging professionals
- Review social media and online platforms for authentic feedback
- Look for examples of long-term partnerships with respected hospitals, outpatient centers, and home health organizations across the Southeast
When you choose an agency that has established relationships and a reputation for consistency, you gain peace of mind that your career is in capable hands.
3. Expect Clear Communication About Pay
Transparency around compensation is crucial. Medical staffing pay packages can include:
- Base hourly rates
- Travel and housing stipends
- Bonuses
Without clarity, it’s easy to feel uncertain about what you’ll actually earn. A trustworthy agency will explain exactly how your pay is structured, whether you’re taking on a rapid response ER RN contract, a CT Tech travel assignment, or a Mammo Tech position.
At Staff Relief, we prioritize transparent communication so you can make informed decisions and feel confident in your earnings.
4. Assess Benefits and Support
The right staffing agency offers more than just placements. Look for a partner that provides:
- Credentialing and compliance support
- Guidance navigating state requirements if you’re crossing from Georgia into Florida, Alabama, or the Carolinas
- Professional development resources and scheduling assistance
Staff Relief is committed to offering comprehensive support, so you can focus on providing excellent patient care, whether you’re working in PCU, ER, surgical services, or home health.
5. Look for Joint Commission Certification
When an agency is Health Care Staffing certified by The Joint Commission, it demonstrates a commitment to quality and safety. Certification means the agency has:
- Passed rigorous evaluations of processes, compliance, and clinical standards
- Demonstrated consistent excellence in recruiting and supporting healthcare professionals
This recognition shows you’re working with an organization that meets the highest standards. This is something you can expect when partnering with Staff Relief.
6. Find the Right Fit for Your Working Style
Every agency operates differently. Some rely on automated platforms and self-service tools, while others offer more personal, one-on-one support.
Ask yourself:
- Do you want direct access to a recruiter who knows you by name?
- Would you rather work with an agency that manages credentialing and logistics for you?
- Do you prefer a more high-touch approach over an impersonal online process?
Choosing an agency that fits your communication style and values makes every assignment more rewarding. Staff Relief’s approach is personal, responsive, and focused on helping you thrive in the role that’s right for you.
When you work in specialized, high-demand fields like CT Tech, ER RN, Surgical Tech, RRT, Mammo Tech, PCU RN, Home Health RN, and M/S RN. You deserve a staffing partner who understands your expertise and advocates for your success.
The right agency combines:
- Regional knowledge of healthcare employers throughout Georgia, Alabama, Florida, and the Carolinas
- Transparent, competitive pay structures
- Robust support and credentialing assistance
- A proven reputation with hospitals and clinics across the Southeast
- Certification that demonstrates credibility
- A commitment to personal service and professional respect
With the right support you’re not just taking a job, you’re building a sustainable career.
If you’re exploring your next contract or travel assignment in the Southeast, Staff Relief is here to help. Our partnerships with respected healthcare facilities and our experience placing clinicians in high-demand specialties mean you can feel confident you’re making the best move for your future.
Contact us today to learn more about available positions and start your search with a staffing agency that puts you first.

The Cost of Nurse Turnover: A Breakdown
Poor nurse retention is a major issue for healthcare facilities, with the national registered nurse (RN) turnover rate standing at nearly 20%. According to the 2024 NSI National Healthcare Retention and RN Staffing Report, the average cost of nurse turnover is estimated to be $56,300 per every RN who leaves their job. For the average hospital, this can equate to roughly $3.9 to $5.8 million in losses per year.
Beyond the financial impacts, high turnover can also have rippling effects on company culture and patient care. In this article, we’ll break down all the costs of nurse turnover and outline strategies that can help you mitigate this issue at your facility.
Nurse turnover occurs when nursing professionals leave their jobs or the profession altogether. This can include instances in which staff are involuntarily terminated from their positions, enter retirement, or choose to leave their roles for other reasons. Some of the most common reasons why nursing professionals willingly leave their jobs include burnout, feeling underappreciated, and a lack of peer support.
Before we break down the cost of nursing turnover, it’s important to note that national nurse turnover and cost estimates often only account for RNs. While it’s difficult to estimate a turnover rate that is representative of all levels of nursing, let’s take a look at how turnover rates and costs have been reported for other types of roles:
- The cost of nurse practitioner turnover is estimated to be $85,832 to $114,919 per episode, with the average turnover rate standing at roughly 10%.
- The cost of nurse managerturnover is estimated to be between $132,00 to $228,000 per episode, with some hospitals reporting that 50% of their nurse leaders intend to leave their jobs within 5 years.
- The indirect costs of replacing one certified nursing assistant (CNA) can range from $3,000 to $6,000, with turnover rates averaging as high as 50% in nursing homes alone.
From these statistics, it’s clear that turnover costs can add up quickly if nursing professionals keep leaving their positions. But how exactly does turnover amount to millions of dollars per year? Here’s a rundown of what can contribute to both the economic and non-economic costs.
There are several ways in which frequent turnover can lead to increased operational costs for facilities. We’ll review and summarize these costs below.
Costs of Vacancies
When a nurse leaves their position, facilities must spend excess money to compensate for vacancies and understaffing. This includes the costs of advertising the opening, hiring temporary staff, and paying existing staff for overtime. Facilities may even need to close beds and defer patients, which leads to diminishing returns.
Several studies have found that these factors combined can contribute to significant losses, accounting for anywhere between 44% to 83% of turnover costs. These costs also continue to rise the longer a position stays open.
Costs of Training
Each time a facility hires a new nurse, additional resources must be spent for onboarding and training. Research has suggested that training can account for roughly 7% to 9% of turnover costs, as preceptors are often given temporary salary raises to orient new nurses.
Facilities that invest in new nurse residency programs are also estimated to incur an additional training cost of roughly $2,041 per resident. Residency programs are often used as a strategy to improve new nurse retention. But if turnover remains high for other reasons, these programs can have a lower return on investment.
Costs of Productivity Loss
Studies have also shown that initial reductions in productivity can contribute to a large proportion of losses, accounting for roughly 45% to 88% of turnover costs. This is because facilities are essentially paying two nurses to do the work of one during training periods — with some preceptorships lasting months at a time.
Additionally, there can be variations in skill level when facilities use a mix of temporary staff. This means that managers may need to spend more time overseeing care, which also contributes to reduced productivity at the leadership level.
High turnover can also impact the overall workflow and culture at a facility. These non-economic costs are important to consider since they can, conversely, lead to more turnover and create a cyclical issue over time.
Poor Teamwork
High turnover means that the entire nursing team must frequently adapt to new personalities and workstyles. Studies have shown that this can worsen communication and collaboration, impacting the overall cohesiveness of the unit. This can also make it more difficult to retain new hires, since teams may come across as unsupportive.
Lower Quality of Care
When existing staff take on increased workloads to compensate for gaps in staffing, quality of care can go down. Some studies have even shown that high turnover can significantly increase the rate of medical errors, mortality, pressure ulcers, and length of stay.
Reduced Employee Morale
The fragmented communication and increased stress resulting from high turnover can also lower staff morale. This may contribute to burnout, which can cause even more nurses to leave their jobs if staff retention and job satisfaction aren’t made a priority.
While there are many different causes of nurse turnover, studies have shown that nurses are four times more likely to voluntarily leave their positions than to get involuntarily terminated. This means that comprehensive measures at the institutional level are needed to retain staff and keep them satisfied in their roles.
Fundamentally, it’s important to engage your staff in conversations and identify the root causes of turnover at your facility. From there, you can apply more meaningful solutions that help your staff feel supported. This may include:
- Using sustainable staffing alternatives that allow for manageable workloads.
- Empowering nurses by giving them more control over their schedules and work.
- Creating a healthy work environment to prevent staff burnout.
- Providing transparent, consistent, and objective leadership.
The cost of nurse turnover can impact the operations, care quality, and culture at your facility. Need solutions that will stabilize your workforce in the long run? Get dozens of free, expert-written facility management tips and insights delivered straight to your inbox.
https://www.intelycare.com/facilities/resources/the-cost-of-nurse-turnover-a-breakdown/
KPMG’s 2017 U.S. Hospital Nursing: Labor Costs Study
This study identifies several trends and benchmarks in relation to hospital nursing labor costs in the United States. Some of the key findings are summarized below. When all costs are considered, traveling nurses appear to cost less than permanent nurses on an hourly basis. Cost data provided by hospitals indicates that the hourly, all-in cost for a full-time, permanent nurse is approximately $89. This hourly cost is higher than traveling nurses that cost approximately $83 per hour. Key costs that are after captured in this all-in measure are overtime pay, paid time off, retirement, insurance, recruiting, and payroll taxes – and these costs vary by nurse type. Additionally, the survey finds a quantifiable “hidden” cost associated with permanent nurses that is the result of non-productive labor hours, and an unquantified “hidden” cost associated with attrition and time required to fill a permanent direct care registered nurse position. Respondents to the survey indicated that traveling nurses are widely used today, representing approximately 11 % of respondent’s nursing staffs. Also, these hospitals indicated their use of traveling nurses will likely continue to grow in the future. Primary factors for this upward trend are local nursing shortages and facility growth. In all, traveling nurses appear to be a cost effective source of labor tor hospitals, and hospitals are forecasting higher usage of these nurses in the future.

2025 NSI National Health Care Retention & RN Staffing Report
With people living longer, the subsequent rise in chronic conditions and the fact that all Baby Boomers will reach retirement age by 2030, recruiting and retaining quality staff will continue to be a top healthcare issue for years to come. Last year, hospitals increased staff by adding ~304,000 employees, a 5.4% add rate. Of this, ~98,000 RNs were hired which represents a 5.6% RN add rate.
Hospital and RN turnover continue to fall but both remain slightly elevated. Nationally, the hospital turnover rate stands at 18.3%, a 2.4% decrease from CY23, and RN turnover is recorded at 16.4%, a 2.0% decrease. Registered Nurses working in pediatrics, women’s health, and surgical services reported the lowest turnover rate, while nurses working in behavior health, step down and emergency services experienced the highest.
The cost of turnover can have a profound impact on diminishing hospital margins and needs to be managed. According to the survey, the average cost of turnover for a bedside RN is $61,110, an 8.6% increase, resulting in the average hospital losing between $3.9m – $5.7m. Each percent change in RN turnover will cost/save the average hospital an additional $289,000/yr.
The RN vacancy rate also remains elevated at 9.6% nationally. While 0.3% lower than last year, over forty percent (41.8%) reported a vacancy rate of ten percent or more. The RN Recruitment Difficulty Index decreased three (3) days to an average of 83 days. In essence, it takes approximately 3 months to recruit an experienced RN, with step down and med/surg presenting the greatest challenges. Feeling financial stress, hospitals will continue to focus on controlling the high cost of labor with contract labor being a top strategy to navigate a staffing shortage. The greatest potential to offset margin compression is in the top budget line item (labor expense). Every RN hired saves $79,100. An NSI contract to replace 20 travel nurses could save your institution $1,582,000.

2024 Employer Health Benefits Survey
Employer-sponsored insurance covers 154 million nonelderly people. To provide a current snapshot of employer sponsored health benefits, KFF conducts an annual survey of private and non-federal public employers with three or more workers. This is the 26th Employer Health Benefits Survey (EHBS) and reflects employer-sponsored health benefits in 2024.

Hiring More Nurses Generates Revenue for Hospitals
Underfunding is driving an acute shortage of trained nurses in hospitals and care facilities in the United States. It is the worst such shortage in more than four decades. One estimate from the American Hospital Association puts the deficit north of one million. Meanwhile, a recent survey by recruitment specialist AMN Healthcare suggests that 900,000 more nurses will drop out of the workforce by 2027.
American nurses are quitting in droves, thanks to low pay and burnout as understaffing increases individual workload. This is bad news for patient outcomes. Nurses are estimated to have eight times more routine contact with patients than physicians. They shoulder the bulk of all responsibility in terms of diagnostic data collection, treatment plans, and clinical reporting. As a result, understaffing is linked to a slew of serious problems, among them increased wait times for patients in care, post-operative infections, readmission rates, and patient mortality—all of which are on the rise across the U.S.
Tackling this crisis is challenging because of how nursing services are reimbursed. Most hospitals operate a payment system where services are paid for separately. Physician services are billed as separate line items, making them a revenue generator for the hospitals that employ them. But under Medicare, nursing services are charged as part of a fixed room and board fee, meaning that hospitals charge the same fee regardless of how many nurses are employed in the patient’s care. In this model, nurses end up on the other side of hospitals’ balance sheets: a labor expense rather than a source of income.
For beleaguered administrators looking to sustain quality of care while minimizing costs (and maximizing profits), hiring and retaining nursing staff has arguably become something of a zero-sum game in the U.S.
But might the balance sheet in fact be skewed in some way? Could there be potential financial losses attached to nurse understaffing that administrators should factor into their hiring and remuneration decisions?
Research by Goizueta Professors Diwas KC and Donald Lee, as well as recent Goizueta PhD graduates Hao Ding 24PhD (Auburn University) and Sokol Tushe 23PhD (Muma College of Business), would suggest there are. Their new peer-reviewed publication* finds that increasing a single nurse’s workload by just one patient creates a 17% service slowdown for all other patients under that nurse’s care. Looking at the data another way, having one additional nurse on duty during the busiest shift (typically between 7am and 7pm) speeds up emergency department work and frees up capacity to treat more patients such that hospitals could be looking at a major increase in revenue. The researchers calculate that this productivity gain could equate to a net increase of $470,000 per 10,000 patient visits—and savings to the tune of $160,000 in lost earnings for the same number of patients as wait times are reduced.
“A lot of the debate around nursing in the U.S. has focused on the loss of quality in care, which is hugely important,” says Diwas KC.
But looking at the crisis through a productivity lens means we’re also able to understand the very real economic value that nurses bring too: the revenue increases that come with capacity gains.Diwas KC, Goizueta Foundation Term Professor of Information Systems & Operations Management
“Our findings challenge the predominant thinking around nursing as a cost,” adds Lee. “What we see is that investing in nursing staff more than pays for itself in downstream financial benefits for hospitals. It is effectively a win-win-win for patients, nurses, and healthcare providers.”
To get to these findings, the researchers analyzed a high-resolution dataset on patient flow through a large U.S. teaching hospital. They looked at the real-time workloads of physicians and nurses working in the emergency department between April 2018 and March 2019, factoring in variables such as patient demographics and severity of complaint or illness. Tracking patients from admission to triage and on to treatment, the researchers were able to tease out the impact that the number of nurses and physicians on duty had on patient throughput. Using a novel machine learning technique developed at Goizueta by Lee, they were able to identify the effect of increasing or reducing the workforce. The contrast between physicians and nursing staff is stark, says Tushe.
“When you have fewer nurses on duty, capacity and patient throughput drops by an order of magnitude—far, far more than when reducing the number of doctors. Our results show that for every additional patient the nurse is responsible for, service speed falls by 17%. That compares to just 1.4% if you add one patient to the workload of an attending physician. In other words, nurses’ impact on productivity in the emergency department is more than eight times greater.”
Adding an additional nurse to the workforce, on the other hand, increases capacity appreciably. And as more patients are treated faster, hospitals can expect a concomitant uptick in revenue, says KC.
“It’s well documented that cutting down wait time equates to more patients treated and more income. Previous research shows that reducing service time by 15 minutes per 30,000 patient visits translates to $1.4 million in extra revenue for a hospital.”
In our study, we calculate that staffing one additional nurse in the 7am to 7pm emergency department shift reduces wait time by 23 minutes, so hospitals could be looking at an increase of $2.33 million per year.Diwas KC
This far eclipses the costs associated with hiring one additional nurse, says Lee.
“According to 2022 U.S. Bureau of Labor Statistics, the average nursing salary in the U.S. is $83,000. Fringe benefits account for an additional 50% of the base salary. The total cost of adding one nurse during the 7am to 7pm shift is $310,000 (for 2.5 full-time employees). When you do the math, it is clear. The net hospital gain is $2 million for the hospital in our study. Or $470,000 per 10,000 patient visits.”
These findings should provide compelling food for thought both to healthcare administrators and U.S. policymakers. For too long, the latter have fixated on the upstream costs, without exploring the downstream benefits of nursing services, say the researchers. Their study, the first to quantify the economic value of nurses in the U.S., asks “better questions,” argues Tushe; exploiting newly available data and analytics to reveal incontrovertible financial benefits that attach to hiring—and compensating—more nurses in American hospitals.
We know that a lot of nurses are leaving the profession not just because of cuts and burnout, but also because of lower pay. We would say to administrators struggling to hire talented nurses to review current wage offers, because our analysis suggests that the economic surplus from hiring more nurses could be readily applied to retention pay rises also.Sokol Tushe 23PhD, Muma College of Business
For state-level decision makers, Lee has additional words of advice.
“In 2004, California mandated minimum nurse-to-patient ratios in hospitals. Since then, six more states have added some form of minimum ratio requirement. The evidence is that this has been beneficial to patient outcomes and nurse job satisfaction. Our research now adds an economic dimension to the list of benefits as well. Ipso facto, policymakers ought to consider wider adoption of minimum nurse-to-patient ratios.”
However, decision makers go about tackling the shortage of nurses in the U.S., they should go about it fast and soon, says KC.
“This is a healthcare crisis that is only set to become more acute in the near future. As our demographics shift and our population starts again out, demand for quality will increase. So too must the supply of care capacity. But what we are seeing is the nursing staffing situation in the U.S. moving in the opposite direction. All of this is manifesting in the emergency department. That’s where wait times are getting longer, mistakes are being made, and overworked nurses are quitting. It is creating a vicious cycle that needs to be broken.”
Goizueta faculty apply their expertise and knowledge to solving problems that society—and the world—face. Learn more about faculty research at Goizueta.
*Ding, Tushe, Kc, Lee: “Frontiers in Operations: Valuing nursing productivity in emergency departments.” Manufacturing & Service Operations Management 26:4:1323-1337 (2024)

Georgia could see the largest shortage of RNs by 2036
Staffing is one of the biggest issues facing ASCs. A 2023 survey from ORManager found that in the last 12 months, 56% of ASCs reported an increase in volume. Despite this success, 68% of facilities also reported having a more difficult time recruiting experienced operating room nurses.
“I think the biggest threat towards ASCs in 2023 is staffing, especially qualified, experienced staffing in all areas of an ASC, including business office, pre-op, OR (both nursing and surgical technicians), post-anesthesia care unit and recovery nurses. In addition, sterile processing technicians,” Michael Powers, administrator of Knoxville, Tenn.-based Children’s West Surgery Center, told Becker’s. “Each of these areas require a certain set of skills that are acquired and honed over time. There is increased competition, and in fact it is hard to compete with large health systems/hospitals. I am also finding that ASCs are competing in the same region against one another for the available staffing pool.”
The HRSA report highlights nurse workforce projections from 2021 to 2036 generated using the agency’s health workforce simulation.
Here are the five states with the largest projected shortages of registered nurses by 2036, per the report:
1. Georgia: 29% projected shortage
Projected vacancies: 34,800
2. California: 26% projected shortage
Projected vacancies: 106,310
3. Washington: 26% projected shortage
Projected vacancies: 22,700
4. New Jersey: 25% projected shortage
Projected vacancies: 24,450
5. North Carolina: 23% projected shortage
Projected vacancies: 31,350
https://www.beckersasc.com/leadership/5-states-facing-the-biggest-nurse-shortages-by-2036

Nursing Shortage Fact Sheet
The U.S. is projected to experience a shortage of Registered Nurses (RNs) that is expected to intensify as Baby Boomers age and the need for health care grows. Compounding the problem is the fact that nursing schools across the country are struggling to expand capacity to meet the rising demand for care. The American Association of Colleges of Nursing (AACN) is working with schools, policy makers, nursing organizations, and the media to bring attention to this healthcare concern. AACN is leveraging its resources to shape legislation, identify strategies, and form collaborations to address the shortage.
For more information including below, see attached PDF:
- Current and Projected Shortage Indicators
- Contributing Factors Impacting the Nursing Shortage
- Impact of Nurse Staffing on Patient Care
- Efforts to Address the Nursing Shortage

The cost of nurse turnover in 24 numbers
The 2024 NSI National Health Care Retention & RN Staffing Report features input from 400 hospitals in 36 states on registered nurse turnover, retention, vacancy rates, recruitment metrics and staffing strategies.
It found the average cost of turnover for one staff RN grew from January through December 2023 to $56,300, among other dollar figures and statistics that are helpful to understand the financial implications of one of healthcare’s most challenging labor disruptions.
Here are 24 numbers that illustrate the cost of nurse turnover, according to the most recent edition of the report, which is available in full here.
1. The turnover rate for staff RNs decreased by 4.6% in 2023, resulting in a national average of 18.4%. Given varying bed size, RN turnover can range from 5.6% to 38.8%.
2. The average cost of turnover for a staff RN increased by 7.5% in the past year to $56,300, with a range of $45,100 to $67,500. This is up from the average cost of turnover for an RN in 2022, which was $52,350.
3. Each percent change in RN turnover stands to cost or save the average hospital $262,500 per year.
4. The RN vacancy rate sits at 9.9% nationally. This marks an improvement, as hospitals hired an additional 153,000 RNs in 2023 and lowered the vacancy rate by 5.8%.
5. The average time to recruit an experienced RN ranges from 59 to 109 days, with the average for 2023 sitting at 86 days — nine days quicker than the year prior.
7. Every region represented in the 2024 report recorded a decrease to RN turnover, ranging from -1% to -5.1%. The South Central region saw the high end of this range while the North Central region saw the low end.
8. Over the past five years, RNs in step down, emergency services, and telemetry were most mobile with a cumulative turnover rate between 112% and 119%. “Essentially, these departments will turn over their entire RN staff in less than four and a half years,” the report states.
9. RNs in pediatrics, surgical services, and women’s health were less mobile, with 2023 turnover rates of 13.3%, 15.4% and 16.3%, respectively.
https://www.beckershospitalreview.com/finance/the-cost-of-nurse-turnover-in-24-numbers-2024

Costs and cost-effectiveness of improved nurse staffing levels and skill mix in acute hospitals
Extensive research shows associations between increased nurse staffing levels, skill mix and patient outcomes. However, showing that improved staffing levels are linked to improved outcomes is not sufficient to provide a case for increasing them. This review of economic studies in acute hospitals aims to identify costs and consequences associated with different nurse staffing configurations in hospitals.
Although more evidence on cost-effectiveness is still needed, increases in absolute or relative numbers of registered nurses in general medical and surgical wards have the potential to be highly cost-effective. The preponderance of the evidence suggests that increasing the proportion of registered nurses is associated with improved outcomes and, potentially, reduced net cost. Conversely, policies that lead to a reduction in the proportion of registered nurses in nursing teams could give worse outcomes at increased costs and there is no evidence that such approaches are cost-effective. In an era of registered nurse scarcity, these results favour investment in registered nurse supply as opposed to using lesser qualified staff as substitutes, especially where baseline nurse staffing and skill mix are low.
https://www.sciencedirect.com/science/article/pii/S0020748923001669

American Hospital Association Health Care Workforce Scan
The pandemic exacerbated existing shortages of health care workers in all roles, from clinicians to environmental and food services to admissions and scheduling. These shortages will persist well beyond the pandemic given today’s highly competitive labor market.
Record numbers of people are leaving their current jobs for new ones, new fields or new pursuits outside the job market altogether.
Despite all the difficulties, trauma and challenges they have faced, millions continue to show up and believe in their ability to make a difference in patients’ lives. Their mental and physical well-being requires tangible help and support from their leaders, and respect from the communities they serve.
The incredible challenges have also created unique opportunities to accelerate change and improve the way care is delivered, whether through technology, new care delivery approaches or multidisciplinary team models.
Ensuring the health and safety of the health care workforce – and the health and safety of the patients they care for – requires commitment at the individual, organizational and community level.

The Real Costs of Healthcare Staff Turnover
Staffing tops the list of healthcare industry challenges heading into 2023, according to polling data from healthcare advocacy group MGMA. It’s no wonder: Hospital staff turnover rates climbed as high as 26% in 2021 as workers retired due to burnout or went to work for organizations offering higher pay or better work-life balance.
For healthcare organizations, high employee turnover rates are a burden on finances and resources. Turnover costs include the expense of recruiting, hiring, and training new employees, as well as the cost of temporarily filling staffing gaps with expensive contract workers. There’s also the cost of reduced productivity as managers shift much of their attention to hiring and as new hires get up to speed. A less tangible—but still significant—turnover cost is lower employee morale as those who remain work harder to fill gaps for less pay than contract workers hired to provide temporary coverage.
Employee turnover refers to the total number of workers who leave a company over a specific period of time. Companies measure involuntary departures (layoffs and firings) and voluntary turnover (resignations) as well as the cost of replacing a given type of employee. Considering turnover can provide opportunities to replace underperformers, many employers also calculate the ideal turnover rate for their organization so managers can set specific employee retention goals. Every company has employee turnover—farsighted companies take the time to understand their turnover rate, the factors driving turnover, and what they can do to build and retain a workforce that will help achieve their organizational goals.
Key Takeaways
- Even before COVID-19, more than half of doctors and nurses reported symptoms of burnout, defined by physical and/or emotional exhaustion due to the rigors of the profession. But the pandemic shifted burnout into overdrive. During the pandemic, 93% of health workers reported experiencing stress.
- The average cost of turnover for a regular position is between six and nine months of an employee’s salary. Replacing a highly specialized healthcare professional can cost as much as 200% of the employee’s yearly salary.
- Patients notice high turnover rates when they see the impact of poor patient-to-staff ratios. They lose confidence in their healthcare provider when they don’t believe they’re receiving the best care, which can cause reputational damage.
In 2022, turnover rates for segments of the healthcare industry ranged from 19.5% at hospitals to 65% for at-home care providers to 94% at nursing homes.
This level of turnover puts a huge financial and logistical burden on healthcare providers. While COVID-19 put additional stress on the healthcare labor force, and the industry will likely feel the effects of COVID for years to come, the healthcare staffing crisis existed long before the pandemic. The following factors are also contributing to today’s healthcare worker exodus:
Inflexible, demanding schedules
Healthcare jobs are notorious for long hours and erratic schedules, and many are considered “deskless” jobs, meaning workers spend much of their time on the move. In fact, it’s estimated that nurses in hospitals walk about five miles a day.
Excessive administrative work
Fictional doctors and nurses are often depicted standing by a patient’s bedside, developing personal relationships and providing hands-on care. In reality, providers no longer have sufficient time to spend one-on-one with patients and other caregivers. Instead, they’re burdened by documentation, charting, and other administrative tasks. In 2021 doctors reported spending, on average, 15.6 hours per week on paperwork and other administrative tasks. First-year medical residents spend only about 10% of their work time face-to-face with patients, according to a study from Penn Medicine and Johns Hopkins University.
Heavy workloads
Even before COVID-19, more than half of nurses and physicians reported symptoms of burnout, according to the U.S. Department of Health and Human Services, and burnout rates have worsened over the past several years due to heavy workloads and related job stress. (A person experiencing burnout suffers from emotional exhaustion, depersonalization—a sense of detachment from oneself—and a reduced sense of personal accomplishment.) During the pandemic, researchers found that 93% of health workers were experiencing stress, 86% had anxiety, and 76% reported exhaustion.
Disconnection from managers
Healthcare workers who don’t work in a single location, such as nurses, medical assistants, and respiratory therapists, may miss out on opportunities to interact with their managers in person. Cut off from these critical personal connections, they can feel underappreciated and unseen, which makes it more likely they’ll look for a job elsewhere.
Relatively low pay
Many nurses feel they aren’t getting the pay they deserve. Even with a median annual salary of US$77,600, 66% of nurses describe pay as their No. 1 consideration when planning their next career move, according to a survey by Vivian, a healthcare hiring platform.
The direct costs of high employee turnover—the costs of recruiting, onboarding, and training new people and the costs of hiring contract staff to fill empty positions—are relatively easy to measure. The indirect costs are less quantifiable but just as burdensome; they include reduced patient satisfaction and lower employee morale. Consider these costs as you assess the impact of employee turnover on your organization.
1. Separation costs
These include severance pay, costs associated with unemployment insurance claims, payments for any ongoing benefits, and the costs associated with exit interviews and removing employees from all internal systems and directories.
2. Hiring costs
Turnover costs an organization much more than money. There’s the cost of reduced productivity when an employee leaves, and the hiring process itself can be expensive and resource intensive. It costs an employer an average of between six and nine months of an employee’s annual salary to replace them, according to the Society for Human Resource Management, and it can cost as much as 200% of the employee’s annual pay to replace a specialized healthcare professional.
3. Training costs
Even highly skilled and experienced employees need time to adapt to a new job. The healthcare industry has mandatory training and certification requirements that don’t exist in other industries. Unfortunately, many healthcare employees don’t feel they’re getting the right skills training for their rapidly changing roles, and managers and healthcare HR teams struggle to track and enforce training requirements.
4. Contingent labor costs
Understaffed healthcare organizations often resort to hiring travel or contract staff to fill workforce gaps. Unfamiliar with a facility’s policies, staff, and even its geography, contract workers can reduce overall productivity and burden full-time employees.
5. Substandard patient care
High employee turnover can lead to unsafe staff-to-patient ratios that make it hard to provide the best care. With too many patients to monitor, nurses and aides can overlook issues that slow recovery times and endanger patients. A study by the US National Institutes of Health showed that patients can lose confidence in their healthcare provider when they don’t believe they’re receiving the best care, which can tarnish the provider’s reputation.
6. Lower morale
The US healthcare industry lost more than 500,000 employees each month in 2022, according to the U.S. Bureau of Labor Statistics, and those left behind are dispirited about the future. In 2021, nearly three quarters of healthcare employees surveyed by Vivian, a healthcare hiring platform, said that workplace morale had gotten worse over the previous 12 months, and only 20% said they’re optimistic about the future of healthcare in the US. This lack of employee engagement is likely to increase employee turnover rates and reduce patient care levels, negatively impacting a healthcare organization’s reputation and financial health.
To reduce healthcare staff turnover (PDF), organizations must first improve employee well-being. People want to be compensated fairly, but beyond that, they want to be surrounded by coworkers and managers they respect. They want to feel ownership of their work lives and find work-life balance. They want systems and processes that are easy to navigate so they can focus on what matters—patient care. Here are some steps healthcare organizations can take to reduce turnover.
Managers who practice intentional hiring take the time to develop a clear job description for an open role and a clear plan for finding the right set of candidates. It may feel like this preparation lengthens the hiring process, but in the long run, it will pay off for the organization and for the candidates’ coworkers.
There are complications inherent in managing any 24/7 workforce, but these complications are compounded in healthcare by the need to have people with specific education, training, and certifications present at all times. The latest cloud-based human capital management (HCM) systems give managers visibility into staffing needs and availability and allow them to anticipate and cover surges.
Giving new employees the right tools at the start allows them to get a clear sense of the organization’s training goals and how they can fit training requirements into their workday. Dashboards that show employees what training they need, and when they need it, can improve compliance numbers while showing HR staff who’s falling behind. Cloud-based HCM systems let employees set their own training pace and measure their progress, which is especially valuable in busy workplaces where staff may have limited time to devote to training.
Healthcare professionals look for organizations that offer professional development programs beyond what’s required by law, including courses in management, communications, and ethics.
The stress of logging long hours in challenging situations is compounded by having to use inflexible, out-of-date, unconnected systems. Prospect Medical Holdings, which operates 17 hospitals and 165 medical care clinics across five states, at one time had 37 different HCM systems before successfully centralizing operations on a single cloud platform. A cloud HCM system enables employees to choose flexible schedules, sends workers notifications when it’s time to take a break, and allows management to send out regular communications that make workers feel more connected to the organization.
Healthcare-specific recruiting features in Oracle Fusion Cloud HCM help hospitals and other providers attract the best doctors, nurses, physician assistants, therapists, technicians, and support staff while giving them the tools they need to retain their accreditations and grow their expertise.
Oracle Cloud HCM’s workforce management capability enables staff to manage their schedules, sign up for shifts on their mobile devices, and block off time when they’re not available—giving them the ability to manage when and where they work. Healthcare providers can also use the cloud application’s dashboards to stay informed about patient counts and resource requirements so they can make shift changes as needed. Additionally, Oracle Cloud HCM’s employee experience platform makes it easy for hospital leaders to keep employees informed about significant organizational news and initiatives and, through pulse surveys, learn about employee concerns and needs.
Technology alone will never solve the healthcare industry’s employee turnover problem. That will take concerted efforts by healthcare organizations to focus on staff well-being, open up lines of communication, and improve the workday experience. But the right technology—easy to use, mobile friendly, and able to take on the most monotonous administrative tasks—can make a huge difference, allowing staff to focus on more complex and rewarding work: caring for patients.
Learn how the Oracle ME platform can help your organization improve the employee experience.
What is the cost of employee turnover generally?
Employee turnover costs US companies an average of $50,000 per worker, not factoring in the heavy burden on the employees who stay.
How is the cost of employee turnover calculated?
To calculate turnover costs, dig into the numbers. Calculate the cost to hire contract fill-ins for the vacant position and the cost to recruit and hire the new employee (including job postings, managerial and HR time, and background screenings). Also factor in onboarding and training costs, as well as productivity costs as the new hire ramps up. The latter is usually calculated as the cost of a new hire’s salary and benefits during their first 30 to 90 days, when they’re doing more training than work.
What is the cost of nurse turnover?
The average cost of turnover for a staff registered nurse in the US is $46,100, with an average range of $33,900 to $58,300, according to the 2022 NSI National Health Care Retention and RN Staffing Report from Nursing Solutions Inc., a national nurse recruitment agency. The average time needed to replace a nurse is about 87 days. Nurses in some fields, including emergency services and behavioral health, are leaving at accelerating rates, with cumulative turnover rates that exceed 100%. (This happens when jobs need to be filled over and over—for example, an organization with 100 employees may have 50 positions that are filled by employees who stay long term and 50 positions where lots of turnover is the norm. Each terminated employee is part of the organization’s overall turnover rate.)
https://www.oracle.com/human-capital-management/cost-employee-turnover-healthcare

The Relationship Between Nurse Staffing, Quality, And Financial Performance In Hospitals
Little evidence exists on the relationship of nurse staffing and quality with financial performance in hospitals. This study aimed to measure the relationship between nurse staffing, quality of care, and
profitability in hospitals. This study used longitudinal panel datasets from 2006 to 2010, drawn from various datasets including the American Hospital Association Annual Survey Database, Medicare Cost Report, and Hospital Compare Data. This study used the random-effects linear regression model to measure the relationship between nurse staffing, quality, and profitability. In addition, we tested a mediating effect of quality on the relationship between nurse staffing and profitability. This study found nurse staffing’s significant association with quality and profitability in hospitals. First, compared to hospitals in the lowest quintile of RNs per 1,000 inpatient days, hospitals in the higher quintiles had lower pneumonia readmission rates, and higher total profit margins, operating margins, and cash flow margins. In addition, hospitals with lower pneumonia readmission rates were found to have higher total profit margins and cash flow margins. Lastly, the current study found that the positive relationship between RNs per 1,000 inpatient days and total profit margin and cash flow margin was partially mediated by pneumonia readmission rates. In conclusion, our finding that nurse staffing is positively associated with both quality of care and profitability in hospitals suggests that the idea of hospitals responding to financial pressures by cutting RN resources with a goal of greater profitability should be called into question. The influence of lower RN staffing levels on higher profitability for hospitals is uncertain, while it is possible that RN staff reductions may compromise the quality of patient care. Keywords: nurse staffing, registered nurse, quality of care, readmission rate, profitability, total profit margin, operating margin, cash flow margin, hospital.
On a practical level, the findings on the relationship between nurse staffing, and the quality and financial outcomes in hospitals can assist nurse managers and chief executive officers in identifying the optimal RN staffing level. These findings suggest that RN staffing level may be a strong predictor of quality and profitability and that the quality may mediate the relationship between RN staffing level and profitability in hospitals. This could be of particular interest to current hospital managers because of the payment reductions for excessive readmissions embedded in the ACA, which might have significantly affected the average profitability of some service lines in their hospitals. A lesson that can be learned from the past is that hospitals may attempt staff reductions in response to increased financial pressures as a result of payment reforms. However, as the findings in this research and the literature suggest, the reduction of nursing staffs may be related to an increase in adverse effect on the quality of patient care. The analysis results of this study demonstrated that a higher RN staffing level was associated with a lower pneumonia readmission rate, while the medium level of RN staffing level (≈ 7.7 RNs per inpatient day) had the highest profitability among general and acute care, non-federal government hospitals. Staffing decisions involve balancing between labor costs and the level of care required to fulfill healthcare needs of patients (Blegen, Vaughn, & Vojir, 2008). It is a matter of choice to hospital managers to decide what would be the most effective nurse staffing strategy for their hospitals in response to the HRRP.
https://journals.scholarpublishing.org/index.php/ABR/article/view/8745

The Effects of Nurse Staffing on Hospital Financial Performance: Competitive Versus Less Competitive Markets
Hospitals facing financial uncertainty have sought to reduce nurse staffing as a way to increase profitability. However, nurse staffing has been found to be important in terms of quality of patient care and nursing related outcomes. Nurse staffing can provide a competitive advantage to hospitals and as a result better financial performance, particularly in more competitive markets
In this study we build on the Resource-Based View of the Firm to determine the effect of nurse staffing on total profit margin in more competitive and less competitive hospital markets in Florida.
By combining a Florida statewide nursing survey with the American Hospital Association Annual Survey and the Area Resource File, three separate multivariate linear regression models were conducted to determine the effect of nurse staffing on financial performance while accounting for market competitiveness. The analysis was limited to acute care hospitals.
Nurse staffing levels had a positive association with financial performance (β=3.3; p=0.02) in competitive hospital markets, but no significant association was found in less competitive hospital markets.

Optimizing the Role of Nursing Staff to Enhance Physician Productivity: One Physician’s Journey
After completing my family medicine residency a few years ago, I immediately joined a private group practice with eight family physicians and two nurse practitioners and inherited a nearly full patient panel from a retiring family physician. I naively assumed that transitioning from residency to private practice would decrease my workload and increase my quality of life, but after a hectic first year, I knew that something had to change for my professional life to be sustainable. I was spending way too much time working and could see that the complexity of practicing medicine would continue to increase in the years ahead.
I began to look for ways to cope and came across an article in Family Practice Management by Peter Anderson, MD, and Marc D. Halley, MBA.1 The article described a new model in which a physician works simultaneously with two clinical assistants – a registered nurse (RN), a licensed practical nurse (LPN), or even a capable medical assistant (MA) – allowing them to assume more responsibility for each patient encounter so the physician can focus on the patient and medical decision-making. The additional nurse responsibilities include gathering an initial history (including the history of present illness, HPI; review of systems; past medical, social, and family history, PSFH; and health habits) and then staying in the exam room to document the physician encounter, order needed tests, print handouts, send prescriptions to the pharmacy, and complete the note including the assessment and plan. By shifting many of the ancillary physician tasks to well-trained clinical assistants, the physician can focus on what he or she is uniquely trained to do – provide high-quality acute, chronic, and preventive care in the context of a therapeutic relationship. After discussing this idea with my nurse (an LPN) and practice manager, we decided to try this new model.
My nurse and I started slowly, selecting several days where we would see fewer patients, thereby allowing additional time to learn our new process. It was a significant adjustment for both of us. She was now in charge of the documentation (and thus the computer), and it became necessary for me to clearly verbalize every aspect of the visit, including the physical exam, the assessment, and the plan for treatment or additional workup (labs, imaging, medications, referrals, etc.). We used Anderson and Halley’s model as our starting point, but soon our process evolved based on our own skills and strengths, the needs of our patients, and the limitations of our office space, schedule, and electronic health record (EHR). After experimenting for a month, we were both convinced that we were ready to fully commit to this new model and decided to hire a second nurse. Because we had spent significant time fine-tuning our system, the training process for our second nurse (also an LPN) was relatively smooth, and my original nurse was able to do the bulk of the teaching.
Every new process requires some experimentation and modification in the early stages, and for our practice key adjustments occurred in the following areas:
Communication with nurses. When we first began, I would handwrite my assessment and plan for each patient encounter to ensure accuracy. Quickly, my nurses let me know that this was a waste of time. Instead, they suggested that I clearly explain each diagnosis and associated plan to the patient, and they would capture the information as I spoke. The nurses have also demonstrated that they can capture patient instructions as we discuss them, and they now typically print those instructions at the conclusion of each visit. Today it is unusual for me to type or handwrite anything during an office visit.
Access to patient data. Each of our exam rooms has a desktop computer that we use to navigate the EHR. Lab and imaging results import electronically into the EHR, as do many of our consult notes. With my nurse in the room using the computer during the office visit, I lost the ability to peruse the chart during the visit, so I began to use an iPad with our wireless Internet connection to view a read-only version of the chart. The iPad also allows me to review the history related to each problem, the problem list, and current medications without pulling my nurse away from her documentation responsibilities.
Chart review. As we progressed with our new model, I continued to gradually shift more responsibility onto my nurses’ capable shoulders. They assumed responsibility for immunization status (checking status for adults and children, administering needed vaccines, creating catchup schedules, etc.), preventive care, and even some basic chronic disease management (confirming annual diabetic eye exams and referring as needed, ordering annual lipid panels when appropriate, etc.). The nurses found that in opening a visit note, they were essentially doing a thorough chart review including reviewing, updating, and sorting the problem list; reviewing preventive care needs; sorting the medication list; reviewing and reorganizing the PFSH and health habits; starting the HPI by searching the chart for any prior tests or visits related to the chief complaint (as recorded by the front desk staff when scheduling the visit); and even starting the assessment and plan portion of the note by listing the relevant diagnoses. It was not possible to accurately complete such a chart review between patients, so my nurses agreed to arrive about an hour before our first patient each day to allow additional time for this work.
Patient check-in form. We have continually worked to implement processes that improve patient flow and efficiency during office visits. One of our more successful processes involves using a patient check-in form. Early on, it became apparent that the rooming process was a bottleneck in our patient flow because of the need to confirm problems, medications, allergies, social history, family history, habits, etc. I had asked my nurses to attempt to quickly update these at each office visit, and it turned into a time-consuming process, particularly for complex patients on multiple medications. To expedite the process, we worked with our EHR support staff to create a one-page document that lists a patient’s medications, allergies, family history, social history, health habits/risk factors, pharmacy of choice, and advance directives. These forms are printed directly from the EHR during the morning chart review and are given to the front desk staff to pass out to patients when they arrive. This allows patients to review much of their history while sitting in the waiting room and allows the nurses to address only changes that need to be made. As an added benefit, patients appreciate that we put time into prepping for their arrival rather than handing them a blank form to complete.
Patient privacy. I was concerned that having a nurse present in the exam room might be a distraction for patients or make them uncomfortable sharing sensitive information. While we did receive several questions initially about the nurse being in the room, I have been pleasantly surprised by how many patients don’t even seem to notice. There are occasional instances when it is evident that a patient would be more comfortable without a nurse present during the visit, and the nurses can usually ascertain this while rooming the patient. Overall, feedback has been amazingly positive. Rather than viewing the nurses as an intrusion, patients appreciate the additional resources that my nurses have become. They also seem to recognize that the nurses’ presence allows me to be fully focused on them, rather than trying to manage charting, test orders, referrals, and refills while providing their care.
Space, workflow, and scheduling issues. Because my colleagues were not implementing the same practice model that I was, I was careful to limit the impact on them. To create a new workspace for my second nurse, I cleared some supplies from an unused desk, purchased a new computer, purchased a new office chair, and moved an unused phone. I typically have access to only two or three exam rooms while seeing patients (the Anderson and Halley model suggests three to five exam rooms), but I have not asked for more. I have found that even with two exam rooms I am considerably more efficient under this model.
While both of my nurses participate in patient visits throughout the day, they typically have short breaks between patients and can use this time to manage phone calls, medication refills, and other peripheral nursing issues. Because of this, we have not needed to schedule additional time for the nurses to manage these tasks, although we have utilized our group’s two full-time triage nurses for support on our most hectic days.
The transition to our new model has probably been most difficult for our office manager and our group’s lead nurse. A new process was required to schedule my nurses, and it can be tedious to manage schedules when I am out or one of my nurses is out. I have just recently started training some of our other office nurses in the new model, but previously I would have to resort to my old single-nurse system if one of my two nurses was out of the office.
Ongoing improvement. To fully implement this system requires nurses who are motivated and willing to assume more ownership over each patient encounter. The nurses’ knowledge of each patient and their overall medical knowledge has grown as a result of their active participation in each visit, and they have learned by watching how I make decisions and conduct the medical workup. I also continue to teach them in a more formal manner by using interesting cases that we see, and I have learned this model requires an ongoing commitment to training. I started out meeting with my nurses for one hour each week, and even though I have been using this system for almost two years, I continue to meet with them at least twice per month. During these meetings I elicit feedback about problems or inefficiencies, provide feedback on recent chart notes, and provide teaching about changing medical standards of care. My nurses are now often the ones to identify problems and suggest appropriate changes to improve our model and the care we provide. These routine meetings have created a culture of teamwork and a continual focus on innovation – traits that will likely serve us well in the ever-changing world of medicine.
Two years into the model, we can report positive results.
Patient care statistics. The organization I work for monitors patient care data, generating physician report cards for preventive care and chronic disease management. Since implementing this new practice model, I have seen an improvement in most of my report card measures, particularly those that rely more on my nurses to complete. For example, the table below shows improvements in virtually every category of diabetes care, with a particularly large jump in the percentage of diabetes patients who have received foot exams, a task I have completely turned over to my nurses.
Since implementing my new practice model, in which nurses take greater responsibility for certain aspects of the patient visit, I have seen improvements in most of my report card measures, including those for diabetes care, shown here.
| Percentage of diabetes patients | |||
|---|---|---|---|
| Diabetes measures | Goal | Old system | New system |
| A1C > 9% | < 15% | 5% | 0% |
| A1C < 7% | > 40% | 53% | 64% |
| Blood pressure > 140/90 mm Hg | < 35% | 22% | 7% |
| Blood pressure < 130/80 mm Hg | > 25% | 53% | 64% |
| Eye examination completed | > 60% | 47% | 48% |
| Smoking status and cessation advice or treatment provided | > 80% | 98% | 98% |
| LDL > than 130 mg/dl | < 37% | 15% | 9% |
| LDL < 100 mg/dl | > 36% | 58% | 62% |
| Nephropathy assessment completed | > 80% | 95% | 95% |
| Foot examination completed | > 80% | 60% | 79% |
Finances and productivity. The costs incurred with this new model can be divided into two categories: initial startup costs and ongoing costs. I estimate that my initial startup costs were in the range of $15,000. This includes the fairly nominal cost of additional office equipment (computer, office chair, etc.) and the more significant cost of slowing down my days as I brought both nurses up to speed on the new system. The only significant ongoing cost is paying the salary and benefits of my second LPN, approximately $8,000 per quarter. This is less than you might expect because four months after transitioning to this new model, I made a personal decision to decrease my full-time equivalent (FTE) status from 1.0 to 0.75. Thus, I am not responsible for the full salary of my second nurse. The remainder of her time is allocated to other parts of the practice.
My FTE change makes it nearly impossible to calculate how my practice change has affected revenue, but I can say that my office productivity has increased. We measure productivity in terms of patient visits per half-day and average charge per patient visit, which we track based on work relative value units (RVUs). Since moving to this new system, I have seen my patient visits per half-day increase by 15 percent and my average charge (work RVU) per office visit increase by 10 percent (see the graph below). Because some of our practice costs are divided based on productivity, this increase in my productivity has led to a relatively minor, but ongoing, increase in those costs.
Under my new practice model, patient visits per half-day have increased 15 percent and work relative value units (RVUs) have increased 10 percent. These numbers reflect an eight-month average before and after changing to the new model.
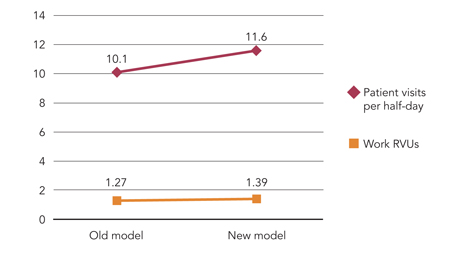
Although this new model has certainly brought an increase in expenses, I have seen a much greater increase in productivity and revenue, which has allowed me to maintain an annual income above the national median of $160,000 for a full-time family physician, despite having decreased my FTE status to 0.75.
Nurse and patient satisfaction. During this transition I have regularly asked my nurses for feedback regarding their satisfaction with our change, and when there have been frustrations or difficulties, I have done my best to work creatively with them to correct those. At this point, I am happy to report that my nurses are both very pleased with our current system. My original nurse reports that “Overall, I am very happy with the two nurse system. My favorite thing about it would be that I get to see from start to finish the entire diagnostic and treatment process. It allows me to become educated on each patient’s history and treatment plan, which in turn allows me to provide appropriate care and to be a better advocate for that patient. While working so closely together, I’ve been able to gain an understanding of how Dr. Anderson practices, and I have become more confident in myself and my own skills. Our care as a team has become significantly more thorough, and we are able to focus now on providing comprehensive care to each individual.”
Although we have not conducted a formal patient survey, the feedback we have received from patients has been almost universally positive. Patients are happy to have my undivided attention while in the exam room, they appreciate getting so much done with each office visit, and they are grateful that my increased efficiency has allowed me to be more available for same-day appointments.
This journey in restructuring my practice model has led me to a place where I am able to focus more on my patients, provide higher quality care, be more productive, and have happier employees. As physicians, we should not view ourselves as beholden to old models of care. Instead, we ought to view ourselves as empowered to institute fundamental changes to our work. The practice of family medicine is likely to get more demanding in the years ahead, and it is our opportunity and responsibility to build innovative practices that meet these demands while enabling excellent patient care, employee satisfaction, and a sustainable and meaningful personal life.

10 Best Practices for Increasing Hospital Profitability
Industry experts say that hospitals wishing to increase their profitability can focus on two key areas — reducing costs and increasing reimbursement. Here are 10 best practices for increasing hospital profitability by reducing costs and increasing revenue and reimbursement.
Because labor is the largest single expense for hospitals, it is critical that hospitals are not over- or under- staffing their facilities.
Hospitals leaders can cosider the use of flexible staffing, such as part-time or hourly employees, and adjust staffing based on patient census data. Leaders should also monitor the efficiency of this staffing by continuously reviewing benchmarking data such as hours worked per case.
Amy Floria, CFO of Goshen (Ind.) Health System, says that her facility monitors patient volume on a daily basis and adjusts staffing accordingly. “We adjust our nursing staffing every eight hours after looking at our inpatient volume and expected discharges and admits,” she says.
Kevin Burchill, a director at Beacon Partners, a healthcare management consulting firm, agrees that staffing must be adjusted daily. “The easiest thing that a hospital can do to improve profitability is for the senior management team to assume responsibility for the day-to-day performance of an organization and look at the organization’s performance in real time,” he says. “You must shift to an emphasis on the day-to-day, not pay-period to pay-period or month-to-month.”
It is important that concerns regarding efficient staffing are communicated throughout the organization and that hospital leaders work in collaboration with physicians. Donna Worsham, COO of National Surgical Hospitals, suggests that hospital leaders share staffing efficiency benchmarking data with unit managers and provide feedback regarding the productivity of the unit.
Flexible staffing is especially useful for OR nursing staff. OR managers should review clock-in times versus surgery-start times and determine if their staff is consistently arriving before a surgery actually begins. If this is the case, mangers can utilize flexible staffing to allow nursing staff to arrive later so that when surgeries run over, no overtime expenses are incurred, says Ms. Worsham.
Other facilities are saving in staffing costs by reducing benefits for full-time staff. Goshen Health System, for example, deferred merit increases, reduced paid vacation time and suspended its retirement matching program in response to the current economy, according to Goshen’s CEO, Jim Dague. Goshen reduced employee dissatisfaction in response to these cuts by soliciting employee feedback on which benefits to reduce, thereby building organizational support for the changes. In addition, Goshen’s executives took a voluntary 20 percent cut in order to help sustain the system through the recession.
Joe Freudenberger, CEO of OakBend Regional Medical Center in Richmond, Texas, agrees that staff must buy in to any reductions in hours and shifts worked that will personally affect them in order for the hospital to remain successful. He says that hospital leaders must communicate the reasoning for these changes to the staff before making them. “If we call off staff, they see it as personally hurting their income when we need to help them understand that it is actually preserving their income by maintaining the financial viability of the hospital,” he says. “It may be obvious to us that we’re calling them off because we have a significant reduction in patient volume, but we need to communicate that to them for them to understand the financial realties we face.”
Although some staffing cuts may be necessary, hospitals should be careful not to take a blanket approach to layoffs or cuts in services. Hospital leaders must take a close look at their business before making cuts.
“Don’t make the same mistake everyone else does — don’t look at bottom line, determine that you need to cut $1 million, for example, and then cut 10 percent across the board. Doing so will trim some fat but will cut meat and bone in other areas,” says Mr. Burchill.
He suggests that hospitals assess each program individually and determine which ones are what are winners and losers. “You do not want to cut areas that you should be doing more of or that are already profitable,” says Mr. Burchill.
Hospital leaders can reduce supply costs by working with vendors to improve contracts and encouraging physicians to make fiscally responsible supply decisions.
“When it comes to supply costs, you must drive this expense or the vendor will drive it for you,” says Ms. Worsham.
Hospital leaders should not shy away from approaching vendors for discounts. Goshen’s IT director recently requested a discount on the health system’s contract for IT maintenance due to current economic conditions and successfully received a discount that saved the hospital 15 percent on this contract, according to Ms. Floria.
Hospitals can also reduce supply costs be reducing the number of vendors. Goshen, for example, is in the process of reducing the number of vendors in its surgical suite and aims to eventually scale the vendors down to 4-6 companies. “This action is expected to save us at least a million dollars in supply costs,” says Mr. Dague.
Another way in which hospitals may reduce supply costs is by requiring vendors to submit purchase orders for any equipment or implants that are not included in a negotiated, written agreement with the facility. “All of our vendors sign agreements that any purchase orders must be submitted at least 24 hours before a procedure and must be approved by the materials manager or the CEO, or it’s free,” says Ms. Worsham. “If you don’t require this, vendors will drop off the invoice for a pricey piece of equipment or implant after the procedure has already taken place and walk out the back door, which can greatly hurt your profitability.”
All hospitals can benefit from tightening up the efficiency of their operating rooms, but it is especially critical that less busy facilities ensure that their ORs are used as efficiently as possible.
“Hospitals need to review block time utilization,” says Ms. Worsham. “Physicians who are assigned more time than they are using are hurting your profitability.”
Ms. Worsham suggests that hospital OR managers work directly with physicians to make OR utilization more efficient.
“When physicians’ schedules create gaps in the OR schedule, it effects a hospital’s ability to staff effectively, which can create significant labor costs for the hospital,” says Ms. Worsham.
Hospitals should work to encourage physicians to become more concerned about the costs of supplies and other activities, such as unnecessary tests and inefficient coding processes that may drive up hospital costs.
“Hospitals today have a unique opportunity to leverage physicians’ interest in having hospitals help to stabilize their incomes with the hospitals’ needs to involve physicians in cutting costs and improving quality,” says Nathan Kaufman, managing director of Kaufman Strategic Advisors, a hospital consulting firm.
Hospitals can encourage the use of products from vendors that are cost-effective, but still high quality, especially in areas such as orthopedic implants, which can be considerably costly for hospitals. In addition, experts say the use of protocol-based care can reduce costs associated with unnecessary tests or treatments.
Mr. Freudenberger says that one of the biggest mistakes hospitals make is not engaging medical staff in profitability. “Physicians have a huge role in maintaining hospital profitability, but unless you give them a reason to be concerned with a hospital’s profitability, they will make choices in what and to whom they refer services that will not consider the implications to the hospital,” says Mr. Freudenberger. “Hospital leaders should work to help medical staff understand the connection of their referrals to the hospital’s viability so that their referral decisions reflect the value they place on the hospital.”
During tough economic times, some hospitals may benefit from outsourcing or partnering with other organizations for certain services, such as food and laundry services, and even, in some cases, clinical services.
“Some hospitals see these economic times as an opportunity to outsource unprofitable services,” says Mr. Burchill.
By outsourcing certain services to more efficient providers, hospitals can share the savings with the service provider. However, hospitals must be sure to select truly efficient providers.
“Outsourcing is clearly a smart thing to do if an organization can gain greater efficiency through finding a larger-scale operation; however the provider must be more efficient than the hospital,” says Kevin Haeberle, executive vice president, HR capital, for Integrated Healthcare Strategies.
Oftentimes, hospitals outsource services such as laundry, food and nutrition, information technology or human resources because they do not have the capital to invest in the equipment upgrades or training that is needed to increase the efficiency of their internal service. In these cases, the decision to outsource may not directly be related to profitability but instead the “lacking of funds for the investment required to make current services viable,” says Mr. Haeberle. However, this decision can improve profitability in the long-run by allowing hospitals to use funds for more profitable services.
Some hospitals have also begun to outsource clinical services such as emergency room staffing and anesthesiology in an attempt to become more efficient. Because these staffing groups employ a large number of specialty physicians, they may be able to provide more efficient services, especially in clinical areas that require around-the-clock coverage where the demand for services is high.
Mike Mikhail, MD, vice president of client services for Emergency Physicians Medical Group, says that hiring an emergency department management company can help to improve the profitability of hospitals whose demand for emergency services exceeds its emergency treatment capabilities. “An emergency management group can help make the emergency department more efficient by introducing management oversight and best practices, allowing more patients to be seen and keeping others from leaving to find another hospital,” he says. “Because a majority of hospital admits come from emergency walk-ins, driving more patients through an ER will create more admits, and therefore more profit for the hospital.”
An increasing number of hospitals are joint venturing with local physicians and surgery center management companies to offer outpatient services through the development of a surgery center.
According to Clete Walker, vice president of development for Surgical Care Affiliates, hospitals are beginning to focus on the need for a comprehensive outpatient strategy and recognizing the need to partner with doctors to effectively execute on this strategy. Mr. Walker reports that he has seen an increased interest from hospitals in joint venture arrangements for outpatient services.
“More and more hospitals are realizing that their core competency is providing inpatient care; their outpatient cases are more costly per case and take up more of the physician’s and patient’s time than they do at an ASC,” he says. “As a result, hospitals are competing with physicians for outpatient cases. Hospitals with joint-venture agreements, however, do not have to compete with the physicians.”
Hospitals can leverage their standing in the community to partner with local physicians to share the revenue generated by efficient outpatient cases.
“We are in lean times, and lean times call for us to rethink our strategies,” says Mr. Walker. “It’s better for physicians, hospitals and other groups to work together to provide an efficient delivery system for patient care than for the groups to compete.”
Identifying and attracting additional physicians to bring cases to your hospital is another way that hospital leaders can increase profits. Physician-owned hospitals can bring in additional physicians as partners, while other types of facilities can recruit new physicians who are willing to perform cases at their hospitals.
“New physicians will bring in more cases and grow your profits,” says Ms. Worsham.
Ms. Worsham suggests polling your medical staff for names of local physicians to target and inviting them into the facility. During the visit, Ms. Worsham recommends that hospitals work to “wow” the target physician. “We work tirelessly to promote the services we can offer them,” she says.
When a new physician begins performing cases at one of Ms. Worsham’s facilities, that physician is assigned a concierge. “We have strong internal programs in place for this first day. A concierge is assigned to each new physician who provides them with a tour facility and walks them through every aspect of their day,” says Ms. Worsham.
Hospitals may also be able to grow case volume and profits by adding new service lines. However, hospitals need to be careful to do their homework on the expected profitability and ROI for any new lines added, especially in a market where access to the funds required to invest in new service lines may be tight.
“You have to look at what the market needs are and where you’re going to get the referrals from,” says Ms. Worsham. “Meet with local physicians and interview them about their needs and the number of cases they see that could utilize a new service.”
Hospitals should also be sure to examine the competitive landscape for any new service line.
Ms. Worsham reports that her facilities have had great success from adding a hyperbaric service line because few competitor hospitals were offering this service.
Hospitals that use hospitalists to care for patients can benefit from the more efficient care and better documentation that specialized hospitalists can potentially provide.
“A protocol-based hospitalist program can increase efficiency and help to reduce the length of stay for patients, which can increase case volume without the need for additional beds,” says Mr. Kaufman.
Hospitals should consider employing these specialists as a means to improving care and enhancing their bottom lines, according to Mr. Kaufman.
Stephen Houff, MD, president and CEO of Hospitalists Management Group, says that hospitalist groups can provide effective care to patients and possibly increase reimbursement. “Hospitalists may be the most reliable and cost-effective means available for hospital leaders to transform medical delivery in their health system,” he says. “Through shared vision, an effective hospitalist team partners with hospital leadership to improve patient safety and access, streamline care, improve patient and family satisfaction, enhance reimbursement via improved clinical documentation and provide seamless transition to post-discharge care.”
One of the most important ways that hospitals can improve their profitability is by continually evaluating and renegotiating their managed care contracts.
“Hospitals must demand their fair share of premiums from third-party payors in order to subsidize the underpayment of Medicare and Medicaid,” says Mr. Kaufman. “Hospitals need to focus on reducing their cost structure as much as possible to approach breaking even with Medicare reimbursement rates, but that only goes so far.”
Mr. Kaufman recommends that hospitals only agree to contracts that reimburse at 130-140 percent of cost. “If a facility is not big enough or strong enough to get these rates, then they should look at merging with a larger facility,” says Mr. Kaufman.
Ms. Worsham suggests that hospitals perform a profitability analysis by payor and by procedure in order to determine where a facility is losing money and identify any trends. She also suggests that hospitals evaluate older contracts due to changes in severity-based DRGs and carve out the reimbursement of implants in order to ensure they are reimbursed appropriately for the costs associated with these.
Ms. Worsham also suggests that hospitals evaluate contracts on a quarterly basis, even if the contract is not near expiring. She suggests that hospital leaders examine the contracts with the following questions in mind:
• Is revenue where we thought it would be given reimbursement rates and volume of policy holders?
• Are we being paid as agreed upon in the contract?
• Are we being paid in a timely manner?
Contracts that are determined to be “high risk” should be renegotiated. Make sure your contracts contains a material harm clause, which will allow you to readdress terms of contracts that have become financially harmful to the facility, according to Ms. Worsham. Renegotiating contracts can be very valuable — one hospital Ms. Worsham advises will gain $500,000 this year due to renegotiations.
Hospitals that focus on enacting these best practices are likely to see improvements in their profitability; however, hospitals can also benefit by using today’s economic conditions as an opportunity to improve their overarching approach to business, creating a more sustainable organization in the future.
“When profits were high, hospitals had the luxury of being sloppy in some areas; now we must run a tighter ship,” says Ms. Floria. “This will benefit the industry in the long-run.”
Hospitals can also use this opportunity to find creative solutions to problems that plague their facilities.
Goshen Health System, for example, recently enacted a program in which the hospital pays the premium required to sustain Cobra benefits for recently laid-off patients seeking care. “We are willing to be creative with our patients,” says Ms. Floria. “We pay for benefits when certain patients cannot. The revenue we receive from caring for these patients recoups this cost and provides us with additional cash flows that likely would have been uncollected or written off to charity care or bad debt.”
This idea, which was enacted during lean times to improve profitability, will continue to benefit the hospital’s bottom line, even when profitable times return.
Contact Lindsey Dunn at lindsey@beckersasc.com.